Key Takeaways
- Drug detox symptoms are the physical and psychological reactions that occur when a dependent individual stops using substances.
- Medical supervision is critical, as withdrawal from alcohol and benzodiazepines can be life-threatening without proper care.
- Medication-assisted treatment (MAT) and structured aftercare significantly improve long-term recovery outcomes.
- This guide empowers professionals to better understand withdrawal physiology and optimize patient safety during crisis stabilization.
Understanding Drug Detox Symptoms and Physiology
How Your Brain Adapts to Substances
As a professional guiding individuals through crisis, you know firsthand how challenging drug detox symptoms can be. But how exactly does the brain change when someone uses drugs regularly? Think of the human brain like a highly sensitive control center, always working to keep things balanced. When substances like alcohol, opioids, or stimulants are introduced repeatedly, the brain starts to adjust. It gets used to having these chemicals around, almost like adjusting a thermostat when the weather changes outside.
Certain areas in the brain, particularly the reward circuit, start to rely heavily on the drug just to feel normal. Over time, natural ways of feeling pleasure—such as eating favorite foods or spending time with loved ones—simply don’t work as well. This happens because the brain’s natural “feel-good” signals become weaker, requiring more of the substance to achieve the same effect.
“Every step forward counts when you are guiding someone through the complexities of brain chemistry recovery. Your empathy and clinical understanding are their anchor.”
When the drug suddenly disappears, the brain isn’t ready. It reacts by swinging wildly in the opposite direction, leading to severe drug detox symptoms such as anxiety, tremors, sweating, and intense cravings. Imagine riding a bicycle and suddenly slamming on the brakes—the body wants to keep moving forward, but the environment has abruptly changed. That’s why withdrawal feels so harsh and unpredictable. Research shows these changes in brain chemistry can last for weeks or even months after stopping drug use, explaining why cravings and mood swings often linger3.
Why Withdrawal Symptoms Vary by Drug
Why do your patients experience such vastly different drug detox symptoms depending on the substance involved? It helps to think of each drug as having its own unique “lock and key” mechanism in the body. Alcohol, opioids, benzodiazepines, stimulants, and cannabis all interact with entirely separate sets of brain and body systems. When someone stops using, those specific systems react in their own unique ways—just like different musical instruments making their own distinct sounds when you stop playing them.
| Substance Type | Primary Symptoms | Medical Risk Level |
|---|---|---|
| Alcohol & Benzodiazepines | Seizures, high blood pressure, delirium | High (Life-Threatening) |
| Opioids (Heroin, Fentanyl) | Muscle aches, nausea, intense cravings | Moderate to High |
| Stimulants (Meth, Cocaine) | Severe depression, anhedonia, fatigue | Moderate |
For example, alcohol and benzodiazepine withdrawal can be incredibly dangerous because they directly affect the brain’s calming signals. Stopping these drugs suddenly may lead to seizures, high blood pressure, or even life-threatening complications. In contrast, opioid withdrawal rarely causes death directly but often brings intense muscle aches, runny nose, nausea, and powerful cravings. Stimulant withdrawal is more likely to cause deep depression, low energy, and trouble feeling pleasure, while stopping cannabis usually brings sleep problems and irritability.
These differences are key for professionals to understand, because the right medical support depends entirely on the specific symptoms and risks of each drug. Research shows that withdrawal severity is linked to both how long and how much the substance was used, and that medical supervision is especially important for alcohol and benzodiazepine detox due to the risk of seizures and death1.
Life-Threatening Drug Detox Symptoms and Syndromes
Alcohol Withdrawal and Seizure Risk
Alcohol withdrawal can produce some of the most dangerous drug detox symptoms you will manage. When someone who has been drinking heavily for a long time suddenly stops, the brain’s calming system goes into overdrive. It is almost like a car engine revving far too high after the brakes are slammed. Early symptoms might look mild—shakiness, anxiety, sweating—but as a professional, you know things can escalate rapidly.
The biggest danger is the risk of seizures, which usually show up 6 to 48 hours after the last drink. Seizures can be unexpected and life-threatening, often arriving before anyone expects them. In rare but severe cases, people can develop a condition called delirium tremens (DTs), which brings confusion, hallucinations, high blood pressure, and even heart problems. Without medical care, up to 15% of people with severe alcohol withdrawal can die, but with the right monitoring and treatment, that risk drops below 1%8, 2.
