Key Takeaways
- Never skip medical supervision: Unmanaged withdrawal is dangerous; always ensure 24/7 medical oversight during detox.
- Look beyond detox: Detox alone has an 8% success rate; a full continuum of care is essential for lasting recovery.
- Demand measurable results: Choose facilities that track outcomes using data, not just promises.
- Golden Rule: Sustainable recovery requires treating the whole person through a seamless, evidence-based continuum of care.
Why Choosing the Right Addiction Recovery Center Matters Now
Quality addiction treatment requires more than clinical protocols—it demands measured outcomes, personalized care pathways, and a therapeutic environment that supports genuine healing. When you are evaluating an addiction recovery center for your loved one, the distinction between adequate and excellent care becomes critical. In a field where detox alone yields just an 8% success rate without comprehensive follow-up, you need a partner you can trust.
Effective treatment centers demonstrate their commitment through verifiable results. At Pacific Crest Trail Detox (PCTD) in Milwaukie, Oregon, we track outcomes using ERPHealth software, providing statistically-significant data that validates our clinical approach.
“Recovery is not a destination, but a continuous journey of healing that requires the right environment and unwavering support.”
This outcomes-focused methodology ensures that every element of care—from medically supervised detox through our continuum of partial hospitalization programs (PHP), intensive outpatient programs (IOP), and standard outpatient services—contributes to sustainable recovery rather than simply program completion.
The treatment environment itself shapes recovery potential. Our home-like residential setting creates a therapeutic atmosphere distinct from hospital-based programs. This approach combines the medical rigor essential for high-risk detox cases—particularly alcohol and benzodiazepine withdrawal—with the warmth and dignity that support psychological healing.
Personalization extends beyond clinical customization to recognizing the specific contexts that influence recovery. Our specialized programs for LGBTQ+ individuals, veterans, and professionals address the unique challenges these populations face. For those requiring medication-assisted treatment (MAT), we integrate MAT as part of comprehensive care rather than as a standalone intervention. Co-occurring mental health disorders receive integrated treatment, recognizing that sustainable recovery addresses the whole person.
Mistake 1: Ignoring Medical Supervision
The Hidden Dangers of Unsupervised Detox
Unsupervised detox might seem, on the surface, like a quick route to sobriety, but the risks beneath are serious—and sometimes deadly. When withdrawal from substances like alcohol or benzodiazepines isn’t monitored by medical professionals, complications can escalate quickly. Seizures, heart problems, and severe dehydration are just a few dangers families have seen when detox happens without proper oversight.
One startling fact: drug overdose is a leading cause of injury-related death in the United States, and unmanaged withdrawal can directly contribute to this toll5. Beyond the physical dangers, there’s the emotional distress your loved one may face alone. The fear and discomfort of withdrawal can push even the most motivated person to give up or relapse.
| Detox Approach | Medical Oversight | Risk Level | Outcome Potential |
|---|---|---|---|
| Unsupervised (“Cold Turkey”) | None | Extremely High (Seizures, Cardiac Issues) | Low (High relapse rate) |
| Medically Supervised (PCTD) | 24/7 Nursing & Physician Support | Managed & Mitigated | High (Stabilization for next steps) |
As a parent and a professional, you know that dignity and safety matter just as much as clinical outcomes. The absence of medical supervision isn’t just a gap in care—it’s a risk to life and hope. To prevent these outcomes, always prioritize a facility that offers 24/7 medical support and evidence-based withdrawal management. Ask about staff credentials, emergency protocols, and how individual risks are assessed. Your advocacy ensures your loved one receives care that values both their safety and their future.
What Proper Medical Care Actually Looks Like
Proper medical care during detox isn’t just about having a nurse nearby—it’s about building a safety net that covers every risk, both obvious and hidden. When you evaluate a program, you want to see a clear structure: 24/7 medical supervision, individualized assessment protocols, and immediate access to emergency interventions. This isn’t about paranoia—it’s about being realistic and proactive.
Here’s what effective care actually looks like in practice:
- Comprehensive Assessment: Every person receives a medical and psychological evaluation at admission. This identifies not just substance use history, but underlying health issues, mental health disorders, and unique withdrawal risks2.
- Continuous Monitoring: The center’s medical staff—ideally including physicians experienced in addiction medicine—monitor vital signs, withdrawal symptoms, and mental health status around the clock3.
