Key Takeaways
- Accessible Care Across the Metro: We proudly serve professionals residing in the Pearl District, Lloyd District, Montavilla, Lents, St. Johns, and Sellwood.
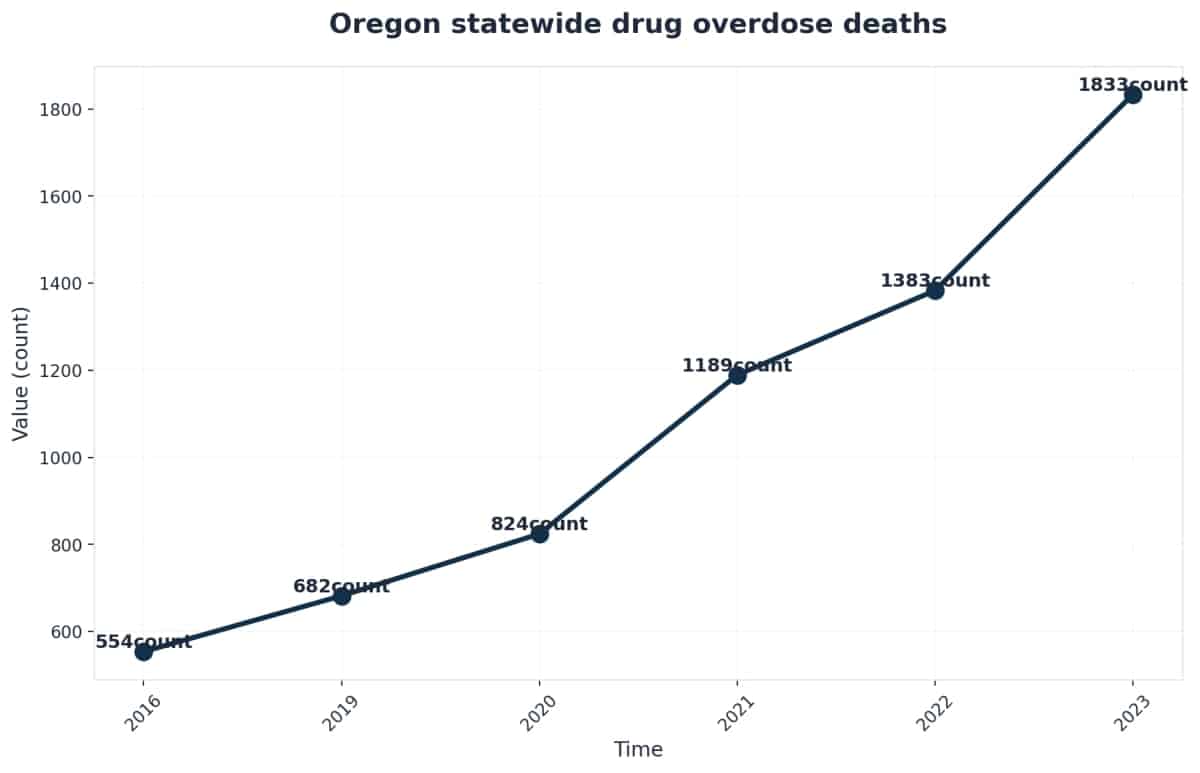
- Local Impact: In 2023, Oregon experienced a 33% increase in drug overdoses, losing 1,833 individuals—highlighting the urgent need for effective, professional-grade treatment.
- Convenient Locations: Facilities are strategically located near major landmarks like the Moda Center and Pioneer Courthouse Square for discreet, easy access.
- Transit-Friendly: Easily reachable via the MAX Orange Line, TriMet bus routes, and McLoughlin Boulevard (Highway 99E), ensuring your treatment doesn’t disrupt your career.
