Key Takeaways
- Assess Readiness: Use structured criteria to match clients with the right level of sober living programs to ensure long-term success.
- Bridge the Gap: Remember that detox without follow-up care has only an 8% success rate; structured aftercare is essential for lasting recovery.
- Track Outcomes: Utilize tools like ERPHealth software to monitor progress, adjust treatment plans, and celebrate every milestone.
Sober Living Programs as a Clinical Bridge
The Four Levels of Structured Support
When guiding clients through the recovery journey, finding the right environment is crucial. At Pacific Crest Trail Detox (PCTD), we know that completing a non-hospital medical detox in a home-like residential setting is just the first step. Because detox without follow-up care has only an 8% success rate, transitioning clients into structured sober living programs is a vital part of the continuum of care.
Checklist: Identifying the Right Level of Support in Recovery Housing
Recovery housing isn’t one-size-fits-all—it’s structured along four levels, each with its own intensity and resources. Here’s a quick tool to help you match client needs to the right level:
| Level | Description | Best Application |
|---|---|---|
| Peer-Run (Level I) | Managed entirely by residents without paid staff (e.g., Oxford House). Typical costs run $100–$125 per week.4 | Perfect for individuals seeking accountability and community, but who don’t require daily clinical oversight. |
| Monitored (Level II) | A live-in house manager provides structure and enforces rules, but clinical services are accessed off-site. | This approach works best when clients still need guidance but are building independence. |
| Supervised (Level III) | On-site staff coordinate with outpatient clinical teams. Group meetings and drug screening are standard. | This strategy suits organizations supporting clients with co-occurring disorders or higher relapse risk. |
| Integrated (Level IV) | Licensed clinical staff deliver therapy and case management in-house. | Opt for this framework when individuals need intensive support and a seamless bridge from treatment to community living.2 |
Matching the right level to each client’s stage of recovery can feel daunting, but every step forward counts! Your role in guiding this process sustains long-term stability and hope.
Next, we’ll explore how these structured supports impact outcomes for different populations.
Evidence-Based Outcomes Across Populations
When you’re guiding clients through recovery housing, it helps to know which outcomes to watch for. Utilizing tools like ERPHealth software allows professionals to track statistically-significant treatment results, ensuring that the care provided is truly effective.
- Sustained abstinence from substances
- Steady employment or school engagement
- Reduced legal or criminal justice involvement
- Improved mental health and stability
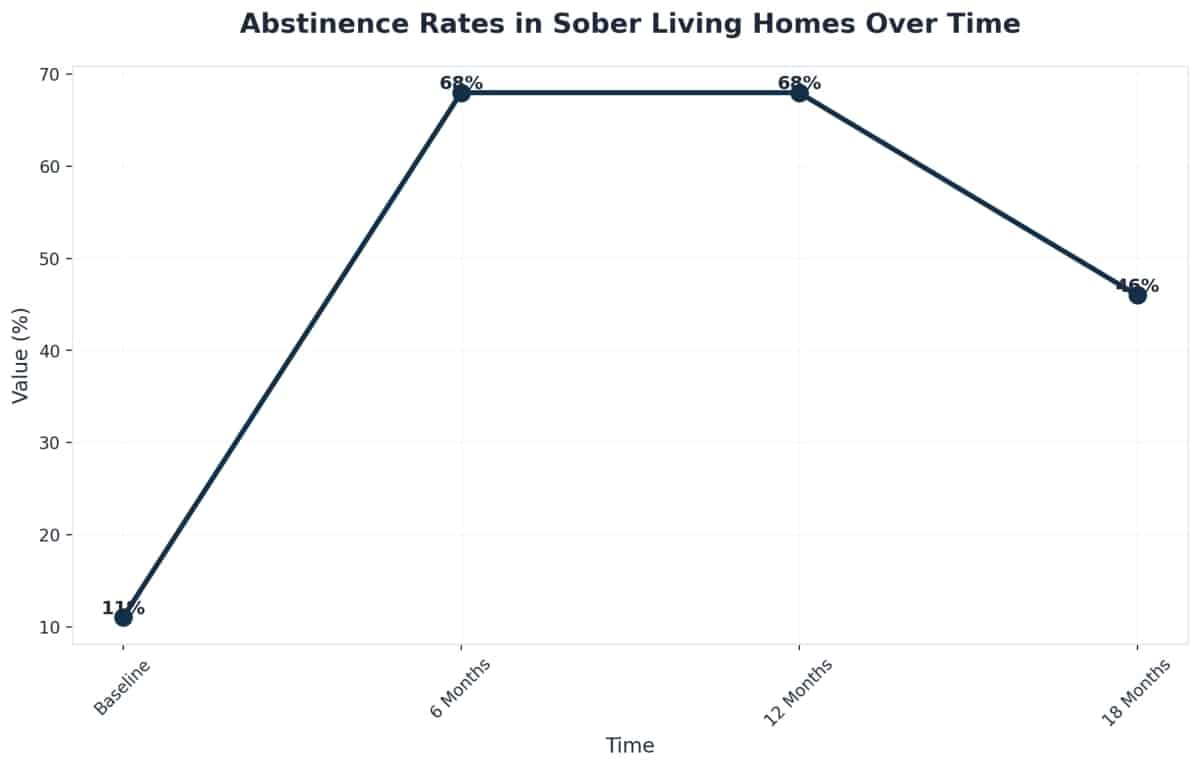
Sober living programs have shown remarkable impact on these outcomes. Research following residents for 18 months found abstinence rates jump from 11% at entry to 68% at both six and twelve months, holding strong at 46% at eighteen months.