- Evidence-Based Interventions: Medications, such as those used in medication-assisted treatment (MAT), are available to ease withdrawal, manage cravings, and reduce relapse risk. These protocols follow the latest clinical guidelines, not a one-size-fits-all approach2.
- Emergency Readiness: There’s a plan for rapid response if complications arise, with staff trained in advanced life support and protocols for safe transfer to higher levels of care if needed6.
When a center combines these elements, families experience relief—knowing that their loved one’s dignity and safety are respected every step of the way. Every high-quality facility should make this level of care the norm, not the exception.
Mistake 2: Settling for Detox-Only Programs
Why 8% Success Rates Should Concern You
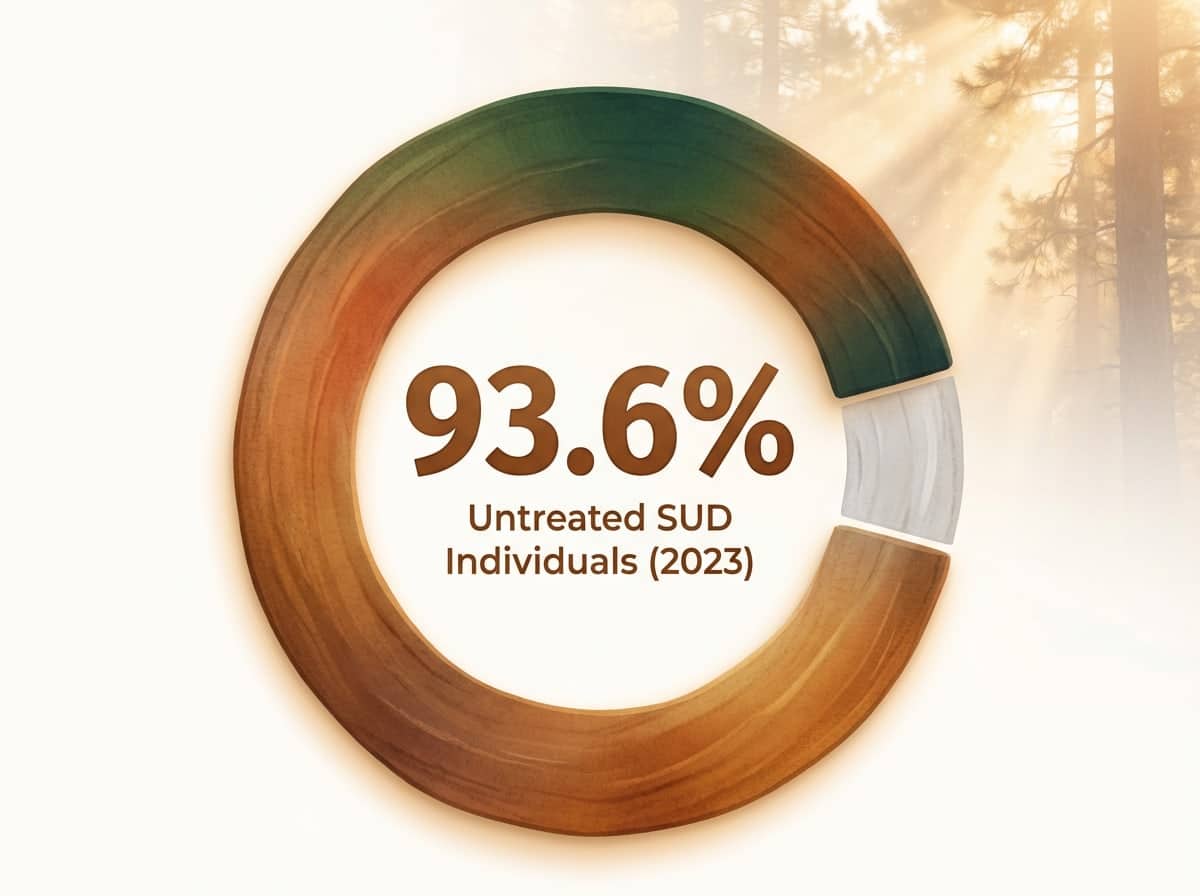
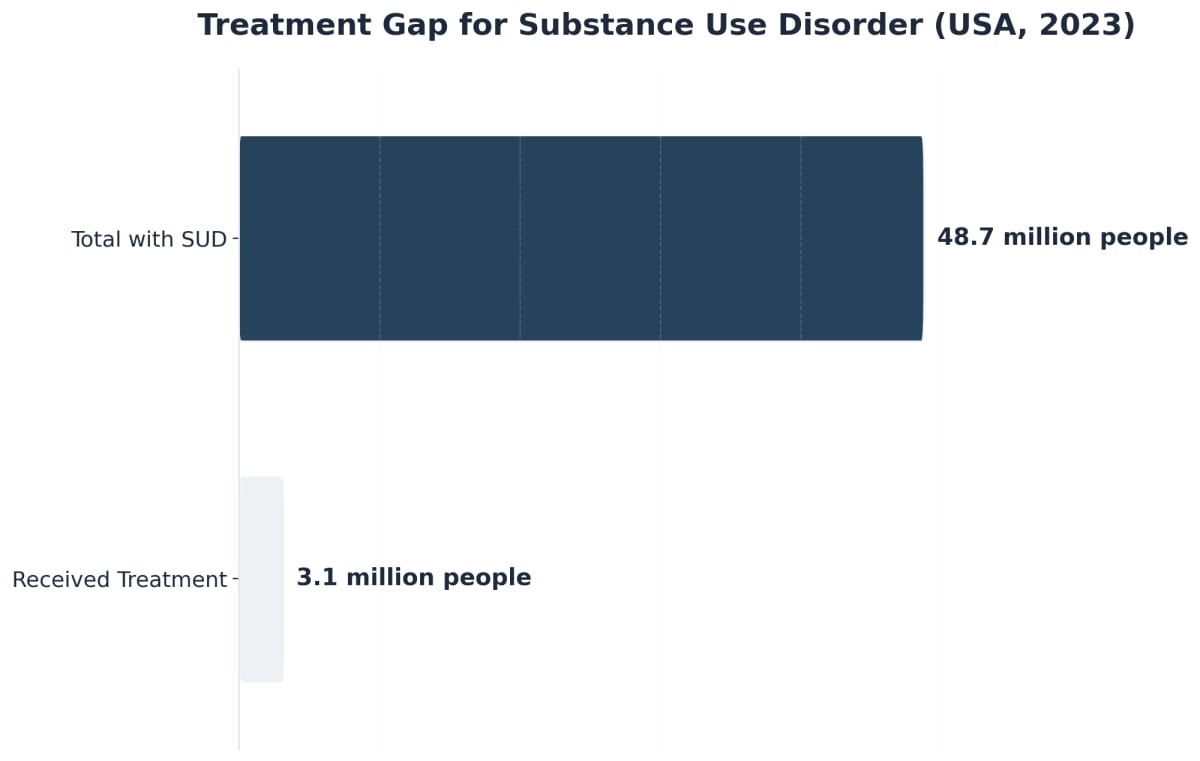
Imagine pouring every ounce of hope into a detox-only program, only to see your loved one relapse within weeks. That heartbreak is all too common. Research shows that detox without ongoing care succeeds for just 8% of individuals—leaving 92% at risk for relapse or worse9. For parents who are also professionals, this number is more than a statistic; it’s a warning sign that short-term fixes rarely bring long-term change.
Why is the success rate so low? Detox deals only with the immediate physical withdrawal, not with the mental, emotional, or social challenges that drive substance use. Without follow-up counseling, medication-assisted treatment, and structured aftercare, most people return to old habits. It’s like sending someone home after surgery without rehab or pain management—progress fades fast without ongoing support.
What should you do instead? (Click to expand)
Prioritize a facility that provides a clear path from detox through outpatient care and aftercare. Ask about their approach to continuity: Does the team include therapists, doctors, and peer support? Are treatment plans personalized and regularly updated? Confirm that aftercare is part of the program, not an afterthought.
Every layer of support helps your loved one build real, lasting change. Yes, it’s tough to advocate for more than the minimum—but every step forward makes a difference. Keep pressing for whole-person care that honors both safety and hope.
Building a Real Continuum of Care
It’s easy to hope that detox alone will solve the problem, but as you know, real recovery is a journey, not a single event. The biggest missed opportunity comes when families stop at detox, missing out on the comprehensive support that drives lasting change. Imagine your loved one finally taking that first brave step—only to have the system drop them right back where they started. This is why building a continuum of care matters so much.