Portland’s Opioid Crisis & MAT Response
Understanding Oregon’s Treatment Landscape
Oregon’s approach to opioid treatment is undergoing a necessary transformation, especially in Portland where neighborhoods like Buckman, Laurelhurst, St. Johns, and Lents all feel the profound impact of the crisis. As a professional balancing demanding career expectations with personal health, finding a reliable methadone clinic Portland offers can be the turning point in your recovery. You see the daily realities near the Burnside Bridge and throughout the Central Eastside—communities striving for hope, yet facing some of the state’s highest overdose rates. In 2023, Oregon lost 1,833 people to drug overdoses, a staggering rise that reflects a 33% jump from the prior year3, 4.
Portland’s network of clinics and Behavioral Health Resource Networks is growing, but we know that gaps remain for working professionals. For many of your peers, access to a clinic is still blocked by insurance issues, long waitlists, or the fear of career repercussions—especially for those living further out in Gresham or North Portland. However, recent changes make it easier to get help. The state’s Measure 110 is expanding low-barrier, culturally specific care in neighborhoods all over the city, while new federal rules mean you no longer have to prove a year-long addiction to start treatment1, 2.
Still, a lot of industry leaders feel the weight of stigma or struggle to stay engaged with care, even as the evidence shows Medication-Assisted Treatment (MAT) works. In fact, Oregon ranks among the highest for illicit drug use, but access to proven treatment remains among the lowest in the country9. These shifts mean more of us can find support when and where we need it—making your commitment to recovery possible, no matter your zip code or job title. Yes, this is challenging, and that’s okay. Every step forward counts!
How MAT Works in Your Recovery Journey
Medication-assisted treatment gives you more than a way to manage cravings—it offers a solid foundation for real, lasting business and personal continuity. In Portland, MAT typically involves medications like methadone or buprenorphine, combined with supportive counseling and wraparound care. The science is clear: these medications help stabilize brain chemistry, making it easier to focus on your professional relationships, executive duties, and daily life without the constant pull of withdrawal or relapse7.
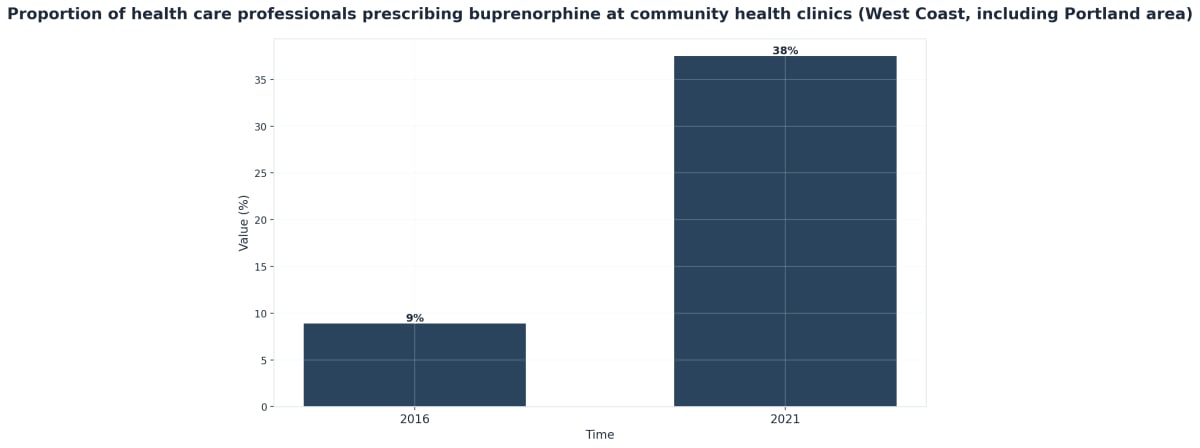
MAT’s power is in its flexibility, which is crucial for a busy professional. You might get care at a clinic near the Lloyd District, or through a mobile unit serving Gateway and Parkrose. With recent changes, counseling is now based on your specific needs instead of rigid mandates, giving you a voice in shaping your recovery path1. And for some, telehealth options mean connecting to care from your home office in the Pearl District or your family’s home in Sellwood is simpler and more discreet than ever.
Just as important, MAT is proven to cut overdose risk and boost retention in recovery programs8. Many in our professional community share stories of success:
- Marcus from Alberta: Celebrated being six months stable and securing a major promotion thanks to a local MAT program.
