Key Takeaways
- Editor’s Pick: Medical detox with medication support is the critical first step for safe withdrawal management, significantly reducing life-threatening risks.
- Integrated dual diagnosis care treats both addiction and mental health simultaneously, providing a unified approach for better long-term outcomes.
- Family-centered programs keep loved ones connected, which has been shown to nearly double treatment completion rates.
- Trauma-informed approaches ensure emotional safety while addressing the underlying wounds that often fuel substance use.
- Comprehensive aftercare and alumni services build a necessary safety net to prevent relapse and sustain recovery.
Understanding Personalized Treatment Planning Examples
When you are helping a loved one navigate the challenging journey of recovery, exploring effective treatment planning examples is a crucial first step. Effective personalized treatment planning goes beyond standard protocols—it requires integrating clinical assessment with real-world factors that influence recovery outcomes.
At Pacific Crest Trail Detox (PCTD), this means combining thorough medical evaluation with an understanding of each person’s substance use patterns, co-occurring mental health conditions, and the life circumstances that will either support or challenge their recovery journey. You are not just looking for a facility; you are looking for a partner in your loved one’s long-term wellness.
The assessment process identifies withdrawal risks, medication needs, and underlying conditions like depression, anxiety, or PTSD that require simultaneous treatment. Rather than a clinical hospital setting, PCTD’s home-like residential environment allows for more nuanced observation of how individuals respond to treatment in a less institutional context—insights that inform ongoing care adjustments throughout the continuum.
“Recovery is not a one-size-fits-all process. It requires a compassionate, adaptable approach that treats the whole person, not just the addiction, ensuring every step forward is built on a foundation of safety and trust.”
Treatment planning effectiveness depends on built-in flexibility. Medical detox protocols differ significantly from what’s needed during partial hospitalization or intensive outpatient phases. Evidence-based approaches combine medical supervision with clinical therapy calibrated to each recovery stage.
Some cases benefit from medication-assisted treatment, while others require intensive focus on trauma or co-occurring disorders. PCTD tracks these outcomes using ERPHealth software to measure statistically-significant results and refine treatment approaches, ensuring your loved one receives the most effective care possible.
Comprehensive plans address multiple recovery dimensions simultaneously: individual therapy for personal processing, group sessions for peer support, family therapy to address relationship dynamics, and structured aftercare planning. The research is clear—detox alone yields only an 8% success rate. Sustained recovery requires integrated care that extends well beyond withdrawal management.
Effective personalized planning establishes clear clinical goals, realistic timelines, and measurable outcomes. Whether working with LGBTQ+ individuals, veterans, professionals, or those with complex co-occurring conditions, individualized treatment provides the specific interventions needed to build lasting recovery—not just manage acute withdrawal, but develop sustainable skills and support systems for long-term wellness.
1. Medical Detox with Medication Support
When Medical Supervision Becomes Essential
Medical supervision is vital when withdrawal symptoms pose serious health risks, especially with substances like alcohol, benzodiazepines, or opioids. Supervised detox keeps your loved one safe, reducing risks such as seizures, dehydration, or heart complications that can happen when the body is clearing these substances.
Clinical guidelines highlight that unsupervised withdrawal from certain drugs can be life-threatening, making medical oversight non-negotiable in these cases3. At PCTD, our medical detox programs provide 24/7 monitoring in a comfortable, home-like setting, ensuring your loved one is never alone during this vulnerable time.
| Detox Approach | Safety Level | Medical Support Provided |
|---|---|---|
| Unsupervised (“Cold Turkey”) | High Risk | None |
| Medically Supervised (PCTD) | High Safety | 24/7 Monitoring & MAT |
Recognizing when to step up care is part of effective treatment planning. If your loved one has a history of severe withdrawal, co-occurring medical or psychiatric conditions, or has previously relapsed during detox, a medically supervised environment gives them the best chance to stabilize and move forward safely.
Compassion and safety go hand-in-hand with medical detox. When care teams monitor vital signs, manage discomfort, and adjust plans as needed, it’s possible to turn a frightening process into a hopeful first step. Every moment spent in a safe, supportive setting is a win that builds momentum for long-term recovery.
Medication-Assisted Treatment in Action
Medication-assisted treatment (MAT) is a key part of many treatment plans, especially when opioid or alcohol withdrawal is involved. MAT uses medications like buprenorphine, methadone, or naltrexone to ease withdrawal symptoms and lower cravings, while also supporting brain and body healing.