Clinical Warning Signs of Delirium Tremens (DTs)
Immediate medical intervention is required if you observe severe confusion, visual or auditory hallucinations, profound dehydration, or a rapidly fluctuating heart rate.
As a provider, your quick action—recognizing warning signs, stabilizing vital signs, and preventing escalation—truly saves lives. Every moment of vigilance counts, and your expertise makes all the difference when withdrawal turns critical. Yes, this work is challenging, but the impact you have is immeasurable.
Benzodiazepine Discontinuation Dangers
Benzodiazepine withdrawal is one of the most serious drug detox symptoms you’ll encounter, and it demands your full, undivided attention. When someone stops taking benzodiazepines—like Xanax, Valium, or Ativan—after regular use, the body’s calming systems become severely overexcited. It’s a bit like pulling the plug on a dam holding back a rushing river: suddenly, everything surges at once, and the brain is left scrambling to restore balance.
Symptoms can start with insomnia, anxiety, and muscle twitching. But the stakes are much higher—seizures, hallucinations, and dangerously high blood pressure are real possibilities. Unlike most withdrawal syndromes, seizures from benzodiazepine detox can happen days or even up to two weeks after the last dose, especially with long-acting medications. These late-onset seizures are unpredictable and can be life-threatening if not recognized early. Protracted withdrawal, with symptoms like anxiety, poor concentration, and sensitivity to light or sound, can linger for months, affecting up to a quarter of patients12.
You know that slow, medically supervised tapers are now considered best practice, as rapid discontinuation sharply raises the risk of crisis. Your vigilance, as a provider, truly protects lives—every careful assessment, every moment of support matters when facing these high-risk drug detox symptoms.
Opioid Withdrawal: Severe But Survivable
Physical Symptoms and Timeline Patterns
Opioid withdrawal brings a cluster of drug detox symptoms that are incredibly tough on the patient but usually not life-threatening on their own. Picture it like a really intense flu, but with even more profound physical discomfort and emotional distress. Symptoms often start within 8 to 24 hours after the last opioid dose.

Common physical symptoms you will observe include:
- Severe muscle aches and bone pain
- Goosebumps, runny nose, and excessive yawning
- Profuse sweating and unusually large pupils
- Nausea, vomiting, diarrhea, and stomach cramps
These gastrointestinal issues make it hard to keep up with basic needs like hydration and nutrition. Anxiety and restlessness are also nearly universal, and many experience strong cravings to use again. The timeline of these symptoms is predictable: they usually peak between 24 and 72 hours after stopping opioids, then slowly improve over the next week. However, the cravings and sleep problems can linger much longer. Providers know that the severity depends on the type of opioid used, how long someone has been using, and their overall health. For example, withdrawal from short-acting opioids like heroin comes on fast, while long-acting opioids stretch symptoms out over more days4.
Why 90% Relapse Without Support
Relapse rates after opioid detox are shockingly high—up to 90% of people return to use without ongoing support or medication-assisted treatment (MAT). Why is it so tough for patients to stay sober after making it through the worst drug detox symptoms? The answer lies in how withdrawal fundamentally alters both the body and the mind.
Even when the physical symptoms fade, people often face intense cravings, mood swings, and trouble sleeping. It’s like finishing a grueling marathon only to find there’s another steep hill just ahead. The brain’s reward system is still out of balance, and everyday stressors can feel completely overwhelming. Without support—like therapy, group counseling, or medications that help reduce cravings—the urge to use again can be overpowering. This is why ongoing care is not just helpful, but absolutely essential for long-term success.
Research makes it clear: medication-assisted treatment and structured aftercare can cut relapse rates in half and save lives4, 16. Every bit of support you provide—whether it’s a listening ear, a safe environment, or help accessing therapy—matters. Recovery is a journey, and nobody should have to walk it alone.
