Key Takeaways
- Assessment Scoring Guide: If you exhibit 2 or more high-risk factors (e.g., history of heavy use, previous withdrawal seizures, co-occurring mental health conditions), immediate inpatient medical supervision is clinically indicated.
- Top 3 Success Factors: 1) 24/7 medical monitoring to prevent life-threatening complications, 2) Evidence-based Medication-Assisted Treatment (MAT) to stabilize neurochemistry, 3) Transitioning to a continuum of care (like PHP or IOP), which increases long-term success rates from 8% to 40-60%.
- Immediate Next Action: Press Call Now to contact a specialized, non-hospital medical detox facility to verify your insurance benefits and arrange a safe, confidential admission.
Drug Detoxification: Your First Step to Recovery
Why Medical Supervision Matters
| Risk Factor | Clinical Implication |
|---|---|
| History of heavy alcohol, opioid, or benzodiazepine use | High risk for severe physiological dependence and acute withdrawal syndrome. |
| Previous withdrawal seizures or delirium tremens | Indicates a lowered seizure threshold; requires immediate medical intervention. |
| Co-occurring physical or mental health conditions | Complicates stabilization; necessitates integrated psychiatric and medical care. |
| Use of multiple substances (Polysubstance use) | Unpredictable withdrawal timelines and compounding symptom severity. |
| Lack of a safe, supportive home environment | Increases relapse risk and danger if medical emergencies occur unsupervised. |
When you’re in the thick of drug detoxification, having medical oversight isn’t just a luxury—it’s the safety net that can mean the difference between a manageable process and a life-threatening crisis. As a professional, you already know the clinical realities. Medical detox, also called medically-managed withdrawal, means trained professionals monitor your vital signs, provide medications when needed, and are ready to act fast if complications develop. This approach works best when your withdrawal risk is high, especially with substances like alcohol or benzodiazepines, where the chance of seizures or delirium tremens can reach up to 50% in unsupervised cases7.

You may feel overwhelmed by the prospect of stepping into the patient role, but remember, you’re not alone. Yes, this is challenging, and that’s okay. Medical supervision brings reassurance—you have peers looking out for your safety, managing symptoms, and supporting you through each step. At Pacific Crest Trail Detox (PCTD), we provide this critical care in a comfortable, home-like residential environment in Milwaukie, Oregon, rather than a sterile hospital setting. Research has shown that medically-supervised detox combined with behavioral therapy increases sustained recovery rates to 40-60%, compared to only 8% for detox alone9.
If you’re supporting a colleague or loved one through this, celebrate their courage for seeking help and remind yourself that every effort toward safety and stabilization is a win. Prioritize medical supervision when withdrawal risks are high or unpredictable—your compassion and vigilance can truly save lives. Next, we’ll break down what actually happens in the body during withdrawal, so you’ll know what to expect and how to prepare.
What Happens in Your Body During Withdrawal
Assessment Tool: Recognizing Withdrawal Symptoms by Body System
- Nervous system: Anxiety, agitation, tremors, insomnia
- Digestive system: Nausea, vomiting, diarrhea
- Cardiovascular: Increased heart rate, high blood pressure, sweating
- Musculoskeletal: Muscle aches, cramps
- Psychological: Mood swings, depression, intense cravings
During drug detoxification, your body works hard to regain balance after the sudden absence of substances it’s relied on. Withdrawal happens because your brain and body have adapted to regular drug or alcohol use. When that supply stops, chemical messengers called neurotransmitters—like dopamine and GABA—swing out of balance, leading to both physical and emotional symptoms3.
For example, alcohol and benzodiazepine withdrawal can cause dangerous shifts in brain activity, sometimes triggering seizures or delirium tremens. Opioid withdrawal typically leads to intense flu-like symptoms, while stimulant withdrawal can bring deep fatigue and depressive moods5, 6. The severity and duration of symptoms depend on the substance, how long it was used, and your personal health history.
“Even though withdrawal is uncomfortable, these symptoms are signs your body is starting to recover. If you notice symptoms escalating, know that medical intervention can provide relief and prevent complications.”
This process is tough, and it’s normal to feel discouraged when symptoms are strong. Remember, every hour you make it through withdrawal is a step toward healing. Up next, you’ll get a breakdown of withdrawal timelines for different substances, so you can prepare for what’s ahead and support those in your care.
