Key Takeaways
- The definition of recovery from addiction is an ongoing process of improving health, wellness, and quality of life for your loved one.
- Medical detox is just the first step; without follow-up care, the success rate is only 8%.
- Comprehensive care, like partial hospitalization programs (PHP) and intensive outpatient programs (IOP), builds a foundation for lasting change.
- Medication-assisted treatment (MAT) and tracking progress with tools like ERPHealth software provide measurable, evidence-based results.
- This guide is designed for parents seeking trusted, medically supervised care pathways for their adult children.
What the Definition of Recovery from Addiction Actually Means
The Medical and Clinical Definition
When you are looking for help for your adult child, understanding the definition of recovery from addiction is your first crucial step. It isn’t just about stopping substance use. Instead, recovery is seen as a gradual process where the brain and body heal, daily functioning improves, and a person is able to make healthy choices more often.

Imagine recovery as rebuilding a house after a storm: you don’t just sweep away the debris (stop using), you also repair the foundation, walls, and roof (heal physically, emotionally, and socially). At Pacific Crest Trail Detox (PCTD), we provide a home-like residential environment rather than a clinical hospital setting to make this rebuilding process as comfortable and dignified as possible.
Health organizations such as the American Society of Addiction Medicine describe recovery from addiction as establishing remission—a period when the symptoms of addiction are reduced or gone—and returning to productive daily life. This may include periods of complete abstinence or, for some, carefully managed use with medical support4. It’s not a one-size-fits-all journey.
The Diagnostic and Statistical Manual (DSM-5-TR) takes it further by defining stages like early remission (3-12 months without symptoms) and sustained remission (over 12 months)9. The Substance Abuse and Mental Health Services Administration (SAMHSA) highlights that this journey is about ongoing change—improving health, taking charge of your own life, and reaching your full potential1. Every step, whether big or small, gets your loved one closer to that goal.
Beyond Abstinence: A Holistic View
When you hear the phrase “recovery from addiction,” it might be tempting to picture someone who simply never uses drugs or alcohol again. But the journey goes much deeper than just stopping substance use. Think of recovery like growing a garden: pulling out the weeds (avoiding substances) is only part of the work.
“True growth also means nourishing the soil, planting new seeds, and making sure the environment is healthy for everything to flourish.”
A holistic view of recovery means looking at the whole person—not just their substance use, but their health, mental wellbeing, relationships, and sense of purpose. Research shows that people are more successful in recovery when they rebuild connections with family, friends, and community, and when they find new meaning in daily life1.
Recovery can include learning new coping skills, managing stress, and building self-confidence. For many, it also involves addressing other mental health needs or finding safe housing and stable employment. This broader picture matters because the journey out of addiction touches every part of someone’s life.
By embracing this all-around approach, you’re not just helping someone avoid old habits—you’re supporting them in building a new, healthier life. Next, we’ll break down the four core dimensions that shape recovery and how each one supports lasting change.
The Four Core Dimensions in the Definition of Recovery from Addiction
Health, Home, Purpose, and Community
The definition of recovery from addiction is often described using four major building blocks: health, home, purpose, and community. These aren’t just buzzwords—they’re the real-life supports that help your loved one maintain progress and heal in all areas of life. Think of them like the legs of a sturdy table: when one is missing, the whole thing can wobble.
| Dimension | What It Means in Practice | How PCTD Supports It |
|---|---|---|
| Health | Making choices that help the body and mind recover, like managing stress and overcoming withdrawal. | Providing non-hospital medical detox and medication-assisted treatment (MAT). |
| Home | Having a safe, stable, and supportive place to live during and after treatment. | Offering a home-like residential environment that feels safe and welcoming. |
| Purpose | Finding direction through goals, employment, or daily meaningful activities. | Integrating career counseling and intensive outpatient programs (IOP) for professionals. |
| Community | Building a positive support network of friends, family, and peers. | Fostering connection through group therapy and robust alumni services. |
By focusing on all four dimensions, the approach turns into a whole-life strategy that celebrates every win, big or small. Research shows that people with strong social support are more likely to stay in recovery and reach their goals1.
How Brain Changes Support Recovery
When people talk about the healing process, it’s important to remember that real change starts in the brain. Addiction isn’t just a problem of willpower. Substances can rewire the brain’s reward and decision-making systems, making it difficult for people to stop using even when they want to.

What is Neuroplasticity? (Click to expand)
Neuroplasticity is the brain’s incredible ability to heal and adapt. Think of the brain like a trail in the woods. If you walk the same path every day (using substances), it becomes well-worn. Recovery is about making new paths—choosing healthier routines and responses—until those become the new normal.
