Key Takeaways
- Assess the Risk: Use our clinical indicators to determine if medical detox is required based on substance history and withdrawal severity.
- Track the Metrics: The top 3 success factors are a minimum 30-day treatment duration, active family involvement, and structured aftercare, which boost success rates from 8% to over 60%.
- Take Immediate Action: If your loved one is currently using high-risk substances like alcohol or benzodiazepines, your next step is securing a medically supervised detox bed in a supportive environment.
Why Medical Supervision Changes Everything
As a professional, you understand the clinical landscape, but when it’s your own adult child facing addiction, navigating the various types of rehabilitation suddenly feels deeply personal. You know the stakes, and you know that the foundation of any successful recovery journey begins with safety. At Pacific Crest Trail Detox (PCTD) in Milwaukie, Oregon, we believe in providing compassionate, personalized care with proven results, starting with a safe, medically supervised withdrawal process.
When Withdrawal Becomes Life-Threatening
When reviewing a chart, seeing a high CIWA-Ar (Clinical Institute Withdrawal Assessment for Alcohol) score or pressing Admit on an intake form is routine. But when it’s your family member, those clinical indicators carry a heavy emotional weight. Yes, this is challenging, and that’s okay. You are equipped to handle this.
| Risk Factor | Clinical Indicator for Medical Supervision |
|---|---|
| Substance Type | History of alcohol or benzodiazepine use |
| Medical History | Previous withdrawal seizures or delirium tremens (DTs) |
| Co-occurring Conditions | Heart, liver, or mental health conditions |
| Usage Patterns | High daily substance use or recent escalation |
| Psychological Symptoms | Severe anxiety, confusion, or hallucinations during past attempts to stop |
When withdrawal crosses the line from uncomfortable to life-threatening, your professional instincts kick in—and for good reason. Substances like alcohol and benzodiazepines can cause seizures, severe confusion, and even death without medical oversight. In fact, research shows that 10-15% of those experiencing untreated severe benzodiazepine withdrawal will have seizures, some of which can be fatal10. Alcohol withdrawal can also trigger delirium tremens, which has a high mortality rate if not managed in a medical setting5.
“Medical detox isn’t simply about comfort; it’s about safety, survival, and giving your family member a real chance at recovery.”
Consider this method if your loved one is at higher risk—meaning they have a long history of heavy use, previous dangerous withdrawals, or complex health challenges. While some types of rehabilitation may be suitable for mild cases, medical supervision is non-negotiable when any of these red flags are present. Understanding when withdrawal becomes truly dangerous helps you make informed, confident decisions. Next, we’ll look at the lasting impact of detox without proper follow-up care.
The 8% Reality: Detox Without Follow-Up
Decision Tool: 8% Recovery Rate Self-Check
- Has your loved one completed detox but not engaged in any therapy or aftercare?
- Are there no scheduled follow-up appointments or counseling sessions?
- Is the plan simply to “get clean” and hope for the best?
If you answer yes to any of these, it’s time to pause and reconsider. Research makes it clear: completing detox without ongoing care gives only an 8% chance of true recovery5. That number can feel crushing, especially when you’re working so hard to support your family member. But knowing this reality means you’re not setting anyone up for disappointment—you’re getting ahead of it.