Understanding Drug Detoxification Timelines by Substance
Alcohol and Benzodiazepine Withdrawal
| Withdrawal Stage | Timeframe | Common Symptoms |
|---|---|---|
| Mild | 6–12 hours after last use | Anxiety, tremor, insomnia, mild sweating |
| Moderate | 12–48 hours after last use | Agitation, high blood pressure, rapid heart rate, mild hallucinations |
| Severe | 48–96 hours after last use | Seizures, delirium tremens, severe confusion |
When supporting someone through alcohol or benzodiazepine withdrawal, timing is everything. Unlike opioid withdrawal, these substances can trigger dangerous complications—especially in the first four days. Symptoms often begin within 6–12 hours of the last drink or dose, but severe reactions, like seizures or delirium tremens, can strike later, sometimes as late as 72–96 hours after cessation6, 7. This unpredictability is why close monitoring is so critical during drug detoxification.
Consider this route if you or your clients have a long history of heavy use, co-occurring health conditions, or have experienced withdrawal seizures before. Even seemingly mild cases can escalate quickly, so err on the side of caution and ensure a safe, medically-supervised setting. Benzodiazepine withdrawal carries an especially high risk—up to 50% of dependent individuals may experience seizures if they stop abruptly without a gradual taper7. Alcohol withdrawal can also be fatal if not managed properly, with delirium tremens carrying a mortality rate of up to 37% without treatment6.
Yes, these numbers are daunting, and it’s normal to feel concern or even fear when facing this situation. Remember, every proactive safety measure you take—regular vital checks, symptom tracking, rapid escalation if signs worsen—can save a life. Each day you make it through withdrawal is a huge victory. Now, let’s look at how opioid and fentanyl withdrawal timelines differ so you can tailor support for each substance.
Opioid and Fentanyl Withdrawal Patterns
Timeline Tool: Opioid and Fentanyl Withdrawal Milestones
- Early symptoms: 8–24 hours after last dose (anxiety, yawning, muscle aches, runny nose)
- Peak symptoms: 24–72 hours (nausea, diarrhea, dilated pupils, intense cravings, chills)
- Resolution: 5–10 days for most short-acting opioids, 10+ days for fentanyl and methadone
Opioid and fentanyl withdrawal each have unique patterns that call for careful observation and compassion. Traditional opioids like heroin and oxycodone often trigger withdrawal symptoms within 8–12 hours after last use, peaking around 1–3 days, and subsiding by day 7 to 10. Fentanyl, with its longer half-life and higher potency, tends to delay withdrawal onset until 12–24 hours after the last dose. Symptoms then peak later, often between 2–4 days, and can persist for two weeks or more5, 10.
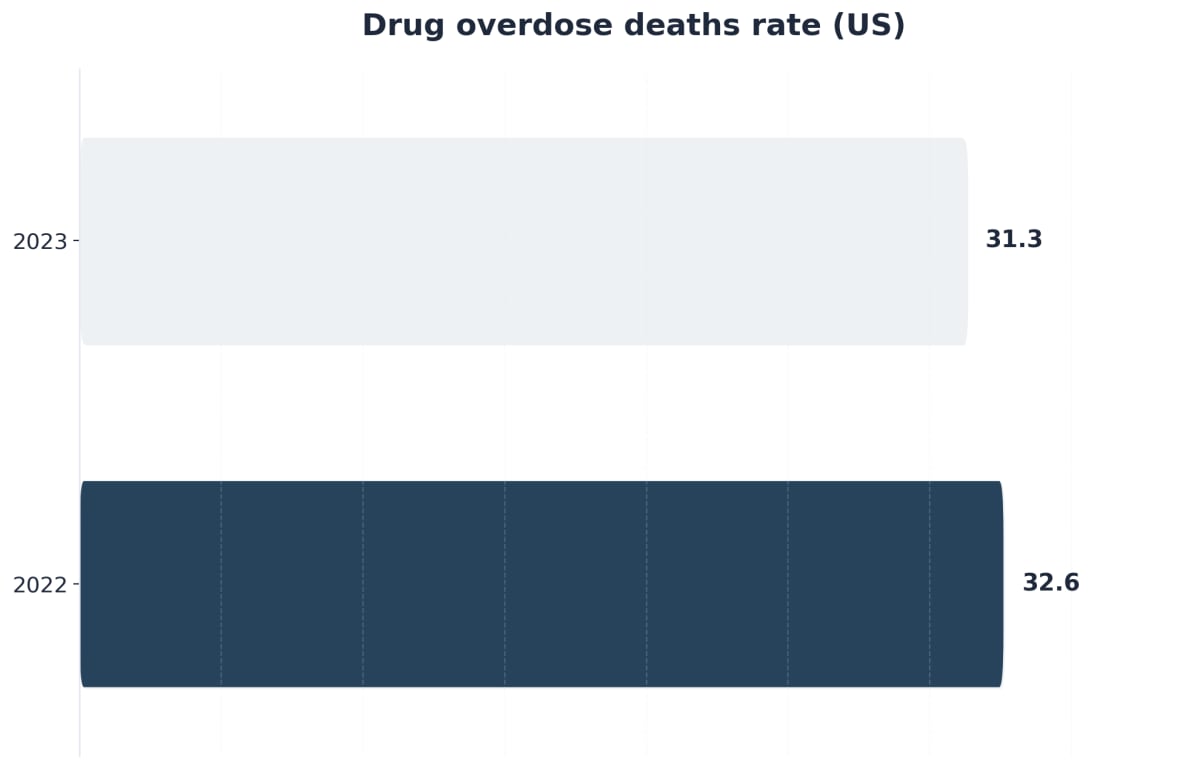
This solution fits practitioners and individuals dealing with a history of synthetic opioid use—especially those who report using fentanyl, as timelines and symptom intensity can be unpredictable. Compared to heroin withdrawal, fentanyl withdrawal is often more prolonged and marked by severe anxiety, restlessness, body aches, and gastrointestinal distress. For many, the drawn-out nature of symptoms can be discouraging, but every day someone endures withdrawal is a testament to their resilience.