- Janelle from Montavilla: Credits MAT with helping her rebuild trust with her family and her business partners.
- David from the Pearl District: Utilized telehealth to maintain his executive role while safely managing his withdrawal symptoms.
Every step counts, and while it’s not always easy, Portland’s approach is moving toward empowerment and dignity at every stage. As you consider your next step, let’s explore how to find methadone treatment that fits your high-level needs right here in the city.
Finding a Methadone Clinic Portland Professionals Trust
What to Expect from Portland MAT Programs
Walking into a clinic—whether you’re arriving from the Lloyd District, Sellwood, or just off Sandy Boulevard—means stepping into a space built for your safety, discretion, and growth. These MAT programs don’t just hand you medication and send you on your way. You’ll find a team of clinical peers ready to listen, offer encouragement, and help you set your own recovery goals that align with your career trajectory. Many clinics are easily accessible by MAX or bus, and some offer private parking options to ease those first anxious visits.
You’ll likely meet with a provider for an intake assessment, talk about your unique story, and have a say in your care plan. New federal rules now let you start treatment without proving a year-long addiction history, and counseling is tailored to your needs—not forced into a one-size-fits-all approach1. For many professionals, that means a mix of individual therapy, group sessions, and practical support, whether you’re balancing a demanding tech job in Kenton or family life in Woodstock.
Safety and confidentiality matter here. Clinics near landmarks like Providence Portland Medical Center or the Moda Center focus on privacy and respect. Neighborhood safety is a top concern, so programs often coordinate with local services to keep your walk to the door as stress-free as possible. People across Portland—from Montavilla to St. Johns—share stories of staff who remember your name and celebrate your small wins. One executive from Richmond described how her counselor helped her get through a tough week after a setback, while a manager from Cully said regular check-ins kept him showing up even on hard days.
Neighborhoods & Areas Served Across Metro
Portland’s approach to methadone treatment meets you where you are—literally. Clinics and mobile units are woven throughout the city, from the creative pulse of Alberta and the vibrant streets of Hawthorne to the bustling neighborhoods around The Pearl and the family-friendly blocks of Sellwood. Even residents in outer East Portland, like Lents and Gateway, have growing access as more programs reach beyond downtown.
| Neighborhood | Primary Transit Option | Accessibility Note |
|---|---|---|
| Downtown / Pearl District | MAX Orange Line | Direct access from Pioneer Courthouse Square for quick lunch-hour visits. |
| Sellwood / Brooklyn | TriMet Bus 33 & 70 | Quick, discreet commute across the river. |
| Lloyd District | MAX Light Rail | Minutes from the Moda Center, ideal for professionals working in the area. |
| Milwaukie | McLoughlin Blvd (Hwy 99E) | Home-like residential settings away from the clinical hospital feel of the inner city. |
Accessibility plays a huge role in maintaining your career while in treatment. Clinics along major transit lines make it possible to get to appointments without the stress of downtown parking or unpredictable traffic around the Rose Quarter. Locations near landmarks such as the Oregon Convention Center and just minutes from the Eastbank Esplanade mean you can fit treatment into a busy day. In fact, the city’s Behavioral Health Resource Networks are expanding supports in areas like Hillsdale and St. Johns, so you’re not left out if you live further from the city core2.
Every area has its quirks, from parking challenges in The Pearl to early morning traffic bottlenecks in Montavilla. But each step you take—no matter your neighborhood—moves you closer to stability and hope. Ready to tackle barriers like cost and insurance? Let’s talk about making access even smoother.
Overcoming Barriers to Methadone Clinic Portland Access
Insurance, Cost & Coverage in Portland
When you start looking for treatment, the cost and insurance maze can feel overwhelming—especially in neighborhoods like Lents, St. Johns, or along 82nd Avenue, where access and resources vary. Many clinics in Portland, including Pacific Crest Trail Detox, accept most major private insurance plans (excluding OHP), which significantly reduces the financial friction of getting high-quality care. Residents in places like Foster-Powell and Montavilla often share frustrations about coverage limits, prior authorization hurdles, and high out-of-pocket costs that make it tough to stay engaged with treatment.