This approach is not about swapping one drug for another; it’s about stabilizing your loved one so they can focus on therapy, relationships, and rebuilding their life with dignity. Research shows that MAT improves retention in treatment and reduces the risk of relapse, especially during the vulnerable period after detox when cravings are strongest1.
People who receive MAT are more likely to stay engaged in care and achieve lasting recovery. Combining medication with counseling and peer support creates a powerful foundation for success. Treatment plans that include MAT reflect a commitment to safety, evidence, and real-world results. As you support your loved one, remember that every step toward stabilization is a step toward hope.
2. Integrated Dual Diagnosis Treatment Plans
Addressing Co-Occurring Mental Health Disorders
Navigating both substance use and mental health challenges together can feel daunting, but addressing co-occurring disorders at the same time is a proven pathway toward real progress. Integrated dual diagnosis treatment ensures your loved one isn’t forced to choose between mental health and addiction care—both are treated together, recognizing how deeply they influence each other.
This kind of treatment includes coordinated therapy, medication management, and support groups—all delivered by a unified team. Research shows that people with dual diagnoses are more likely to achieve stability and avoid relapse when both conditions are treated in the same setting6.
- Comprehensive Assessment: Identifying underlying conditions like anxiety, depression, or PTSD.
- Simultaneous Treatment: Addressing both addiction and mental health concurrently rather than sequentially.
- Unified Care Team: Ensuring all medical and clinical providers are on the same page.
Ignoring one side of the equation increases the risk of setbacks and hospitalizations, while integrated care leads to better engagement and long-term outcomes4. When you advocate for a plan that addresses every aspect of your loved one’s health, you’re creating a supportive environment where small victories build up over time. Every positive step, no matter how small, deserves to be celebrated!
Same Team, Same Setting Approach
Sticking with the same care team, in the same setting, gives your loved one a sense of stability and trust that’s hard to match. When professionals handle both mental health and substance use needs together, communication is clearer and care feels less fragmented.

This approach reduces the chance of mixed messages or overlooked symptoms, which are common when teams work in isolation. Research backs up what many families already know: coordinated care from a single, unified team leads to better engagement and fewer relapses4.
When your loved one doesn’t have to retell their story or bounce between providers, they’re more likely to open up, stick with treatment, and experience real progress. It’s a win for everyone—you, your loved one, and the care team working by your side. Treatment plans that prioritize this model show measurable improvements in outcomes for those with dual diagnoses. Yes, this journey is challenging, but every bit of consistency and teamwork helps build a stronger foundation for recovery.
3. Family-Centered Residential Programs
Keeping Families Together During Recovery
Staying connected as a family during recovery isn’t just comforting—it’s a game-changer for lasting progress. Family-centered residential programs are designed to keep loved ones together under one roof while a parent receives treatment, so bonds aren’t broken by separation.
This approach helps reduce anxiety for both the adult in care and their children, making it easier for everyone to heal and grow together. These programs offer daily routines, parenting support, and family therapy—all in a setting where family members can support and motivate each other.
Tips for Family Involvement
Participate in family therapy sessions, maintain open and honest communication, and educate yourself about the addiction recovery process to provide the best support possible without enabling destructive behaviors.
Research highlights that children living with a parent in residential treatment experience greater stability and safety, with 94% remaining free from abuse or neglect throughout the program5. Keeping families united during care helps break cycles of trauma and sets a foundation for healthy relationships after treatment.
Treatment plans that prioritize family unity reflect compassion, real-world needs, and measurable results. Every day spent together in a supportive environment is a step forward—progress you can be proud of!
Evidence of Family Support Impact
Family involvement isn’t just a nice-to-have—it’s a powerful driver for better outcomes in substance use recovery. Studies show that treatment plans with strong family support lead to higher completion rates and greater stability for everyone involved.
For instance, one residential program found that 94% of children living with a parent in treatment stayed safe from abuse or neglect, underscoring how a supportive environment protects the most vulnerable5. But it’s about more than safety. When families are engaged, adults in care are more likely to stay the course.