It’s normal to feel challenged when navigating fentanyl or polysubstance withdrawal, but remember: each incremental improvement, such as reduced cravings or fewer sleepless nights, is meaningful progress. Medication-assisted treatment and continuous monitoring greatly increase the odds of a safer and more tolerable detox experience1. As you move forward, you’ll encounter a variety of medication-assisted treatment options that can ease withdrawal and support lasting recovery.
Medication-Assisted Treatment Options
Medications That Ease Withdrawal Symptoms
| Substance Type | Common Medications for Withdrawal Management |
|---|---|
| Opioid Withdrawal | Methadone, buprenorphine, clonidine |
| Alcohol Withdrawal | Benzodiazepines (e.g., Librium), gabapentin, carbamazepine |
| Benzodiazepine Withdrawal | Long-acting benzodiazepine taper (diazepam), adjunctive anticonvulsants |
| Supportive Agents | Anti-nausea (ondansetron), sleep aids (trazodone), antidiarrheals (loperamide) |
You know just how overwhelming withdrawal can be for those in acute drug detoxification. Medications that ease withdrawal symptoms aren’t about “replacing one drug with another”—they’re evidence-based tools that give the brain and body time to stabilize while reducing risk and distress. Methadone and buprenorphine, for example, help manage opioid cravings and pain, while also lowering overdose risk during the detox phase1. For alcohol withdrawal, benzodiazepines are standard for preventing seizures and delirium tremens, with research showing their use can be life-saving in severe cases6.
Tapering with a long-acting benzodiazepine remains the safest route for those withdrawing from short-acting benzos, minimizing seizure risk and supporting a gentler transition7. Opt for this framework when you’re supporting clients—or yourself—with high-risk histories, unpredictable withdrawal patterns, or previous detox complications. There’s no shame in leaning on medication-assisted treatment when the alternative could mean dangerous, even fatal, outcomes. Every dose that reduces tremors, anxiety, or pain is a small victory on the road to stabilization.
Next, you’ll see how to match these options to individual needs and treatment philosophies, so you can help shape a plan that truly supports long-term recovery.
Finding the Right Treatment Approach for You
Decision Tool: Matching Treatment Approaches to Patient Needs
- Is the individual at risk for severe withdrawal (history of seizures, polysubstance use, unstable mental health)? If yes, inpatient medical detox is required.
- Does the individual have strong support at home or need a structured environment? If support is lacking, residential care is optimal.
- Are there co-occurring medical or psychiatric conditions? If yes, dual-diagnosis capable facilities are necessary.
- What is the treatment philosophy: abstinence or medication-supported recovery? Align the facility’s MAT policies with these goals.