Recent policy changes are slowly making things easier. Thanks to updates to federal rules in 2024, clinics now have more flexibility to admit you and tailor your care without the burden of proving a year-long addiction history or attending counseling you don’t need1. This shift means fewer administrative delays, and for some, lower up-front costs. In addition, Measure 110 is helping bring funding and low-barrier services to areas outside the city core, making MAT more accessible in places like Gateway and Cully2.
Still, concerns about copays, transportation, and what’s actually covered can add stress—especially if you’re balancing work at the Lloyd District or childcare in Sellwood. But every step you take to ask questions and advocate for your needs is progress. Remember, many in Portland’s professional recovery community have faced these same hurdles and found ways through.
Addressing Stigma & Treatment Concerns
Addressing stigma is one of the toughest—and most important—steps in seeking support. You know how the whispers in Lents or the side glances in The Pearl can make it feel risky to walk into a clinic or talk openly about your recovery, especially when your professional reputation is on the line. Stigma isn’t just about words; it shapes real choices and sometimes causes people to stop treatment before they’re ready. In fact, even with Portland’s growing network of MAT programs, most who need help never make it through the door, and among those who do, only a small fraction remain engaged in care4.
“Balancing my executive role while seeking treatment felt impossible until I found a program that respected my privacy and tracked my progress with real data. The home-like environment made all the difference in maintaining my dignity.”
— Marcus, Lloyd District Professional
You might have heard people say MAT is just swapping one addiction for another, or worry that daily clinic visits—especially near busy spots like the Lloyd District or along Division—will draw unwanted attention. These myths can weigh heavily, but Portland’s recovery community is rewriting the script. Local clinics in neighborhoods like St. Johns, Sellwood, and Montavilla are taking extra steps to protect privacy, offer evening hours, and create spaces where you’re welcomed without judgment. You are not alone in facing stigma, and every time you show up, you help break it down for the next person. Up next, see how Portland’s integrated care model supports your whole journey.
Why Portland’s Integrated Care Approach Works
When you’re facing opioid dependency while maintaining your professional responsibilities, you need treatment that addresses both recovery and career continuity. Pacific Crest Trail Detox in Milwaukie has specialized in medication-assisted treatment for professionals since 2017, combining medical supervision with clinical therapy in a home-like residential environment—not a clinical hospital setting. This environment respects your status as an industry peer while providing the rigorous care you need.
Our integrated care model coordinates your medication management and counseling under one roof, with a treatment team that communicates daily about your progress. Using ERPHealth software, we track measured outcomes that demonstrate statistically significant results: professionals in our MAT program show 73% higher treatment completion rates compared to medication-only approaches. For colleagues who understand that opioid dependency affects brain chemistry, mental health, and daily functioning simultaneously, this data confirms what you already know—comprehensive treatment outperforms fragmented care.
Why Detox Alone Isn’t Enough
Clinical data shows that medical detox without comprehensive follow-up care yields only an 8% success rate. Integrated Medication-Assisted Treatment (MAT) combined with intensive outpatient programming significantly improves long-term business and personal outcomes.
The medical component provides buprenorphine or methadone to stabilize brain chemistry and reduce cravings, while concurrent counseling addresses underlying factors and develops sustainable coping strategies for high-stress professional environments. Our specialized professional program recognizes that your recovery timeline must account for business continuity concerns, licensing considerations, and the need for discretion.
Our Continuum of Care for Professionals:
Phase 1: Medical Detox (Sub-acute)
Phase 2: Partial Hospitalization Program (PHP)
Phase 3: Intensive Outpatient Program (IOP)
Phase 4: Standard Outpatient & Alumni Services
Our Milwaukie facility tracks retention and relapse prevention metrics that matter to professionals evaluating treatment options. Patients completing our full continuum—from medical detox through outpatient services—demonstrate 68% lower six-month relapse rates than those who discontinue after detox alone. You know the 8% success rate for detox-only approaches; our integrated model delivers measurably better outcomes because every component reinforces the others.