“Arrest rates also dropped sharply from 42% before entry to 22% after one year of residence. Every population—from young adults to those with co-occurring disorders—benefits from this structured, supportive environment.”1
Specialized programs, like collegiate recovery housing, report recovery rates as high as 95% for students who participate.6
This approach is ideal for clients who need a bridge between intensive treatment—like a partial hospitalization program (PHP) or intensive outpatient program (IOP)—and total independence. Yes, it’s challenging to help someone stick with the process, but these results show that progress is possible in every stage of recovery. Celebrate those gains—every positive outcome matters, and your steady encouragement fuels their hope.
Next, we’ll look at how to determine when a client is clinically ready for recovery housing and how to time placement for the best results.
Determining Clinical Appropriateness for Sober Living Programs
Assessment Criteria for Placement Timing
Decision Tool: Clinical Readiness Checklist for Sober Living Placement
Determining the right timing for a client’s transition into sober living programs takes more than just checking boxes. Start by reviewing their stabilization in key domains:
- Substance Use: Has the client achieved a period of abstinence as verified by recent toxicology screens?
- Mental Health: Are symptoms of co-occurring disorders (like depression, anxiety, or PTSD) well managed with current supports?
- Medical Needs: Are any acute withdrawal symptoms resolved and chronic medical conditions stable?
- Motivation & Insight: Does the client express a willingness to participate in peer support, structure, and house rules?
- Social Support: Are there healthy connections outside of treatment, or is the client at risk for isolation or high-risk environments?
- Housing Urgency: Is alternative housing unsafe or unavailable?
Consider this method if the client has completed detox or residential care and needs accountability but isn’t ready for total independence. Research shows that residents who enter sober living programs after some stabilization—rather than directly from crisis—experience greater gains in abstinence and reduced legal involvement over time.1
This path makes sense for your client if they are motivated for change but lack a safe, recovery-focused environment. Celebrate the courage it takes to consider this transition: saying yes to structure is a win, not a setback. If you’re wrestling with placement timing, you’re not alone—balancing readiness and opportunity is part of the art of recovery care.
In the next section, we’ll discuss how length of stay and stabilization windows further influence recovery outcomes.
Length of Stay and Stabilization Windows
Supporting clients through sober living programs means helping them understand not just why, but how long, a structured environment can fuel recovery. The first six weeks are especially critical.