When you’re navigating drug detoxification, it’s not one-size-fits-all. The right approach depends on withdrawal risk, personal goals, and available resources. If you’re managing high-risk cases—like a history of seizures or co-occurring disorders—a medically supervised, inpatient setting often offers the greatest safety and structure. This strategy suits organizations and individuals who lack stable housing or have complex medical needs.
For others, outpatient or ambulatory detox can be effective, especially for individuals with lower-risk profiles and reliable support systems. Telehealth monitoring and flexible medication-assisted treatment plans now expand options for clients in rural or underserved areas, helping bridge gaps in care6. It’s also essential to align on recovery philosophy. Some prefer abstinence-based goals, while others thrive with ongoing medication-assisted support.
At PCTD, we utilize ERPHealth software to track statistically-significant treatment results, ensuring that your individualized care plan is actually working. The American Society of Addiction Medicine highlights the value of individualized, evidence-based care in achieving long-term recovery3. Next, you’ll see how building a strong post-detox recovery plan can make all the difference in sustaining progress.
Building Your Recovery Plan Beyond Detox
Completing medical detox is a significant professional milestone—you understand better than most how critical this step is. But as someone who works in this field, you also know the statistics: detox alone, without a structured continuum of care, yields only an 8% long-term success rate. The question isn’t whether to continue treatment, but how to access the same quality of care you’ve provided to others. Right now, your immediate priority is medical safety. Withdrawal from alcohol and benzodiazepines carries genuine life-threatening risks—seizures, cardiac complications, severe delirium.
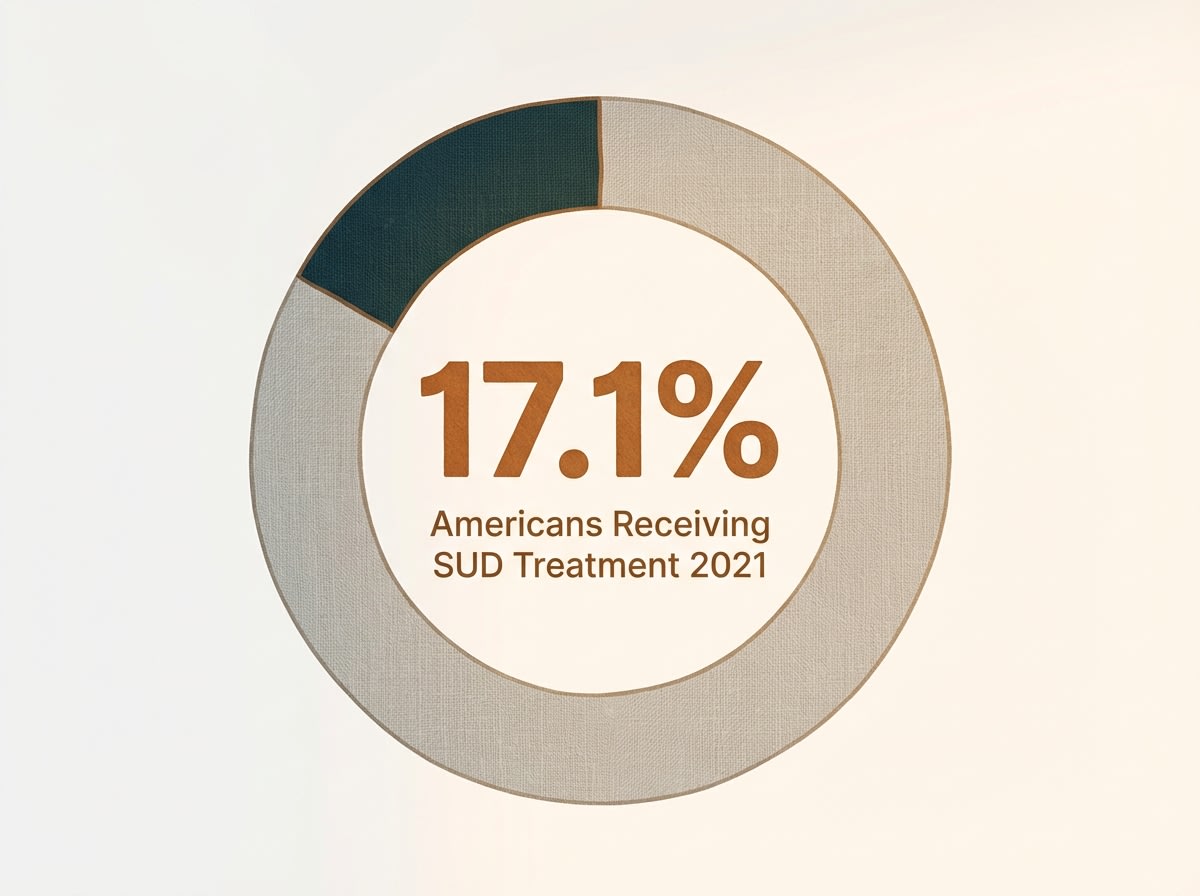
Pacific Crest Trail Detox provides 24/7 medical supervision in a home-like environment rather than a clinical hospital setting, because you deserve the same evidence-based withdrawal management and medication-assisted treatment you’d recommend for your own clients. This isn’t about willpower; it’s about physiological stabilization under proper medical protocols. Once you’re medically stable, the treatment continuum you’re familiar with professionally becomes your own roadmap.