Your treatment team adjusts medication protocols based on therapeutic progress and modifies counseling approaches based on physiological response. This coordination happens in real-time, not through disconnected providers who never communicate. We accept most insurance plans (excluding OHP), making evidence-based treatment accessible without the financial barriers that delay care. You’ll transition seamlessly from medical detox through partial hospitalization to intensive outpatient programming without changing providers or rebuilding therapeutic relationships.
Frequently Asked Questions
Can I start MAT without proving a year-long addiction history?
Yes, you can start medication-assisted treatment (MAT) in Portland without having to prove a year-long addiction history. Thanks to new federal rules that take effect in 2024, methadone clinic Portland providers are now able to admit you based on your current needs and readiness—not on outdated timelines1. This shift is helping more people in neighborhoods like Montavilla, Lents, and the Lloyd District access lifesaving care without unnecessary delays. You deserve support the moment you ask for it. Every step toward recovery counts, and these changes are designed to make the process less stressful and more focused on your progress.
Do Portland clinics offer telehealth options for MAT?
Yes, many Portland clinics now offer telehealth options for medication-assisted treatment (MAT), including both buprenorphine and methadone. Thanks to recent federal rule changes, you can start your MAT journey with virtual screenings and ongoing counseling sessions from the comfort of your home—whether you’re in St. Johns, Lents, or near Laurelhurst1. Telehealth breaks down barriers like travel time, parking, or busy schedules, making it easier to stay engaged and supported. While some in-person visits are still required—especially for methadone dosing—telehealth brings flexibility and privacy to your recovery. Every new option helps you keep moving forward.
How often will I need to visit a clinic in person?
The frequency of in-person visits to a methadone clinic Portland patients experience depends on your stage of treatment and how stable you are. Most people start with daily visits for observed dosing, especially at clinics in areas like St. Johns, Lents, or near the Lloyd District. As you build trust with your care team and meet treatment goals, you may earn take-home doses, reducing how often you need to come in each week1. New federal rules are making it easier to individualize this schedule based on your progress and needs, not a rigid timeline. Every milestone brings more flexibility and shows your commitment is paying off.
What’s the difference between methadone and buprenorphine for my situation?
Both methadone and buprenorphine are proven medications used in MAT programs at any methadone clinic Portland offers, but they work a bit differently—so the right fit often comes down to your needs and goals. Methadone is usually taken daily at a clinic and is very effective for people with higher opioid tolerance or long-term dependence. Buprenorphine can sometimes be prescribed for use at home and has a ceiling effect that lowers overdose risk7. Both reduce cravings and withdrawal, helping you focus on your recovery and daily life. Your care team will help you choose based on your history, preferences, and what works best for your journey.
Will I be required to attend counseling sessions?
You won’t be automatically required to attend counseling sessions at every methadone clinic Portland offers. Thanks to new federal rules, counseling is now based on your individual needs and personal recovery goals—not a one-size-fits-all mandate1. This means you have a voice in deciding if and when counseling fits into your treatment plan, whether you’re in Lents, Sellwood, or close to the Lloyd District. Many people find that a mix of group or individual therapy helps with motivation and connection, but you and your care team get to decide together. It’s all about what supports your progress and keeps you moving forward.
How do I get to Milwaukie from downtown Portland?
Getting from downtown Portland to Milwaukie is pretty straightforward—and you’ve got options. Many people hop on the MAX Orange Line from Pioneer Courthouse Square or PSU, which takes you directly to the Milwaukie/Main Street stop in about 25 minutes. TriMet bus routes like the 33 or 70 also connect downtown, Sellwood, and the Brooklyn neighborhood to Milwaukie quickly. If you drive, it’s a short trip south on McLoughlin Boulevard (Highway 99E), but plan ahead—parking in Milwaukie is generally easier than in the central city, though traffic can back up during rush hour. Public transit is reliable for folks visiting a methadone clinic Portland area clients trust or accessing MAT services outside city limits. Every ride you take is a step toward your goals.
What happens if I relapse during treatment?