Stimulant and Cannabis Withdrawal Effects
Depression and Anhedonia in Stimulant Users
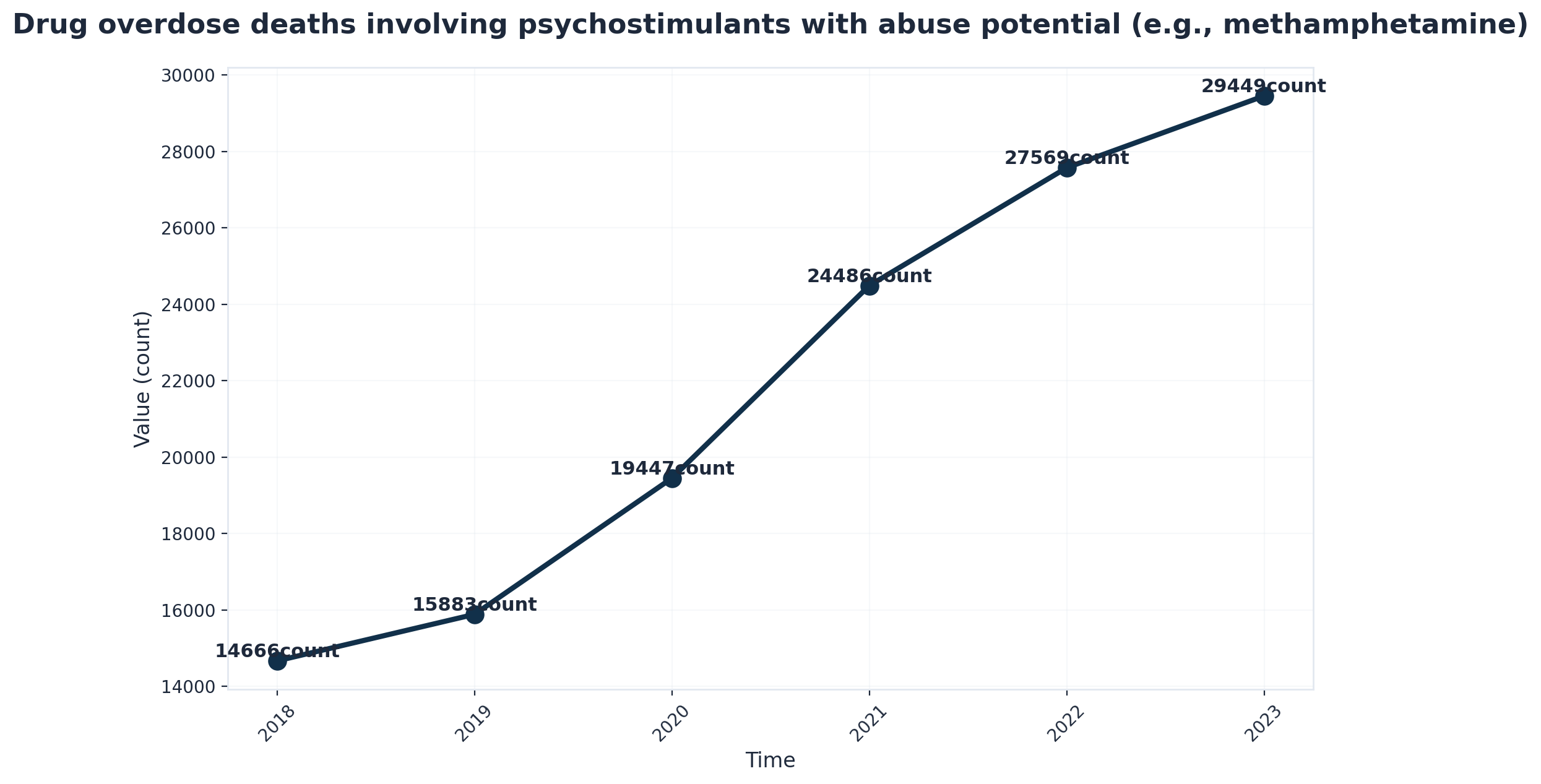
Depression and anhedonia are two of the most challenging drug detox symptoms seen in people withdrawing from stimulants like cocaine and methamphetamine. Anhedonia means not being able to feel pleasure—even from things that used to make them happy, like laughing with friends or enjoying a favorite hobby. Imagine your patient’s brain “reward system” as a battery that suddenly goes dead; nothing seems to recharge it, no matter what you try.
During stimulant withdrawal, people often describe feeling deeply sad, hopeless, or emotionally “flat.” This isn’t just a bad mood—it’s a profound chemical imbalance that can last for weeks and sometimes months. Research shows that these symptoms of depression and anhedonia are not only common, but are among the longest-lasting challenges after quitting stimulants, making relapse more likely if professional support is not available14.
As a professional, you know how tough it can be to watch someone struggle with these invisible pains. Your encouragement, patience, and belief in their progress make a difference every single day. It’s a slow climb, but every small improvement is a real victory.