PCTD offers the full spectrum: medical detox transitioning into partial hospitalization (PHP) for intensive daily structure, then intensive outpatient programs (IOP) that allow you to begin reintegrating professionally, followed by standard outpatient care for ongoing support. You know this progression works because you’ve seen it succeed with others. Your recovery plan will likely include the same evidence-based interventions you’ve administered: individual therapy to address underlying patterns, group therapy for peer connection (particularly valuable with other professionals who understand the unique pressures), and potentially medication-assisted treatment if you’ve been managing opioid or alcohol dependence.
These aren’t theoretical concepts—they’re proven protocols you already trust. The practical considerations matter too. PCTD’s specialized programs for professionals recognize that career concerns, licensure issues, and confidentiality are legitimate factors in your treatment planning. Family therapy can address relationships affected by your substance use. Career counseling helps navigate the professional implications you’re undoubtedly considering. Your plan will evolve as your needs change—you understand that treatment isn’t static. What’s essential is maintaining connection to the continuum of care and being honest about your needs at each stage. You’ve guided others through this process. Now it’s about accessing that same structured support for yourself, starting with the medical safety that only proper detox supervision can provide.
Frequently Asked Questions
How much does medical detox typically cost, and will my insurance cover it?
Medical detox costs can vary widely depending on the setting, length of stay, and type of care needed. While exact figures aren’t always public, inpatient drug detoxification is generally more expensive than outpatient care due to 24/7 medical supervision and support. Most private insurance plans and many employer-sponsored policies cover some or all costs for medically necessary detox services, but coverage details and out-of-pocket expenses depend on your specific plan. Medicaid and Medicare may also provide coverage for qualifying individuals. It’s common for facilities to assist with insurance verification, so reaching out for a benefits check is a helpful first step. Remember, financial worries are real, but effective coverage can make lifesaving treatment accessible for many families 8.
Can I detox at home safely, or do I really need a medical facility?
Detoxing at home may seem appealing, but for many substances—especially alcohol, opioids, and benzodiazepines—trying to quit without medical support can be dangerous or even life-threatening. Withdrawal from these drugs can cause seizures, delirium tremens, or severe dehydration, all of which require immediate medical intervention. Medical facilities are equipped to monitor vital signs, manage complications, and provide medications that ease symptoms, making the process safer and less traumatic. This approach is ideal for anyone with a history of heavy use, co-occurring health issues, or previous withdrawal complications. Remember, seeking professional help isn’t a sign of weakness—it’s prioritizing safety and giving yourself or your clients the best chance at recovery 79.
What happens if I’ve tried detox before and relapsed?
Relapsing after a previous attempt at drug detoxification can feel discouraging, but it’s not a sign of failure or weakness. Addiction is recognized as a chronic, treatable medical condition, and many people need multiple attempts before achieving lasting recovery 3. Each effort offers new insights into what support, environment, or treatments are most helpful for you or your clients. Instead of focusing on setbacks, look for patterns—did follow-up care or therapy lapse after detox? Research shows that long-term success rates jump to 40-60% when detox is paired with ongoing treatment and support, versus just 8% for detox alone 9. Every renewed attempt is a step forward and deserves acknowledgment and hope.
How do I choose between inpatient and outpatient detox programs?