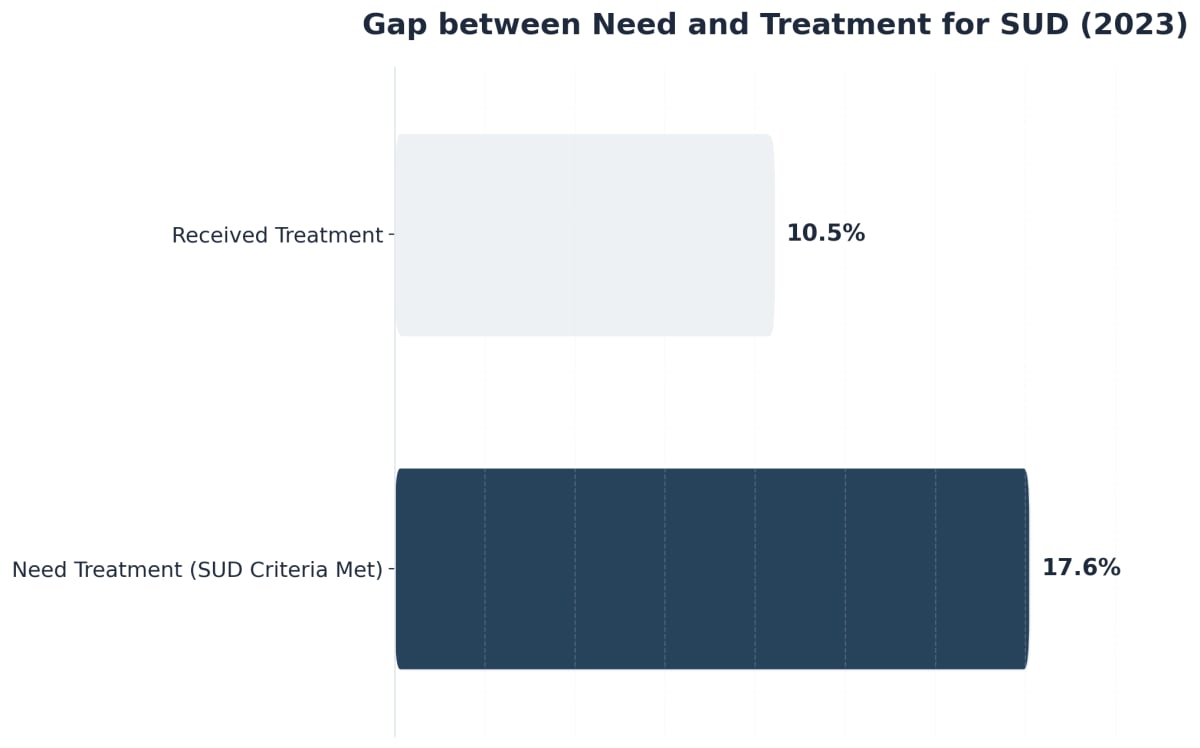
This path makes sense for those who want the fastest, lowest-commitment route, but the data is sobering. Detox alone addresses physical dependence, not the underlying mental health, triggers, or behavioral patterns that fuel relapse6. Most types of rehabilitation that stop at detox end up sending people right back into the cycle. At PCTD, we emphasize that detox is just the first step in a comprehensive continuum of care.
You’re not alone if you’ve seen this happen before. Every step toward structured aftercare, therapy, or a team-based approach dramatically boosts the odds of sustained recovery. Yes, this is challenging—and that’s okay. Every extra layer of support is a win. Up next, let’s explore which types of rehabilitation actually lead to lasting change and higher long-term success.
Three Evidence-Based Types of Rehabilitation
Medical Detox Plus Medication Support
Quick Assessment: Is Medical Detox Plus Medication Support Right for Your Loved One?
- Has there been a history of opioid or alcohol dependence?
- Have previous attempts to quit led to severe withdrawal symptoms?
- Is there co-occurring mental health or chronic pain?
- Are cravings and relapse risk high, even after detox?
For families and professionals supporting adults through recovery, medical detox paired with medication support is one of the most rigorously proven types of rehabilitation. Medical detox means supervised management of withdrawal—especially important for substances like alcohol, opioids, or benzodiazepines, where withdrawal can be dangerous. Medication support, often called medication-assisted treatment (MAT), uses FDA-approved medicines such as buprenorphine, methadone, or naltrexone to reduce cravings and prevent relapse, especially with opioid and alcohol use disorder8.
This solution fits situations where safety, stability, and relapse prevention are top priorities. For example, if you’ve watched a loved one cycle through repeated detox attempts or struggle to maintain progress, research shows MAT can cut illicit opioid use in half and slash overdose deaths by 90% compared to counseling alone8.
In typical settings, medical detox requires a time investment of 3 to 10 days. Depending on insurance coverage, out-of-pocket costs can range from $2,000 to $5,000 for this acute phase, while ongoing medication support and counseling may extend for months or longer depending on individual progress6. Staffed by medical professionals, this approach requires access to licensed providers and ongoing monitoring—but it can be the difference between short-term relief and real, sustainable recovery. Next, we’ll look at residential programs that integrate therapy, structure, and community as another powerful option.