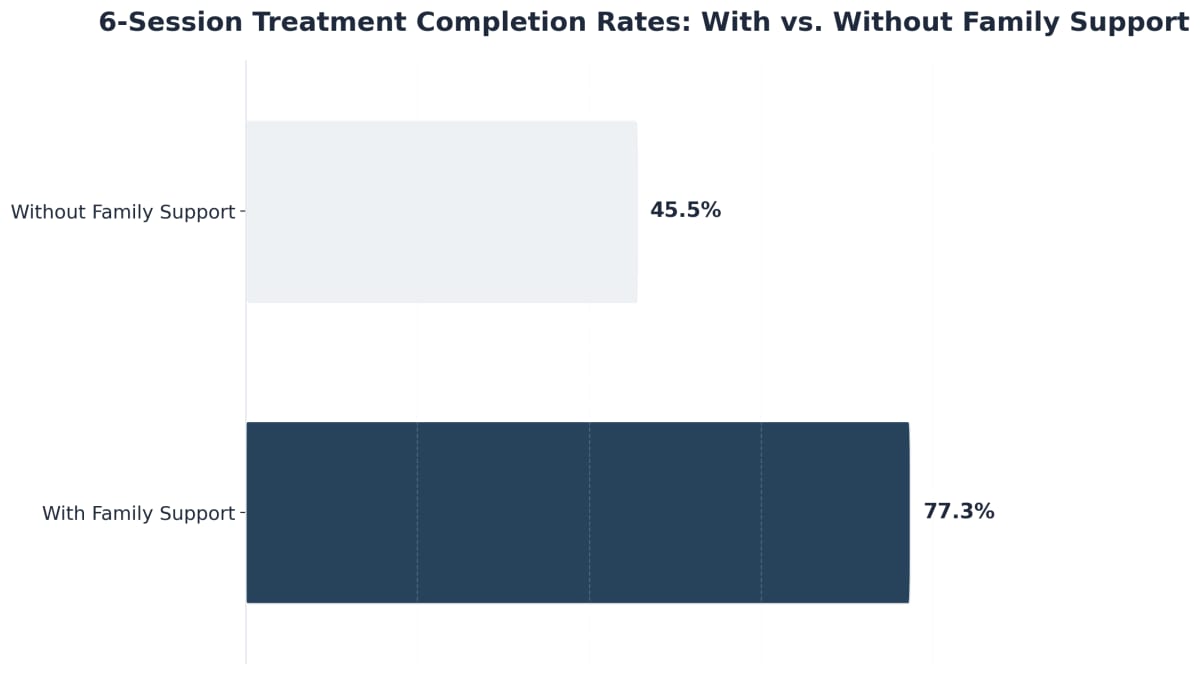
Research from community programs reveals that completion rates jump from 45.5% to 77.3% when family support is present, nearly doubling the odds of lasting change8. That’s a win you can celebrate—every extra day in treatment brings your loved one closer to long-term recovery.
4. Trauma-Informed Care Planning
Building on the foundation of personalized treatment planning, one specialized component deserves particular attention: trauma-informed care. When someone in your family has experienced trauma, traditional treatment approaches might not be enough.
Trauma-informed care planning recognizes that past experiences—whether childhood adversity, abuse, or other painful events—can deeply influence addiction patterns and recovery needs. This specialized approach creates a safer, more effective path forward. You deserve to know that the treatment team understands how trauma affects the brain and behavior.
Trauma-informed planning means clinicians screen for past experiences without forcing disclosure, create environments that feel emotionally safe, and avoid practices that might trigger painful memories. At PCTD’s home-like residential setting, this approach is woven into every aspect of care—from the comfortable, non-clinical environment to specialized programs for veterans who may carry combat-related trauma or LGBTQ+ individuals who’ve experienced discrimination or rejection.
Sample Trauma-Informed Daily Schedule: 08:00 AM - Mindful Morning Meditation 09:30 AM - Group Therapy (Safe Space Protocol) 11:00 AM - 1-on-1 EMDR Session 01:00 PM - Somatic Experiencing Workshop
It’s about building trust first, then addressing both addiction and underlying wounds together. This matters because research shows that up to 75% of people seeking addiction treatment have experienced significant trauma. When treatment ignores this connection, it misses critical pieces of the recovery puzzle.
The person you care about might struggle with trust, have difficulty regulating emotions, or use substances to cope with intrusive memories—all responses that need compassionate, informed care. This is especially true for those with co-occurring mental health disorders, where trauma often intersects with conditions like PTSD, anxiety, or depression.