Research shows that, with time and support, the brain can rebuild connections and restore balance to areas affected by addiction. This process can improve self-control, memory, and emotional stability, supporting people as they make better choices and handle stress in healthier ways5.
True recovery means the brain isn’t just going back to how things were before addiction—it’s developing new strengths to help someone thrive. It reminds us that progress can be slow, and setbacks can happen. But every healthy choice helps reinforce these new pathways—celebrating even small wins along the way.
Different Pathways to Sustained Recovery
Medication-Assisted Treatment as Recovery
It’s easy to imagine that stopping all substance use is the only way forward. But science and medical practice now recognize that recovery can also include medication-assisted treatment (MAT). Think of MAT like using crutches after a leg injury—crutches don’t fix the bone, but they support you while you heal and relearn how to walk confidently.
In recovery, medications such as buprenorphine, methadone, or naltrexone can help balance brain chemistry, reduce cravings, and make it easier to focus on building a healthier life. Leading agencies have updated their guidance to include MAT as a valid and effective recovery pathway1.
This approach combines medication with counseling and support, helping individuals regain control and stability, especially when withdrawal symptoms or cravings might otherwise derail progress. Research shows that people who participate in MAT programs are more likely to stay in treatment and avoid relapse compared to those who rely on willpower alone3.
MAT isn’t about substituting one addiction for another; it’s a carefully monitored medical approach. Just as someone with diabetes might use insulin, people recovering from addiction sometimes need medication to support their health and independence. Every person’s journey is unique, and every step forward—no matter how it looks—deserves recognition.
The Role of Professional Support
Professional support is one of the strongest anchors a person can have. Imagine recovery as learning to navigate a river with unpredictable currents. While personal determination matters, having a skilled guide in the boat—like a medical provider, counselor, or addiction specialist—makes the journey safer and more likely to succeed.
Professional support teams bring medical knowledge, structure, and a sense of accountability that loved ones or peers may not be able to provide alone. This can include doctors who manage withdrawal symptoms, therapists who help unpack underlying struggles, and case managers who connect people with housing, job support, or mental health care.
At PCTD, we differentiate ourselves by measuring these outcomes. We use ERPHealth software to track statistically significant treatment results. For instance, clinicians might use a specific code snippet to log patient progress:
// Example of tracking patient stability
function checkProgress(patient_stability_index) {
if (patient_stability_index >= 8.5) {
return "Ready for Intensive Outpatient Program (IOP)";
}
}
As a parent, you might simply press Enter on a portal to see that your loved one is progressing safely. Research has found that people who engage in long-term professional treatment have recovery rates 50-70% higher than those who only complete detox without continued care2.
Guidance from professionals also means that setbacks or relapses don’t have to derail progress—instead, they become moments for learning and adjustment, not shame. By leaning on professional support, individuals and families create a stronger foundation for long-term wellness, resilience, and hope.
Why Long-Term Support Matters for Success
Recovery from addiction isn’t a sprint—it’s a journey that unfolds over time. And here’s something that might bring you both hope and clarity: the real work begins after detox ends. Medical detox addresses the physical dependence—helping your loved one safely withdraw from substances under medical supervision—but lasting recovery requires building new patterns, developing coping skills, and creating a life worth protecting.