Residential Programs With Integrated Care
Decision Checklist: Is a Residential Program With Integrated Care Right for Your Situation?
- Has your loved one struggled to maintain sobriety after previous outpatient or short-term programs?
- Are there co-occurring mental health conditions or a history of trauma?
- Does the home environment increase relapse risk due to stress or limited support?
- Is 24-hour supervision needed for medical, safety, or behavioral reasons?
Residential programs with integrated care represent one of the most structured and supportive types of rehabilitation available. These programs offer a safe, substance-free environment where clinical and therapeutic services—including medical care, counseling, group therapy, and peer support—are all provided under one roof. The day-to-day routine, community connection, and intensive therapy help stabilize individuals during their most vulnerable periods.
This approach works best when those with moderate-to-severe addiction or complex co-occurring disorders require more than outpatient care can provide. At PCTD, we offer a home-like residential environment rather than a clinical hospital setting, which helps clients feel safe and respected while receiving rigorous medical care.
Research shows that completing residential treatment, followed by step-down outpatient or aftercare, leads to 60-70% sustained abstinence at 12 months—a significantly higher rate than detox or counseling alone9. Typical residential stays last 28-90 days and require a commitment of time and resources, but the payoff is often a stronger foundation for long-term recovery.
Consider this route if your loved one needs a break from old triggers, consistent clinical oversight, or a holistic, team-based approach that addresses both physical and psychological healing. Up next, we’ll explore how to match treatment intensity with individual recovery needs.
Matching Types of Rehabilitation to Recovery Needs
Assessing Co-Occurring Mental Health Factors
Co-Occurring Factor Assessment: Quick Screening Tool
- Does your loved one have a diagnosis of depression, anxiety, PTSD, or bipolar disorder?
- Are there recent episodes of self-harm, severe mood swings, or suicidal thoughts?
- Has prior rehab failed due to untreated mental health issues?
- Is there a history of trauma or chronic stress contributing to substance use?
You know that recovery is rarely a straight path—especially when mental health and addiction collide. Co-occurring disorders (also called dual diagnosis) mean someone faces both substance use disorder and at least one mental health condition at the same time. Untangling these challenges is complex, and treating only one piece usually leads to setbacks.
Research shows that nearly 7.7 million people in the U.S. experience co-occurring addiction and mental health disorders, and outcomes dramatically improve when both are addressed together in treatment7. This strategy suits families and professionals who have seen repeated relapses or worsening symptoms when mental health gets ignored. Integrated treatment models, which combine psychiatric care, therapy, and substance use counseling, offer a measurable increase in recovery rates compared to programs that focus on addiction alone6.
Supporting a loved one through this requires patience and a team of specialists—typically including medical staff, therapists, and case managers. Yes, it’s a challenging road, but every bit of progress matters, and each coordinated step forward is a win. Next, let’s see how outpatient programs can provide flexible support for ongoing recovery.
Outpatient Programs for Sustained Progress
Outpatient Program Fit Guide: Quick Considerations
- Has your loved one completed detox or residential treatment and now needs step-down support?
- Is there a stable home environment and reliable transportation to appointments?
- Can daily routines accommodate regular therapy, medical check-ins, and group sessions?
- Is ongoing work or family engagement a priority during recovery?
Outpatient programs are one of the most flexible types of rehabilitation for supporting long-term progress. These models allow participants to attend therapy, counseling, and sometimes medication management appointments while living at home. The structure can range from highly intensive—like our Partial Hospitalization Program (PHP) or Intensive Outpatient Program (IOP) at PCTD—to standard outpatient care with less frequent visits.
Opt for this framework when individuals have already stabilized medically and need ongoing accountability without the disruption of leaving work or family behind. Research confirms that outpatient care, when used as part of a larger recovery continuum, is associated with improved engagement and long-term abstinence—especially when paired with aftercare and family involvement6.
You’re showing courage by supporting ongoing growth, even when life keeps moving around you. Every step forward counts! Next, we’ll examine which treatment factors actually drive long-term success rates and sustained recovery.