Cannabis Withdrawal: Often Overlooked
Cannabis withdrawal is often missed or underestimated in clinical settings, but it brings its own set of drug detox symptoms that can severely disrupt daily life. People coming off regular cannabis use may notice they feel more irritable, anxious, or restless than usual. Sleep problems are especially common—many report trouble falling or staying asleep, and some even have vivid or upsetting dreams. Appetite usually drops, and stomach discomfort or headaches can show up too. Think of it like suddenly turning off background music you’ve gotten used to; the silence can feel jarring and uncomfortable.
These symptoms don’t usually threaten physical safety, but they can make staying sober feel much harder. In fact, cravings and mood swings are key triggers for relapse, and research shows most symptoms peak within a week and fade after two weeks, though sleep issues can last longer15.
By noticing and validating these challenges, you give people the support and hope they need to keep moving forward. Next, we’ll review why medical supervision during detox is so important for safety and long-term recovery.
Frequently Asked Questions
What is protracted withdrawal syndrome and how long does it last?
Protracted withdrawal syndrome, also called post-acute withdrawal syndrome (PAWS), is a set of drug detox symptoms that linger long after the initial withdrawal phase has ended. These symptoms can include anxiety, trouble sleeping, mood swings, cravings, and difficulty thinking clearly. Instead of lasting just days, protracted withdrawal can stretch on for weeks or even months. Imagine your mind and body still feeling “off” even after the most intense withdrawal is over—this is PAWS. Studies show that 60–70% of people in recovery experience these ongoing symptoms, making relapse more likely without ongoing support 6.
Can you die from opioid withdrawal even though it’s considered non-fatal?
Opioid withdrawal is known for being extremely uncomfortable, but it is rarely fatal on its own. Unlike alcohol or benzodiazepine withdrawal, which can cause deadly seizures, opioid withdrawal mostly brings severe flu-like symptoms—like vomiting, diarrhea, muscle aches, and anxiety. However, there are exceptions. Death can happen if dehydration from vomiting and diarrhea isn’t treated, or if someone with serious health conditions faces complications. The greatest risk comes when a person relapses after detox: lowered tolerance can lead to accidental overdose, which is often deadly. That’s why quick, supportive care and medical monitoring during drug detox symptoms is so important for safety 4.
How do fentanyl withdrawal symptoms differ from other opioids?
Fentanyl withdrawal shares many drug detox symptoms with other opioids, such as muscle aches, chills, anxiety, nausea, and diarrhea. However, fentanyl’s high potency and short half-life mean withdrawal comes on faster and feels more intense for many people. Symptoms may start within a few hours of the last dose and can be more severe than heroin or oxycodone withdrawal. People often describe rapid mood swings, extreme restlessness, body pain, and trouble sleeping. Cravings can be overwhelming, increasing the risk of relapse. Because illicit fentanyl is so strong, medical monitoring is especially important during detox to manage symptoms safely and support recovery 4.
What medications are used during medical detox to manage symptoms?
Several medications can help manage drug detox symptoms and keep your patients safe during withdrawal. For alcohol or benzodiazepine withdrawal, doctors often use benzodiazepines to prevent seizures and calm the nervous system. Opioid withdrawal may be treated with buprenorphine or methadone to ease cravings and reduce physical discomfort. Clonidine is sometimes used to lower anxiety and blood pressure. For people struggling with severe nausea or trouble sleeping, medications like anti-nausea pills or sleep aids can be added. These treatments are chosen based on the person’s symptoms, history, and safety needs. Medication-assisted treatment is proven to double treatment success and cut relapse risk by half 9.
How do you know if withdrawal symptoms require emergency medical attention?
Emergency medical attention is needed for drug detox symptoms when you see signs like seizures, chest pain, trouble breathing, confusion, or a high fever. These can signal dangerous complications—especially during alcohol or benzodiazepine withdrawal, where seizures and delirium can be fatal without quick care. If someone becomes unresponsive, has severe vomiting or diarrhea causing dehydration, or their heart rate or blood pressure is unstable, it’s time to act fast. Trust your instincts—if something feels off or escalating, immediate evaluation is the safest move. Early intervention can prevent life-threatening outcomes and gives your patient the best shot at recovery 1.
Is it safe to detox at home or should you always seek medical supervision?