Effective trauma-informed planning includes specialized therapies like EMDR (Eye Movement Desensitization and Reprocessing) or trauma-focused cognitive behavioral therapy, integrated with addiction treatment. At PCTD, clinicians assess how trauma symptoms interact with substance use patterns and co-occurring mental health conditions, then design interventions that address all three simultaneously.
If your loved one is in crisis, remind them they can always press 1 on the SAMHSA National Helpline for immediate, confidential support10. The goal isn’t just sobriety—it’s healing the whole person. When treatment teams understand trauma’s role in both addiction and co-occurring disorders, they can help your family member develop healthier coping strategies, rebuild their sense of safety, and create lasting change.
5. Comprehensive Aftercare & Relapse Prevention
Recovery doesn’t end when treatment is complete—in many ways, that’s when the real work begins. Just as trauma-informed care addresses the underlying wounds that fuel addiction, comprehensive aftercare supports both the healing process and long-term sobriety.
You know this journey requires ongoing support, which is why Pacific Crest Trail Detox’s continuum of care extends well beyond initial treatment. Think of aftercare as building a safety net that catches someone before a slip becomes a fall. PCTD’s structured approach moves individuals through levels of care based on their progress and needs.
This might mean transitioning from detox to a partial hospitalization program (PHP) for intensive daily support, then stepping down to an intensive outpatient program (IOP) that allows for work or family responsibilities, and eventually to standard outpatient services that provide ongoing therapy and accountability. What makes this continuum powerful is how it adapts to individual circumstances while maintaining structure.
Someone with demanding career obligations might benefit from IOP scheduling that works around professional commitments, while another person might need the daily structure of PHP to establish new routines. For those on medication-assisted treatment, ongoing MAT management ensures consistent support as they navigate recovery milestones.
PCTD’s alumni services create something equally valuable—connection with others who truly understand the journey. These aren’t just occasional check-ins; they’re an active community that celebrates progress, offers peer support during challenging moments, and reinforces the skills learned during treatment. You’ve probably noticed how powerful it is when someone connects with others who’ve walked the same path.
Relapse prevention planning weaves through every level of this continuum, helping identify unique triggers and develop specific coping strategies7. The recovery plan reflects real life—work schedules, family dynamics, mental health needs, and personal goals. This personalized approach, combined with ongoing therapy options and community support, builds the foundation for lasting change. Every therapy session attended, every support group meeting, every alumni gathering is another brick in that foundation.
Frequently Asked Questions
How were these five treatment planning examples selected?
These five treatment planning examples were chosen based on the latest research and clinical standards for supporting adults with substance use disorders. Each example reflects approaches proven to improve outcomes: medical detox with medication support, integrated dual diagnosis care, family-centered residential programs, trauma-informed planning, and comprehensive aftercare. They were selected because they address the most common medical, emotional, and social needs families encounter, and all are backed by evidence and professional guidelines1. By focusing on what actually works, this list helps you create a safer, more hopeful path forward for your loved one.
What makes medical detox with medication support the most critical starting point?
Medical detox with medication support is often the most critical starting point because it addresses immediate safety risks from withdrawal and creates a stable foundation for long-term recovery. For substances like alcohol, opioids, or benzodiazepines, unsupervised withdrawal can cause seizures, heart complications, or even death—so having medical supervision is non-negotiable3. Medication-assisted treatment (MAT) uses evidence-based medications to manage symptoms, reduce cravings, and help your loved one stay engaged in care1. This combination not only lowers the risk of relapse but also supports whole-person healing from the very beginning. Effective treatment planning examples always put safety and stabilization first, giving your loved one their best chance at lasting progress.
How long does the protracted withdrawal phase typically last after detox?
The protracted withdrawal phase—sometimes called post-acute withdrawal—can last anywhere from a few weeks up to six months after detox, depending on the substance and individual factors. During this time, your loved one might experience mood swings, sleep problems, anxiety, or strong cravings. Opioid withdrawal in particular is known for a longer protracted phase, with lingering symptoms and a general feeling of reduced well-being that can persist for months1.
Recognizing that these challenges are part of the healing process helps you offer patient, compassionate support. In treatment planning examples, ongoing therapy, peer support, and medication can make this phase more manageable and reduce the risk of relapse.