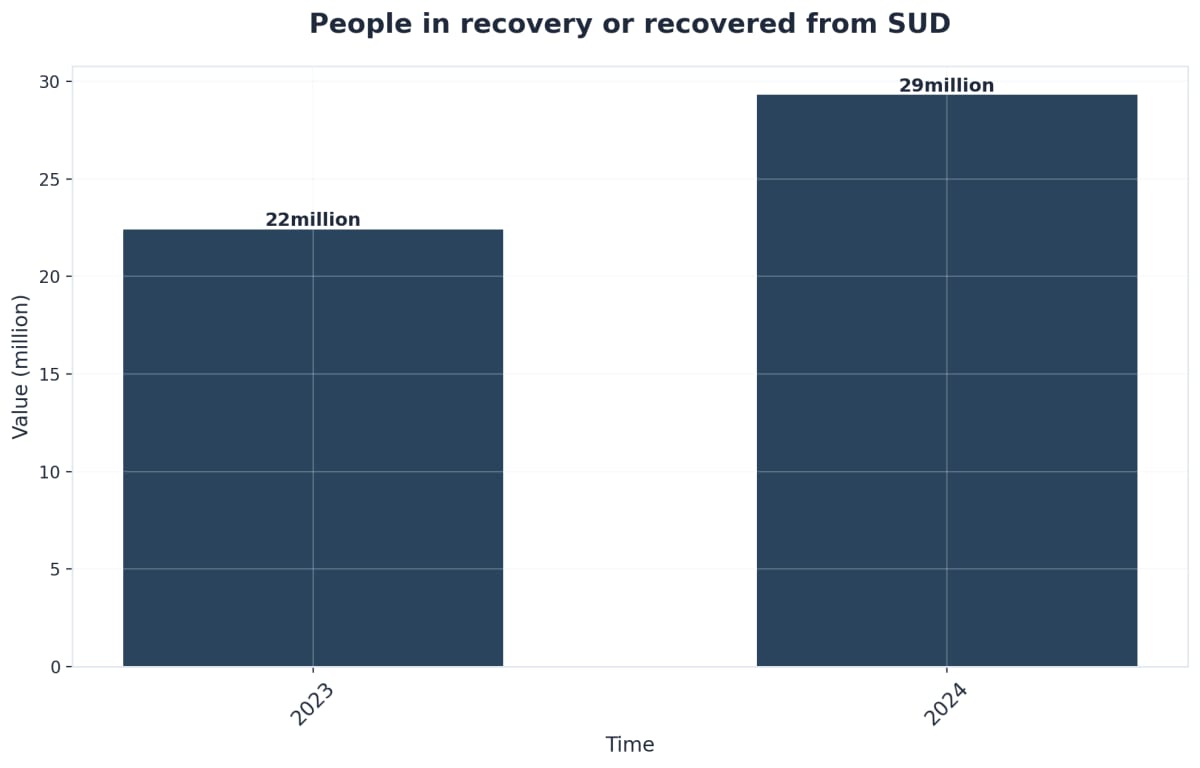
The statistics tell a sobering story, and you deserve to know the truth. When detox stands alone without follow-up care, the success rate hovers around just 8%. That means the vast majority of people who complete detox without ongoing support return to substance use. It’s not a failure of willpower or character—it’s simply that detox alone doesn’t provide the tools, community, and structure needed to navigate the challenges of early recovery.
This is exactly why Pacific Crest Trail Detox tracks outcomes using ERPHealth software—because measuring progress at each stage helps ensure your loved one is truly moving forward, not just completing programs. This is where a true continuum of care makes all the difference.
- Partial Hospitalization Programs (PHP): Attending therapy five days a week while living in a supportive environment.
- Intensive Outpatient Programs (IOP): Gradually stepping down clinical hours as they rebuild their life and career.
- Standard Outpatient & DUII Treatment: Ongoing maintenance and court-mandated support when necessary.
Long-term support also addresses something critical: co-occurring mental health conditions. Depression, anxiety, trauma, and other mental health challenges often fuel substance use. Without addressing these underlying issues through ongoing therapy and clinical support, your loved one faces an uphill battle.
There’s also tremendous value in community. Alumni services and aftercare programming connect people in recovery with others who understand their journey. This sense of belonging combats the isolation that often accompanies addiction. When you choose a treatment approach that emphasizes long-term care rather than quick fixes, you’re investing in real, measurable outcomes.
Frequently Asked Questions
Is recovery the same as being cured from addiction?
Recovery and being “cured” from addiction are not the same thing. The definition of recovery from addiction describes it as an ongoing process of change—improving health, making better choices, and building a fulfilling life, even if some symptoms or challenges remain. Unlike a cure, which means a problem is completely gone, recovery is more like learning to manage a long-term condition, such as diabetes. Most experts agree there is no permanent “cure” for addiction, but people can absolutely achieve strong, stable recovery with support and commitment 1. This journey is about progress, not perfection.
What’s the difference between early remission and sustained recovery?
Early remission and sustained recovery are two stages defined by how long someone has gone without symptoms of addiction. Early remission usually means a person has not shown any signs of addiction for at least three months but less than a year. Imagine it like finishing the first lap of a race—there’s momentum, but it’s still early in the journey. Sustained recovery (or sustained remission), on the other hand, means staying symptom-free for a year or more. This stage shows lasting stability and new healthy habits have taken root. These terms help professionals track progress and set realistic goals for the definition of recovery from addiction 9.
Can someone be in recovery while still taking medication for their addiction?
Yes, someone can absolutely be in recovery while still taking medication for their addiction. The definition of recovery from addiction now includes medication-assisted treatment (MAT) as a valid pathway, not just complete abstinence. Think of MAT like using glasses to help you see clearly—just as glasses support vision, medications like buprenorphine or methadone help stabilize brain chemistry and reduce cravings, allowing people to make healthier choices. Major health organizations recognize that recovery is about progress, stability, and improving quality of life—not how someone gets there 1. For many, these medications are a bridge to lasting change and independence.