Here’s how you can help ensure a true continuum of care for your loved one:
- Start with a Team Approach: Choose a facility where medical staff, therapists, and peer support work together from day one. This team should meet regularly to update the treatment plan based on your loved one’s needs.
- Insist on Individualized Planning: Look for documentation of a step-by-step plan that covers detox, therapy, outpatient services, and aftercare. One-size-fits-all doesn’t work—plans must evolve as your loved one progresses2.
- Prioritize Aftercare: Confirm that structured aftercare—like alumni groups, peer mentoring, or ongoing therapy—is a required part of the program, not just a suggestion. Research shows that aftercare participation increases recovery rates by up to 60% compared to detox alone9.
- Monitor Progress: Ask how outcomes are tracked and how families stay involved. Ongoing communication means you’ll spot setbacks early and celebrate every win together.
When you demand this level of continuity, you’re empowering your loved one to build resilience and hope at every stage. Next, we’ll see why outcome tracking is the key to knowing which centers deliver on their promises.
Mistake 3: Overlooking Outcome Tracking
The Problem with Unmeasured Treatment
Picture this: your loved one completes a program, but you have no idea if the treatment actually worked. This is the reality when a facility doesn’t measure or share outcomes. Without data, families and professionals are left hoping for the best—never truly knowing if the care provided led to real progress. When outcomes aren’t tracked, patterns of relapse, dropout, or incomplete recovery can go unnoticed and unaddressed.
For professionals like you, not having clear results is frustrating and can even put your advocacy efforts at risk. Why does this happen? Many facilities focus on process—admissions, group sessions, discharge plans—without pausing to ask, “Is our approach making a difference?” National standards require outcome tracking for behavioral health accreditation, yet not all programs hold themselves accountable to these benchmarks6.
Research confirms that only about 8% of people succeed long-term in programs that don’t emphasize follow-up and measurable results9. What can you do? Always ask how the center measures success. For example, you might ask them to provide their ERPHealth data reports or press Ctrl + P to print their latest outcome statistics for your review. Look for transparent reporting on treatment completion, relapse rates, and ongoing recovery. Centers that value transparency empower you to make informed decisions and advocate for continuous improvement.
Evidence-Based Programs That Prove Results
It’s easy to feel overwhelmed by the promises every facility makes, but the real difference comes from programs rooted in evidence and tracked outcomes. Centers that focus on proven, science-backed therapies—like cognitive-behavioral therapy, medication-assisted treatment (MAT), and integrated mental health care—deliver measurable progress for families seeking lasting change2, 7.
The strongest programs don’t just claim success; they show it by sharing data on treatment completion, relapse rates, and ongoing engagement after discharge. Here’s how you can spot a program that truly delivers:
- Accreditation & Standards: Look for accreditation by The Joint Commission or CARF, as these facilities must meet strict requirements for safety, staff training, and outcome tracking. Accreditation is linked to 20-30% higher completion rates7.
- Transparent Outcome Reporting: Ask to see real numbers on recovery rates, how often clients maintain sobriety, and what aftercare participation looks like. Choose a center that reviews outcomes regularly and uses this data to improve care6.
- Individualized, Adaptive Care: Strong centers adjust treatment based on regular progress checks, not fixed timelines. This flexibility supports dignity, hope, and better results for your loved one2.
Every step toward evidence-based care is a win for families and their loved ones. Next, we’ll tackle your most pressing questions about finding and evaluating quality treatment options.
Frequently Asked Questions
What should you do if your loved one has already started treatment at a facility without proper medical supervision?
If your loved one has already begun treatment at a facility without proper medical supervision, your first step is to stay calm and act quickly but thoughtfully. Open a direct conversation with the facility’s leadership and request a detailed explanation of their medical protocols—ask specifically about staff qualifications, emergency procedures, and how they handle withdrawal complications. If you learn that 24/7 medical supervision or physician oversight is lacking, advocate for a transfer to an addiction recovery center with accredited medical care, as medically unsupervised detox can increase the risk of serious complications or relapse 2. Trust your instincts and remember: prioritizing safety is a win, not a setback. Every decision you make in this moment helps protect your loved one’s life and future.
How can you verify if a treatment center is properly accredited and licensed?