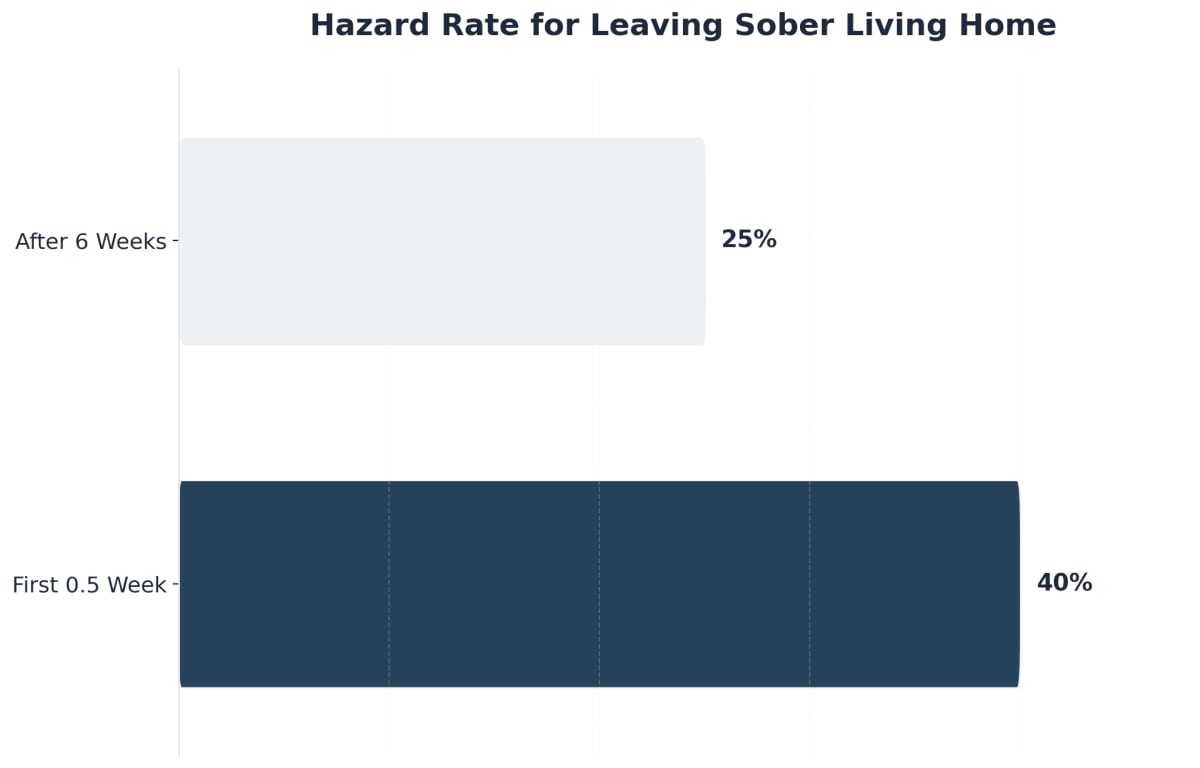
Research shows that nearly 40% of residents leave within the first half-week, but once a resident makes it past six weeks, the risk of early departure drops to just 25%.5 Framing this as a stabilization window can help clients (and teams) set achievable short-term goals and reduce the pressure of thinking about long-term commitments right away.
Stabilization Window & Length of Stay Tracker:
Phase 1 (Weeks 1-2): Acclimation & Routine Building
Phase 2 (Weeks 3-6): Core Stabilization & IOP Integration
Phase 3 (Weeks 7-12+): Independence & Alumni ServicesOpt for this framework when clients are still finding their footing post-detox or treatment. Committing to a stay of at least six weeks supports emotional and behavioral stabilization, giving residents time to adjust to routines, peer expectations, and the realities of daily sober life. Longer stays—typically three to six months—are associated with even stronger outcomes, including higher abstinence rates and decreased legal involvement.1
Yes, it’s challenging to encourage clients to stick it out when discomfort peaks in the early days. Remind them that every week they stay is a marker of progress, not perfection. Even small milestones—like attending house meetings or managing daily responsibilities—count. Your steady encouragement through this high-risk period can be the difference between a short stay and lasting recovery.
Up next, we’ll compare operational models to help you identify which type of sober living program best fits your population’s unique strengths and needs.