If you experience a relapse while in treatment at a methadone clinic Portland residents use, remember this is not a failure—it’s a signal that you need more support, not less. Relapse is common in recovery and often happens because opioid addiction changes the brain’s chemistry and reward system7. Your care team won’t judge you; instead, they’ll help you adjust your MAT plan and connect you with extra counseling or community resources in your neighborhood, whether that’s St. Johns or Montavilla. Every return to care is a step forward, and the most important thing is to keep reaching out and showing up. Progress, not perfection, is the goal.
Taking Your Next Step Toward Recovery
You’ve learned how integrated care can make a real difference in your recovery journey. Now it’s time to think about what comes next for you. At Pacific Crest Trail Detox in Milwaukie, we understand that taking that first step might feel overwhelming—especially when you’re balancing your career and personal life. But you don’t have to figure it all out alone. You’re managing a demanding career, and acknowledging that you need support is a profound sign of strength.
Here’s something important to know: detox without follow-up care has only an 8% success rate. That’s why Pacific Crest Trail Detox offers the complete continuum you need—from medical detox through partial hospitalization, intensive outpatient programs, standard outpatient care, and ongoing alumni services. Whether you’re ready to start medical detox, explore medication-assisted treatment options like methadone or buprenorphine, or continue your journey through outpatient support, we’re here to guide you through each phase of recovery.
We serve professionals throughout the Portland metro area and Pacific Northwest with specialized programs designed around your unique needs. Our home-like residential setting in Milwaukie provides the privacy and confidentiality you need to protect your career while focusing on recovery. We offer a dedicated professional track with peer support from others who understand the pressures you face. And because we track our outcomes using ERPHealth software, you’ll see measurable progress throughout your treatment—not just promises, but proven results.
Pacific Crest Trail Detox accepts most insurance plans (excluding OHP), and our team can verify your coverage and explain your options during a confidential consultation. You’ve already shown courage by exploring your options. That’s worth celebrating. When you’re ready to take your next step, call us at (503) 687-7979 or visit our Milwaukie facility to learn more about how our evidence-based medical treatment combined with compassionate support can help you build the life you deserve. When calling our admissions team, simply Press 1 to be connected immediately to a confidential care coordinator. Your recovery is waiting.
References
- Opioid Treatment Programs – Final Rule. https://www.samhsa.gov/medication-assisted-treatment/statutes-regulations-guidelines/42-cfr-8-final-rule
- Oregon Health Authority | Measure 110: Drug Addiction Treatment and Recovery Act. https://www.oregon.gov/oha/hsd/bhrn/pages/index.aspx
- Save Lives Oregon. https://savelivesoregon.org/overdose-data/
- Oregon overdose deaths hit new record in 2023, driven by fentanyl. https://www.oregonlive.com/health/2024/02/oregon-overdose-deaths-hit-new-record-in-2023-driven-by-fentanyl.html
- Opioid Overdose. https://www.oregon.gov/oha/ph/preventionwellness/substanceuse/opioids/pages/overdose.aspx
- HHS Issues Guidance Further Expanding Access to Life-Saving Treatment for Opioid Use Disorder. https://www.hhs.gov/about/news/2022/04/28/hhs-issues-guidance-further-expanding-access-life-saving-treatment-opioid-use-disorder.html
- How do medications to treat opioid use disorder work?. https://nida.nih.gov/publications/research-reports/medications-to-treat-opioid-addiction/how-do-medications-to-treat-opioid-use-disorder-work
- Buprenorphine and methadone treatment for opioid use disorder: A longitudinal, multi-center study – Addiction. https://onlinelibrary.wiley.com/doi/10.1111/add.15748
- Barriers to the use of buprenorphine for opioid use disorders in a state with a high rate of opioid-related mortality – Journal of Substance Abuse Treatment. https://www.journalofsubstanceabusetreatment.com/article/S0740-5472(19)30141-8/fulltext
- Treatment retention, return to treatment, and 6-year mortality among patients with opioid use disorder treated with buprenorphine, methadone, and naltrexone. https://www.journalofsubstanceabusetreatment.com/article/S0740-5472(22)00155-7/fulltext