Why didn’t outpatient-only treatment make this list of examples?
Outpatient-only care can be a helpful step, but it wasn’t featured in these treatment planning examples because many adults with complex substance use needs require more than what outpatient programs alone provide. Higher-risk cases—like those involving withdrawal risks, co-occurring mental health disorders, or unstable living situations—often need medical supervision, integrated support, or family involvement that outpatient-only models can’t always deliver1. Research shows that matching the level of care to the individual’s needs—using tools like the ASAM Criteria—improves safety and long-term outcomes2.
If your loved one needs extra stability or support, consider programs that offer a continuum of care and adapt as their needs change.
What role does the ASAM Criteria play in determining the right treatment level?
The ASAM Criteria plays a central role in determining the right treatment level for your loved one. It offers a structured, evidence-based framework that guides professionals to match each person with services tailored to their medical, emotional, and social needs. This means your loved one isn’t automatically placed in the most intensive—or the least supportive—setting. Instead, care teams use the ASAM Criteria’s multi-dimensional assessment to evaluate withdrawal risks, mental health, living situation, and motivation, ensuring treatment planning examples are genuinely individualized2. By using this tool, you help set your loved one up for success with a plan that adapts as their needs change.
How does family involvement actually improve treatment completion rates?
Family involvement is a true game-changer for treatment completion. When families are actively engaged—by joining therapy sessions, supporting daily routines, or simply checking in—adults in treatment are much more likely to stick with their plan. Research from community programs shows that completion rates soar from 45.5% to 77.3% when family support is present, nearly doubling the odds of lasting recovery8.
Families provide encouragement, accountability, and a sense of belonging that helps your loved one push through tough moments. In the most effective treatment planning examples, every effort to include family is a step toward greater hope and stability.
Building Your Loved One’s Recovery Path With Treatment Planning Examples
Throughout this article, we’ve explored three pillars that define effective addiction treatment: personalized planning that addresses individual circumstances, trauma-informed care that recognizes underlying factors, and comprehensive aftercare that extends support beyond initial stabilization. These aren’t just theoretical concepts—they’re the framework that separates short-term intervention from sustainable recovery.
At Pacific Crest Trail Detox, these principles translate into measurable outcomes. Through ERPHealth software, we track treatment effectiveness with statistical rigor, providing transparency that respects your professional understanding of what works. Our continuum spans medical detox through alumni services, all within a home-like environment that reduces the clinical barriers many clients face during vulnerable moments.
You understand that detox alone yields only an 8% long-term success rate—that’s why our approach integrates medical supervision with ongoing clinical therapy, medication-assisted treatment when appropriate, and structured aftercare programming. Whether your loved one needs high-risk benzodiazepine detox, opioid withdrawal management, or treatment for co-occurring disorders, we provide specialized care backed by evidence-based protocols.
If you’d like to discuss how PCTD’s services might align with your loved one’s needs, we welcome a consultation. Our clinical team can conduct a comprehensive assessment and outline a potential treatment pathway. You can reach us at (503) 570-9478 or visit our Milwaukie facility to explore whether our approach represents the right partnership for your family’s situation. We accept most insurance and serve the broader Portland metro area.
References
- PMC NCBI – Evidence-Based Practices for Substance Use Disorders. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3678283/
- ASAM – The ASAM Criteria. https://www.asam.org/asam-criteria
- NCBI Books – Clinical Guidelines for Withdrawal Management. https://www.ncbi.nlm.nih.gov/books/NBK310652/
- PMC NCBI – Interventions for Co-occurring Disorders. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8479539/
- Casey Family Programs – Family-Based Residential Treatment. https://www.casey.org/family-based-residential-treatment/
- NIMH – Co-Occurring Substance Use and Mental Disorders. https://www.nimh.nih.gov/health/topics/substance-use-and-mental-health
- Recovery Research Institute – Relapse Prevention. https://www.recoveryanswers.org/resource/relapse-prevention/
- UW ADAI – Retention Toolkit: Family Involvement. https://adai.uw.edu/wordpress/wp-content/uploads/2019/03/RetentionToolkit_FamilyInvolvement.pdf
- PMC NCBI – Ensuring Continuity of Care Post-Hospitalization. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10360814/
- SAMHSA National Helpline. https://www.samhsa.gov/find-help/national-helpline