How long does it typically take for the brain to heal during recovery?
Healing in the brain during recovery doesn’t happen overnight. Research shows that some brain changes begin to improve within weeks of stopping substance use, but full healing can take months or even years, depending on the person and the type of substance involved 5. Think of it like recovering from a sprained ankle: you might be able to walk after a few weeks, but reaching full strength and balance takes much longer. The definition of recovery from addiction includes this gradual process—small improvements in memory, mood, and decision-making add up over time. Staying patient and celebrating each sign of progress helps keep hope alive through the ups and downs.
Does a relapse mean recovery has failed?
No, a relapse does not mean recovery has failed. The definition of recovery from addiction is a process, not a single event, and setbacks are a normal part of learning new habits. Think of recovery like hiking a mountain trail—sometimes you might slip or lose your footing, but that doesn’t erase the progress you’ve made. Most experts agree that what matters is how someone responds to a relapse: reaching out for support, learning from what happened, and getting back on track. Studies show that people who remain engaged in support after a setback are far more likely to achieve lasting recovery 3.
What is recovery capital and why does it matter?
Recovery capital refers to all the resources—internal and external—that help a person succeed in recovery. It includes things like supportive relationships, a safe place to live, job skills, good health, and community connections. Picture recovery capital like a toolbox: the more tools someone has, the easier it is to fix problems and handle setbacks. Having strong recovery capital is linked to better outcomes and lower relapse rates, since people can draw on their strengths and supports when challenges arise. The definition of recovery from addiction now recognizes recovery capital as a key factor for long-term success 3.
Can recovery happen without formal treatment programs?
Yes, recovery can happen without formal treatment programs, though the journey may be harder and less predictable. The definition of recovery from addiction includes many paths—some people find success through self-help groups, faith communities, or by making personal changes with support from family and friends. Others may rely on online resources or peer-led meetings. Research shows that while these approaches work for some, people who engage in structured, professional support are more likely to achieve lasting recovery and avoid relapse 3. The key is that recovery is a personal process, and what works best depends on each individual’s strengths, needs, and available resources.
Conclusion
Your loved one’s recovery journey doesn’t end when detox does—it’s really just beginning. That’s why Pacific Crest Trail Detox offers something different: a complete pathway from medical detox through partial hospitalization, intensive outpatient care, and lifelong alumni services. Operating in Milwaukie, Oregon, and serving the broader Pacific Northwest region, PCTD provides a home-like residential environment where your family member can heal with dignity and comfort.
Remember, detox alone has only an 8% success rate. But when you combine medically supervised withdrawal management with evidence-based therapy, medication-assisted treatment, and continued support through PCTD’s full continuum of care, those odds improve dramatically. We accept most insurance (excluding OHP) to make this vital care accessible.
Whether they need specialized support as a veteran, LGBTQ+ individual, professional, or someone managing co-occurring mental health challenges, PCTD’s programs are designed to meet them exactly where they are. Recovery is challenging, and there will be ups and downs along the way. But here’s what matters: you’re taking action.
You’re researching options, asking the right questions, and refusing to give up on someone you love. That courage matters more than you know. With the right support system in place—one that combines medical expertise with genuine compassion, tracks progress with proven methods, and walks alongside your family for the long haul—real healing becomes possible. Every step forward counts, and you don’t have to navigate this alone.
References
- What is Recovery? | SAMHSA. https://www.samhsa.gov/find-help/recovery
- National Recovery Month | SAMHSA. https://www.samhsa.gov/recovery-month
- Treatment and Recovery | NIDA. https://www.nida.nih.gov/research-topics/treatment-recovery
- Definition of Addiction | American Society of Addiction Medicine. https://www.asam.org/quality-care/definition-of-addiction
- What Recovery From Addiction Really Means | NIH News. https://www.nih.gov/news-events/news-releases/what-recovery-addiction-really-means
- Alcohol Use and Your Health | CDC. https://www.cdc.gov/alcohol/fact-sheets/alcohol-use.htm
- Substance Use and Co-Occurring Mental Illness | NIMH. https://www.nimh.nih.gov/health/topics/substance-use-and-co-occurring-mental-illness
- A Definition and Framework for ‘Recovery’ From Substance Use Disorder | Substance Abuse and Rehabilitation. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3188625/
- Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR) | APA. https://www.psychiatry.org/psychiatrists/practice/dsm
- The Joint Commission – Accreditation Standards for Substance Use Programs. https://www.jcaho.org/