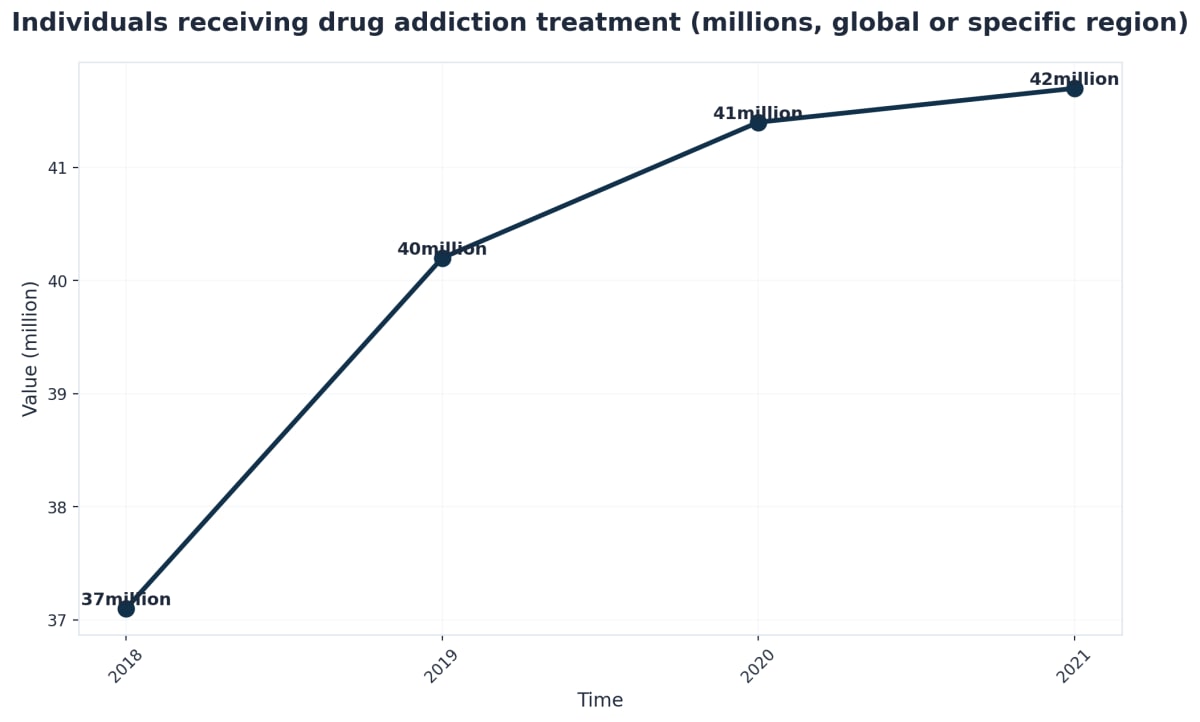
What Produces 40-60% Long-Term Success Rates
Duration, Engagement, and Aftercare Impact
Progress Checklist: Is Your Loved One’s Treatment Setting Up Long-Term Success?
- Is the total treatment duration at least 30 days?
- Are therapy appointments regular and actively attended?
- Does the plan include aftercare or step-down support?
- Is there ongoing check-in with providers post-discharge?
Staying engaged in care—well beyond the initial detox—is where real change happens. Research consistently finds that the most effective types of rehabilitation sustain 40-60% recovery rates at 12 months, but only when treatment lasts at least 30 days, includes consistent engagement, and builds in aftercare4. This isn’t just a matter of keeping busy; ongoing involvement in therapy and alumni groups helps your loved one manage triggers, navigate setbacks, and stay grounded as life gets complicated again.
Prioritize this when you are committed to more than a quick fix. Shorter programs or inconsistent attendance often leave gaps that relapse can fill. At PCTD, we differentiate ourselves through measured outcomes using ERPHealth software to track statistically-significant treatment results, ensuring that engagement translates into real-world success.
When you encourage and structure longer, connected care—including aftercare and routine progress check-ins—you’re not just hoping for the best; you’re giving recovery its strongest shot. Yes, it takes extra coordination and patience, but every follow-up appointment or aftercare group attended is a win worth celebrating. Next, let’s look at how family involvement and peer support networks can further boost these long-term success rates.
Family Involvement and Alumni Support Systems
Family and Alumni Involvement Tool: Strengthening the Recovery Network
- Are you invited to participate in therapy or educational sessions?