Choosing between inpatient and outpatient detox programs comes down to the level of safety, structure, and support each option offers. Inpatient detox is best for those with a history of severe withdrawal, complex medical or mental health needs, or little support at home—it provides 24/7 monitoring and immediate access to medical care. Outpatient detox fits clients with stable health, reliable support systems, and a lower risk of complications, allowing them to maintain some daily routines. This approach works when managing mild to moderate withdrawal and when responsibilities like work or caregiving are a priority. Research shows both settings can be effective when matched to individual needs and risks, but inpatient care is safer for high-risk drug detoxification cases 69.
Will I be able to work or take care of my family during detox?
Whether you’ll be able to work or care for family during drug detoxification depends on the severity of withdrawal and the type of program. Inpatient detox usually requires taking time off from work and stepping away from daily responsibilities—it’s a period focused on safety and stabilization, often with 24/7 monitoring. Outpatient detox can sometimes allow you to maintain some routines, but withdrawal symptoms like fatigue, anxiety, and sleep disruption may still make working or caregiving difficult for a few days. This solution fits those with mild to moderate withdrawal and strong support at home. It’s okay if you need to step back temporarily—healing takes priority, and every step you take helps build a stronger foundation for your future 9.
What’s the difference between detox and rehab, and do I need both?
Detox and rehab serve different, but equally important, roles in recovery. Detox—formally called drug detoxification—is the initial phase focused on safely managing withdrawal and stabilizing your physical health under medical supervision. Rehab, on the other hand, refers to longer-term treatment where you (or your clients) address the psychological, social, and behavioral aspects of addiction through therapy, education, and skill-building. Most people benefit from both: detox alone has just an 8% long-term recovery rate, while adding rehab and follow-up care increases sustained success to 40–60% 9. Each phase offers its own support, and together, they build a stronger foundation for lasting change.
Your Path Forward Starts with Safe Detox
You already know the clinical reality: withdrawal from benzodiazepines and alcohol isn’t just uncomfortable—it’s medically dangerous. Seizures, cardiac complications, delirium tremens—these aren’t theoretical risks. As someone who understands the physiology, you recognize why attempting detox without medical supervision puts your life at risk. This isn’t about willpower or professional pride; it’s about medical necessity. At Pacific Crest Trail Detox, we’ve built our approach around what the data actually shows.
Our ERPHealth tracking software measures real outcomes, not just completion rates, and the numbers confirm what you likely already know: detox alone has only an 8% long-term success rate. That’s why our continuum extends from medical stabilization through partial hospitalization and intensive outpatient care. We also recognize that professionals often face co-occurring mental health challenges—depression, anxiety, trauma—that require integrated treatment, not sequential care. Our facility offers the medical oversight you need in an environment that doesn’t feel like a hospital.
We work with professionals, veterans, and LGBTQ+ individuals who need specialized understanding alongside evidence-based protocols. We accept most private insurance plans (excluding OHP) to make this critical care accessible. The path forward starts with safe medical detox because you can’t build recovery on an unstable foundation. You understand the science of withdrawal. Now it’s about applying that same clinical judgment to your own medical safety. Every step forward counts, and we are here to support you.
References
- Medications to Treat Opioid Addiction. https://www.nida.nih.gov/research-topics/treatment/medications-to-treat-opioid-addiction
- SAMHSA Medications for Substance Use Disorders. https://www.samhsa.gov/medications-substance-use-disorders
- American Society of Addiction Medicine (ASAM) Definitions and Terminology. https://www.asam.org/resources/definitions-terminology
- CDC: Substance Use Treatment and Prevention. https://www.cdc.gov/niosh/topics/emres/chemsafe.html
- StatPearls: Opioid Withdrawal (NIH/National Center for Biotechnology Information). https://www.ncbi.nlm.nih.gov/books/NBK348/
- StatPearls: Alcohol Withdrawal (NIH). https://www.ncbi.nlm.nih.gov/books/NBK470154/
- StatPearls: Benzodiazepine Dependence and Detoxification Protocols. https://www.ncbi.nlm.nih.gov/books/NBK448199/
- SAMHSA National Survey on Drug Use and Health (NSDUH). https://www.samhsa.gov/data/sites/default/files/reports/rpt39397/2021-nsduh-sae-highlights.pdf
- Journal of Addiction Medicine: Medically Supervised Withdrawal and Treatment Outcomes. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6007197/
- StatPearls: Fentanyl Withdrawal and Specific Management Protocols. https://www.ncbi.nlm.nih.gov/books/NBK557662/