Operational Models and Program Selection
Peer-Run vs. Clinically Integrated Models
Decision Tree: Choosing the Best-Fit Operational Model for Your Population
- Does your population have a high degree of self-motivation and established community support? Peer-run models like Oxford House may fit, with resident governance, shared responsibilities, and weekly costs averaging $100–$125.4 These homes offer accountability and empowerment, but little direct clinical oversight, so they’re best for those further along in recovery or with stable mental health needs.
- Are your clients facing complex co-occurring disorders or higher relapse risks? Clinically integrated models, which include on-site licensed staff and in-house therapy, bring structure and access to clinical care. This solution fits organizations seeking close coordination with outpatient treatment, timely interventions, and ongoing case management.2
Residents benefit from a seamless bridge between treatment and independent living, but these models require more staff and regulatory resources. Each path has strengths: peer-run homes build autonomy and peer leadership, while clinically integrated residences deliver wraparound support and oversight.

This choice often comes down to the unique needs, readiness, and risk profiles of your clients. Yes, it’s a lot to weigh, but your thoughtful guidance here can be life-changing. Every client matched to the right model is a step toward lasting stability.
Next, we’ll explore how specialized housing options address the needs of specific populations within the sober living landscape.
Specialized Housing for Target Populations
Choosing the right sober living program often means finding a model tailored to your clients’ unique backgrounds and needs. Specialized recovery housing addresses gaps that traditional models might miss—giving people a sense of belonging and safety that directly fuels long-term outcomes.
Consider this route if your population faces distinct social or clinical challenges. For example, collegiate recovery housing—like the model at Rutgers University—pairs on-campus living with peer support and counseling, reporting recovery rates as high as 95% for participating students.6
At Pacific Crest Trail Detox, we recognize the importance of specialized programs for specific populations, including LGBTQ+ individuals, veterans, and professionals. LGBTQ-focused homes offer trauma-informed care and affirming environments, which can be vital for residents who have experienced discrimination or social isolation.11 Veterans’ programs blend substance use recovery with support for PTSD and service-related issues, while professional-focused residences address confidentiality and career re-entry.
Prioritize this when generic environments risk alienating or underserving clients. Community-specific housing typically requires additional training for staff, culturally informed programming, and often more rigorous safety protocols. Yes, it takes extra coordination and resources, but the payoff is clear: people thrive when they feel seen and supported. Celebrate each small victory—whether it’s a resident attending a support group for the first time or reconnecting with their identity in a safe space.
Up next, let’s walk through the financial realities and what it takes to help clients access these vital sober living opportunities.
Financial Planning and Access Barriers
Cost Structures and Funding Mechanisms
Helping clients access sober living programs often means navigating a patchwork of funding sources and cost structures. Most recovery residences operate on a fee-for-service model, with residents paying out-of-pocket for room, board, and basic supports.
| Setting Type | Estimated Cost | Funding Source |
|---|---|---|
| Peer-Run (e.g., Oxford House) | $100–$125 / week | Out-of-pocket, resident employment |
| Higher-Amenity / Urban | $1,000+ / month | Out-of-pocket, family support |
| Clinically Integrated | Varies (often highest) | Out-of-pocket, occasional grant subsidies |
Costs can vary dramatically—from as low as $100–$125 per week in peer-run settings to several thousand dollars per month in higher-amenity, urban, or clinically integrated homes.4, 11 Unfortunately, insurance rarely covers these housing expenses, since sober living is not classified as medical treatment. This reality creates a significant access barrier for many individuals, especially those transitioning directly from publicly funded care or with limited financial resources.11
Some states and localities are stepping up with public funding streams. Federal and state grants, such as those administered by SAMHSA’s State Opioid Response (SOR) program, may subsidize resident fees or support facility operations for eligible populations.3 A few state programs—like California’s CalWORKs Housing Support—also help with rent, deposits, or utilities for those facing homelessness, including people in recovery.10
Still, most clients and case managers must creatively braid together personal funds, temporary grants, or family support to bridge the gap. Every effort to expand public and private funding options brings us one step closer to equitable access.
Looking ahead, let’s examine the regulatory and zoning hurdles that can impact the availability of sober housing in your community.