- Is your loved one engaged in a peer or alumni group post-treatment?
- Do you have access to family support resources or coaching?
- Are milestones and setbacks openly discussed within your support network?
You know that supporting recovery is not a solo project. The most effective types of rehabilitation recognize that long-term success hinges on weaving family and peer support directly into the process. Research highlights that when family members actively participate in therapy, education, or structured support, relapse rates drop and engagement rises6. Alumni programs—where individuals connect after formal treatment—offer ongoing inspiration, accountability, and a place to celebrate progress or ask for help during setbacks.
This approach is ideal for families eager to stay involved without taking over, and for professionals who want to foster independence while still offering a safety net. Family and alumni systems create a sense of belonging and shared purpose, making it easier for your loved one to reach out instead of slipping back into isolation. Every check-in call, group meeting, or honest conversation is a win—yes, even the tough ones. You’re building trust, hope, and resilience together. Next, you’ll see how to use these principles in practical steps for the first 30 days of recovery.
Frequently Asked Questions
How do you choose between residential and outpatient treatment when both seem appropriate?
When both residential and outpatient treatment seem appropriate, start by weighing the intensity of support needed and the daily environment your loved one will return to. Residential programs offer 24-hour clinical care and a break from outside triggers, making them a strong fit for those with moderate-to-severe addiction or unstable home situations. Outpatient programs, on the other hand, work well when someone has a safe, supportive home and can reliably attend therapy and medical appointments. Research suggests that matching the setting to the individual’s needs—rather than defaulting to one model—leads to better outcomes for all types of rehabilitation6. Talk openly with your care team; there’s no shame in reassessing as needs change.
What’s the typical cost difference between treatment models, and does insurance coverage vary?
The cost difference between treatment models can be significant, with residential programs generally requiring more resources than outpatient care. Residential types of rehabilitation involve 24-hour supervision, housing, meals, and intensive therapies, which increases total expense compared to programs where clients live at home and attend scheduled sessions. Insurance coverage often varies based on plan details and medical necessity assessments. Most private insurance will cover both residential and outpatient treatment if criteria are met, but out-of-pocket costs and coverage limits can differ. Always check with your insurer—many families find that comprehensive treatment is more accessible than they first assume due to expanded behavioral health mandates6.
How long does it take to see measurable progress in a comprehensive treatment program?
You can expect to see measurable progress within the first 30 days of a comprehensive treatment program, especially when it combines medical care, therapy, and aftercare support. Research shows that programs lasting at least a month—rather than just a few days of detox—are linked to significantly higher recovery rates, with many individuals showing improved mood, engagement, and reduced cravings by week four4. Most types of rehabilitation require ongoing participation beyond that first month for the best results, but celebrating early wins can help keep motivation high. Recovery is a process, and seeing real change takes patience and encouragement.
Can someone transition from residential to outpatient care, or does switching programs reduce effectiveness?
Absolutely, transitioning from residential to outpatient care is not only possible—it’s often encouraged as part of proven types of rehabilitation. Research confirms that moving from a structured, 24-hour setting to step-down outpatient care does not reduce effectiveness when the transition is carefully planned and supports are in place. In fact, individuals who complete residential treatment and then engage in ongoing outpatient or aftercare see 60-70% sustained abstinence at 12 months, which is substantially higher than those who stop treatment abruptly9. This approach works best when your loved one is ready for more independence but still needs regular therapy and support. Every thoughtfully managed transition is a step forward on the path to lasting recovery.
What happens if your loved one refuses medication-assisted treatment but needs medical detox?
If your loved one refuses medication-assisted treatment but still needs medical detox, they can still receive safe, supervised withdrawal care. Medical detox focuses on stabilizing the body and managing acute withdrawal symptoms—even without follow-up medications for cravings or relapse prevention. In these cases, the care team may use comfort medications, close monitoring, and supportive therapies to ensure safety, especially for substances like alcohol or benzodiazepines where withdrawal can be dangerous10. While medication-assisted treatment improves long-term outcomes, the right types of rehabilitation always respect patient choice and prioritize immediate medical needs first. Open communication and ongoing support can keep the door open for future treatment options.
How do you evaluate if a facility’s outcomes data is credible and not just marketing?