Detoxing at home might seem convenient, but it can be risky, especially with substances like alcohol or benzodiazepines. Some drug detox symptoms—like seizures, confusion, or dangerously high blood pressure—can come on suddenly and may be life-threatening without immediate medical care. Even with opioids or stimulants, severe vomiting, dehydration, or mental health crises can put someone in danger. Medical supervision means professionals can spot warning signs early and provide treatments that reduce complications and save lives. Research strongly recommends medical monitoring for withdrawal from high-risk substances to prevent emergencies and keep patients safe 1.
Medically Supervised Detox Saves Lives
When a patient is going through withdrawal, their body is under serious physiological stress. Alcohol and benzodiazepine withdrawal can be life-threatening without proper medical care. Seizures, dangerous blood pressure spikes, and heart complications can happen suddenly—and these aren’t risks anyone should face alone. That’s why Pacific Crest Trail Detox (PCTD) provides 24/7 medical supervision in a comfortable, home-like residential environment in Milwaukie, Oregon. Here, trained professionals monitor vital signs around the clock, ready to intervene immediately if complications arise.

At PCTD, we combine compassionate support with evidence-based medical care. Our team provides medication-assisted treatment (MAT) to ease symptoms safely, making withdrawal more manageable while keeping patients medically stable.
// PCTD Clinical Tracking Protocol Example
System: ERPHealth Software
Action: Log Patient Vitals -> Press Enter
Outcome: Statistically-significant treatment results tracked in real-time.
We track every patient’s outcomes using specialized ERPHealth software to measure real results—because safety and success matter. This isn’t a cold, clinical hospital setting. It’s a supportive space where nurses and doctors understand what patients are experiencing and respond to changing needs with personalized care.
Here’s something important to know as an industry peer: detox without follow-up care has only an 8% success rate. That’s why we don’t just help patients get through withdrawal—we guide them through a complete continuum of care. After medical detox, individuals can transition seamlessly into our partial hospitalization program (PHP), intensive outpatient program (IOP), or standard outpatient services. We also offer specialized programs tailored for LGBTQ+ individuals, veterans, professionals, and anyone dealing with co-occurring mental health disorders like depression, anxiety, or PTSD.
Every recovery story starts with that first brave decision to get help, and as a professional, you are instrumental in guiding them there. PCTD accepts most insurance plans (excluding OHP) and proudly serves the Portland metro area and broader Pacific Northwest region. Whether your patients are struggling with alcohol, opioids, benzodiazepines, or other substances, our proven approach combines medical expertise with genuine compassion. Ready to learn more about how our personalized care can support your clients’ recovery journey? Reach out today—the path to lasting recovery starts here.
References
- Mayo Clinic – Drug Withdrawal Symptoms and Treatment. https://www.mayo.edu/patient-visitor-guide/conditions-and-diseases
- CDC – Fetal Alcohol Spectrum Disorders and Alcohol Withdrawal Information. https://www.cdc.gov/ncbddd/fasd/index.html
- National Institutes of Health – Research News on Substance Use and Withdrawal. https://www.nih.gov/news-events/news-releases
- UpToDate – Opioid Withdrawal Clinical Reference. https://www.uptodate.com/contents/opioid-withdrawal
- American Psychiatric Association – DSM-5 Substance Withdrawal Criteria. https://www.americanpsychiatry.org/psychiatrists/practice/dsm
- National Center for Biotechnology Information – Protracted Withdrawal Syndrome Review. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6002647/
- World Health Organization – Substance Use Disorder Management Guidelines. https://www.who.int/publications-detail/management-of-substance-use-disorders
- Alcohol Withdrawal – StatPearls, National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK430973/
- SAMHSA – Medications for Substance Use Disorders. https://www.samhsa.gov/medications-substance-use-disorders
- National Institute on Drug Abuse – Treatment and Recovery Science. https://www.nida.nih.gov/publications/drugs-brains-behavior-science-addiction/treatment-recovery
- Opioid Withdrawal – StatPearls, National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK482157/
- Benzodiazepine Withdrawal – StatPearls, National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK555893/
- SAMHSA National Helpline – Substance Abuse and Mental Health Services Administration. https://www.samhsa.gov/find-help/national-helpline
- Stimulant Withdrawal and Protracted Withdrawal Syndrome – PubMed/Medical Literature. https://www.ncbi.nlm.nih.gov/pubmed/34662234
- Cannabis Withdrawal Syndrome – StatPearls, National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK482151/
- Opioid Overdose Crisis – National Institute on Drug Abuse. https://www.nida.nih.gov/research-topics/opioids/opioid-overdose-crisis