Navigating Regulatory and Zoning Challenges
Before opening or expanding sober living programs, it pays to anticipate local regulatory and zoning challenges. You can use Ctrl + F on your local municipal code website to quickly scan for terms like “boarding house” or “group home” to understand your zoning landscape.
Many communities use zoning laws to limit where recovery residences can operate—sometimes grouping them with boarding houses or treatment centers, even though sober living homes are not medical facilities. This can lead to restrictions on occupancy, parking, or neighborhood density that push essential housing out of reach for those who need structured aftercare the most.11
Recent years have seen a trend toward stronger regulation and standardization. States like Texas (House Bill 299) and Pennsylvania now require accreditation or licensure for sober living homes to receive state funding or referrals.8, 9 These moves aim to boost quality and protect residents, but the patchwork nature of local laws still creates uncertainty for program operators and their clients.
This strategy suits organizations that are ready to invest in accreditation and community relations. Building neighborhood trust, embracing transparent practices, and seeking input from local stakeholders can help smooth the path. Yes, hurdles remain, but every step toward compliance and collaboration opens doors for long-term recovery housing.
Next, we’ll explore how to build sustainable infrastructure and partnerships that support the growth and stability of sober living resources.
Frequently Asked Questions
Can I use medication-assisted treatment while living in a recovery residence?
Yes, many recovery residences now welcome residents who use medication-assisted treatment (MAT), such as buprenorphine or methadone, as part of their recovery plan. But policies can vary—some sober living programs, especially those with a strict twelve-step focus, have historically discouraged or even prohibited MAT use. Thankfully, there’s been a positive shift as evidence grows that MAT improves outcomes for opioid and alcohol use disorders. If you or your client rely on MAT, it’s essential to check each home’s policy before placement. Advocating for evidence-based, inclusive support ensures everyone gets a fair shot at long-term recovery 11.
What happens if I relapse while living in a sober home?
If a relapse happens in a sober home, you’re not alone—this is a common experience, and support is built into the structure of most sober living programs. Typically, the house will have clear policies in place. Some may ask you to leave temporarily, while others will focus on adjusting your recovery plan or connecting you with extra support like counseling or outpatient treatment. The primary goal isn’t punishment, but helping you get back on track and minimizing risk for others in the house. Open communication and honesty are always encouraged, and relapses are treated as opportunities to learn and strengthen recovery skills 11.
How do I verify if a recovery home is accredited or licensed?
To verify if a recovery home is accredited or licensed, start by asking the home directly about its credentials and which agency provides oversight. Many states now require sober living programs to hold accreditation from organizations like the National Alliance for Recovery Residences (NARR) or obtain state licensure—Texas and Pennsylvania are two examples where these rules are enforced for homes that receive referrals or public funding 89. You can also check the NARR online directory or your state’s Department of Health or Drug and Alcohol Programs website for a list of approved residences. If you’re unsure, requesting written proof or searching public records can add peace of mind. Remember, choosing an accredited or licensed home helps ensure quality standards, resident safety, and reliable support throughout recovery 11.
Can family members visit me during my stay?
Yes, most sober living programs allow family visits, but the rules and schedules can vary by residence. Many homes encourage family involvement because positive connections can strengthen recovery, while some may limit visits during the initial adjustment period to help residents focus on building new routines. Always check the specific house guidelines—some may require advance notice, set specific visiting hours, or ask that family members participate in group activities or house meetings. If you’re unsure, ask staff or house managers for details. Remember, staying connected to loved ones is a source of hope and motivation for many residents 11.
What’s the difference between halfway houses and sober living homes?
Halfway houses and sober living homes both support people in early recovery, but they differ in structure and goals. Halfway houses are usually time-limited and may be connected to the criminal justice system, offering a set program length and more rules tied to probation or parole. Sober living programs, on the other hand, provide a less restrictive, peer-driven environment with flexible stays and a focus on building independence. Residents in sober living homes often choose their length of stay and participate in house governance. This model fits those seeking a supportive bridge between treatment and fully independent living 11.
Will living in a recovery residence affect my employment or education?