Evaluating a facility’s outcomes data starts with asking for clear, third-party-validated statistics on recovery rates, treatment completion, and post-discharge follow-up—not just testimonials or broad claims. Credible facilities will reference peer-reviewed research benchmarks, such as 40-60% sustained recovery rates at 12 months for evidence-based types of rehabilitation4. Look for transparency about how outcomes are measured (e.g., using standardized tools, regular follow-ups), and whether data accounts for all clients, not just those who finish treatment. This approach works best when you request details on definitions of “success” and ask about independent audits or participation in national data registries. Trust grows when facilities openly share both strengths and areas for improvement.
Is telehealth-based treatment as effective as in-person care for ongoing recovery support?
Telehealth-based treatment has become a valuable tool for ongoing recovery support, especially when access or transportation is a barrier. For many, virtual therapy, medication management, and support groups offer flexibility and convenience that can keep momentum strong between in-person visits. Evidence shows that for mild to moderate cases, telehealth can deliver outcomes comparable to traditional care—provided the platform is secure and patients stay engaged4. However, severe addiction or unstable home environments may still require the structure and supervision of in-person programs. This approach is ideal when you need to bridge gaps in care or maintain continuity during transitions. Every positive connection—whether virtual or face-to-face—counts toward progress.
Your Next 30 Days: Building a Recovery Pathway
You know what evidence-based treatment looks like. You’ve probably recommended it to countless families. But when it’s your own adult child, that professional knowledge can feel both like a blessing and a burden—you understand exactly what’s at stake, and exactly how critical the right care pathway is.

Here’s what comprehensive recovery looks like at PCTD: It starts with medically supervised detox in a home-like residential setting—not a clinical hospital environment—where your loved one’s withdrawal is monitored 24/7 by trained medical staff. This is especially crucial for high-risk substances like benzodiazepines and alcohol, where withdrawal can be life-threatening without proper supervision.
From there, we transition seamlessly into our continuum of care: medication-assisted treatment (MAT) when clinically appropriate, followed by our Partial Hospitalization Program (PHP) for intensive daily support, then our Intensive Outpatient Program (IOP) as they rebuild independence, and finally our aftercare and alumni services that provide ongoing connection. We accept most insurance (excluding OHP) to make this pathway accessible.
You already know the statistics—detox alone has only an 8% success rate without follow-up care. That’s why we track measured outcomes using ERPHealth software, providing statistically-significant data on treatment results rather than relying on anecdotes. Each phase builds on the last: medical stabilization creates the foundation, evidence-based therapy addresses underlying patterns, and structured aftercare reinforces lasting change.
It’s the same continuum you’d design yourself, delivered with the personalized attention and compassion your family deserves. You know what quality addiction treatment looks like. Your loved one deserves nothing less—and you deserve the peace of mind that comes from proven, comprehensive care.
References
- SAMHSA 2023 National Survey on Drug Use and Health – Key Highlights. https://www.samhsa.gov/data/sites/default/files/reports/rpt35325/NSDUH-2023-highlights.pdf
- Principles of Drug Addiction Treatment: A Research-Based Guide (NIDA). https://nida.nih.gov/publications/principles-drug-addiction-treatment-research-based-guide-third-edition
- American Society of Addiction Medicine (ASAM) – Definition and Criteria for Addiction. https://www.asam.org/quality-care/definition-of-addiction
- The Effectiveness of Addiction Treatment: A Review of the Research (NIH/PMC). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3969807/
- CDC – Substance Use and Addiction Overview. https://www.cdc.gov/substance-use/about.html
- NIDA – Treatment and Recovery. https://www.drugabuse.gov/publications/drugs-brains-behavior-science-addiction/treatment-recovery
- National Alliance on Mental Illness (NAMI) – Co-Occurring Disorders Information. https://www.nami.org/Get-Involved/Awareness-Events/Mental-Health-Month
- Medication-Assisted Treatment for Opioid Addiction: Outcomes in the United States (NIH). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4062895/
- Residential Treatment Outcomes for Adolescents and Young Adults (NIH/PubMed). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3181988/
- Benzodiazepine Withdrawal Management and Medical Detoxification (NIH/PMC). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6632961/