To verify if a treatment center is properly accredited and licensed, start by asking directly for proof of accreditation from recognized organizations like The Joint Commission or CARF. These accreditors set strict standards for safety, staff training, and quality, and their approval is linked to 20-30% higher treatment completion rates 7. Next, check with your state’s health department or licensing board to confirm the center’s current license status. Most reputable addiction recovery centers display accreditation certificates visibly and are transparent about their compliance. Always trust your instincts—if a facility hesitates to share this information, consider it a red flag. Your persistence ensures your loved one’s care meets the highest standards.
What questions should you ask about medication-assisted treatment during facility tours?
When touring an addiction recovery center, ask direct questions about medication-assisted treatment (MAT). Start by asking which FDA-approved medications they offer for opioid, alcohol, or other substance use disorders. Confirm whether MAT is available throughout the program, not just during detox. Request details about how individual eligibility for MAT is determined and who prescribes and monitors these medications—ideally, a physician certified in addiction medicine. Inquire about how MAT is integrated with counseling and ongoing support, since research shows that combining medication and behavioral therapy leads to better outcomes 2. You’re helping set your loved one up for long-term success by ensuring MAT is a supported, evidence-based option.
How do you know if a center can handle co-occurring mental health disorders alongside addiction?
To determine if an addiction recovery center can truly handle co-occurring mental health disorders alongside addiction, ask if they provide integrated treatment—meaning both conditions are addressed at the same time, not in separate silos. Look for mental health professionals on staff (such as licensed therapists or psychiatrists) and ask about experience with dual diagnoses like depression, anxiety, PTSD, or bipolar disorder. The center should offer evidence-based therapies tailored to both substance use and mental health needs. Research shows that integrated care leads to better recovery outcomes for people with co-occurring disorders, compared to treating one issue at a time 8.
What insurance coverage questions should you ask before committing to a treatment center?
Before committing to an addiction recovery center, ask for a clear, itemized list of which services your loved one’s insurance covers—this should include detox, outpatient, counseling, and aftercare. Clarify what your deductible, co-pays, and any possible out-of-pocket maximums will be. Request written confirmation that the center is in-network and find out if prior authorization is needed for admission or specific treatments. Ask how denied claims or unexpected costs are handled and whether they assist with appeals. These questions help prevent costly surprises and ensure your loved one can access all levels of needed care 10.
How can you tell if a facility’s aftercare program is comprehensive enough for long-term success?
To gauge if an aftercare program is truly comprehensive, look for clear structure and accountability. An effective addiction recovery center should offer ongoing counseling, peer support groups, relapse prevention planning, and alumni or family engagement opportunities. Ask whether there’s a written aftercare plan tailored to your loved one’s needs and if progress is tracked over time. Research shows that people who participate in structured aftercare have 40-60% higher rates of long-term recovery than those who do not 9. Don’t hesitate to request examples of alumni success stories or see data on continued engagement. Every added layer of support moves your loved one closer to lasting success.
Your Loved One Deserves Proven Care at an Addiction Recovery Center
The continuum matters more than the starting point. While medical detox provides critical stabilization—particularly for life-threatening alcohol and benzodiazepine withdrawal—the transition from acute care into structured recovery programming determines long-term outcomes. Pacific Crest Trail Detox’s approach integrates detox with immediate access to partial hospitalization programs (PHP) and intensive outpatient programs (IOP), creating seamless progression rather than treatment gaps where relapse risk peaks.
Specialized programming addresses what generalized treatment misses. Veterans process trauma differently than civilians. LGBTQ+ individuals face unique stressors that generic protocols overlook. Professionals require scheduling flexibility that standard programs can’t accommodate. Co-occurring mental health disorders—present in over 60% of addiction cases—demand integrated psychiatric care, not sequential treatment that addresses one condition while ignoring the other.