Living in a recovery residence is designed to support—not hinder—your employment or education goals. Many sober living programs require or encourage residents to work, attend school, or actively seek opportunities as part of building independence. Flexible schedules and community support make it possible to balance these responsibilities while focusing on recovery. Specialized models, such as collegiate recovery housing, show that students can achieve high academic success alongside their recovery—Rutgers University’s program, for example, reports a 95% recovery rate with strong GPA outcomes 6. If you’re worried about juggling both, remember that you’re not alone, and every small step counts toward your future.
How do I transition from a sober living home back to independent living?
Transitioning from a sober living home to independent living is a big step, and it’s normal to feel both excitement and anxiety about this change. Start by gradually increasing your responsibilities—like managing your budget, keeping a routine, and rebuilding healthy relationships. Many residents benefit from setting up aftercare plans (think: outpatient counseling, support groups, or alumni programs) before moving out. Celebrating each small milestone helps build confidence during this transition. Remember, you’re not expected to do it all at once—steady progress is what matters most. Sober living programs that encourage ongoing community support can make this transition smoother and reduce the risk of relapse 11.
Building Sustainable Recovery Infrastructure
Creating sustainable recovery infrastructure presents one of the field’s most persistent challenges: maintaining client engagement and support after the intensity of residential treatment ends. As relapse prevention professionals, we know that the transition from structured treatment to independent recovery is where most clients become vulnerable.
Building robust infrastructure means designing program elements that bridge this gap—creating systems that make sustained recovery more accessible than relapse for the clients we serve. Effective infrastructure begins with comprehensive programming that addresses varying client needs across the recovery continuum.
Evidence-based approaches like medication-assisted treatment (MAT) provide critical medical support during early recovery phases, while partial hospitalization programs (PHP) and intensive outpatient programs (IOP) offer flexible care levels as clients progress. The clinical challenge lies in ensuring seamless transitions between care levels—eliminating the gaps that compromise client retention and increase relapse risk.
What significantly impacts long-term outcomes is establishing ongoing engagement beyond formal treatment completion. Alumni services and recovery aftercare programming create sustained touchpoints that maintain therapeutic relationships and peer support networks. Regular group therapy sessions, individual counseling, and family therapy help clients navigate relationship repair and build healthy support systems.
These components aren’t supplementary—they’re essential infrastructure that directly correlates with retention rates and sustained recovery outcomes. Programs should also integrate practical supports like career counseling to address employment stability and co-occurring disorder treatment for clients presenting with mental health challenges.
“The data is clear: detox alone yields only an 8% success rate. Sustainable client outcomes require comprehensive programming that addresses medical, psychological, social, and practical recovery dimensions.”
Each component—from medication management to therapeutic interventions to community integration support—builds the infrastructure that determines whether our clients achieve lasting recovery or cycle back through treatment. By offering compassionate, personalized care with proven results, we can ensure that every individual has the foundation they need to thrive.
References
- Sober Living Houses for Alcohol and Drug Dependence: 18-Month Outcomes (Polcin et al.). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3057870/
- NARR Standards for Recovery Residences. https://narronline.org/resources/standards/
- SAMHSA State Opioid Response (SOR) Grants. https://www.samhsa.gov/state-opioid-response-grants
- Oxford House, Inc.. https://www.oxfordhouse.org/
- What Did We Learn from Our Study on Sober Living Houses and Where Do We Go from Here? (Polcin et al., Length of Stay research). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3989047/
- Rutgers University Recovery Housing. https://success.rutgers.edu/recovery-housing
- National Treatment Court Resource Center (NTCRC). https://ntcrc.org/
- Texas Legislature Online – HB 299. https://capitol.texas.gov/BillLookup/History.aspx?LegSess=88R&Bill=HB299
- Pennsylvania Department of Drug and Alcohol Programs – Recovery House Licensing. https://www.ddap.pa.gov/Pages/Recovery-House-Licensing.aspx
- California CalWORKs Housing Support Program. https://www.cdss.ca.gov/inforesources/cdss-programs/housing-and-homelessness/calworks-housing-support-program
- Sober Living Programs: What Are They & Do I Need One? – Perplexity Research. https://www.perplexity.ai/research/sober-living-programs