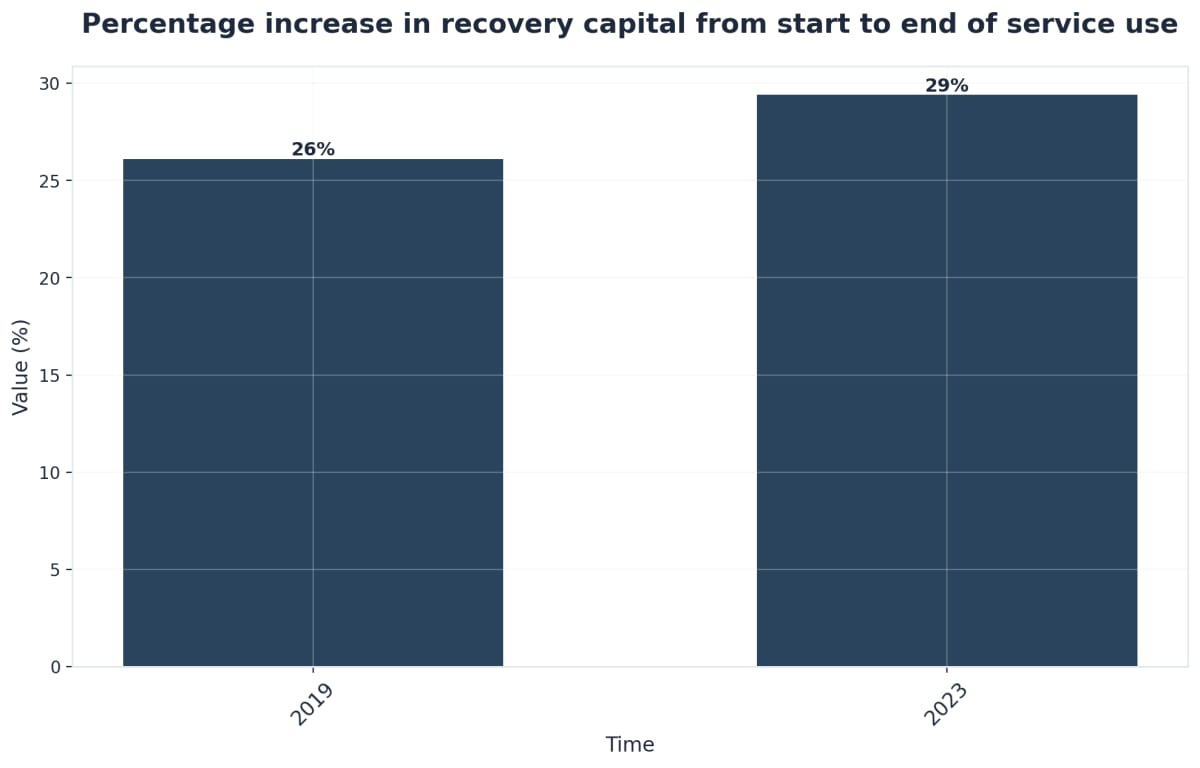
Measurable outcomes separate marketing claims from clinical reality. PCTD utilizes ERPHealth software to track statistically-significant treatment results across their continuum, providing transparency that vague success stories cannot. This data-driven approach extends through alumni services, where ongoing support and accountability transform initial sobriety into sustained recovery.
Data Point: Detox + Structured Aftercare = Up to 60% higher long-term success rate.The evidence remains clear: comprehensive aftercare produces dramatically different outcomes than detox alone. Your loved one’s recovery requires more than medical supervision during withdrawal—it demands a complete pathway from crisis stabilization through long-term community integration. That pathway should include evidence-based therapies, medication-assisted treatment when clinically indicated, and specialized support addressing their specific circumstances rather than one-size-fits-all programming.
References
- SAMHSA National Helpline and Treatment Locator. https://www.samhsa.gov/find-treatment
- NIDA: Principles of Drug Addiction Treatment – A Research-Based Guide. https://www.nida.nih.gov/publications/principles-drug-addiction-treatment-research-based-guide
- American Society of Addiction Medicine (ASAM) – Professional Standards. https://www.asamonline.org/
- SAMHSA: 2023 National Survey on Drug Use and Health (NSDUH) Data. https://www.samhsa.gov/sites/default/files/programs_campaigns/nsduh/2023-nsduh-detailed-tables.pdf
- CDC: Substance Use and Substance Use Disorders. https://www.cdc.gov/substance-use-disorders/index.html
- The Joint Commission – Behavioral Health Accreditation Standards. https://www.jointcommission.org/accreditation-and-certification/certification/certifications-by-setting/behavioral-health-certification/
- American Psychological Association – Evidence-Based Treatment for Substance Abuse. https://www.apa.org/science/about/psa/substance-abuse
- National Institute of Mental Health – Co-Occurring Disorders Resources. https://www.nimh.nih.gov/health/topics/substance-use-and-mental-illness
- NIH/PubMed Central – Aftercare Following Addiction Treatment: Outcomes and Predictors. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3487846/
- Healthcare.gov – Substance Abuse Services Coverage. https://www.healthcare.gov/coverage/substance-abuse-services/





