Key Takeaways
When evaluating drug rehabilitation programs for your adult child, keep these critical factors in mind to ensure you are making the most informed, clinical, and compassionate choice possible:
- Decision Flowchart: Assess immediate medical risk → Choose medical detox if high risk (especially for alcohol or benzodiazepines) → Transition to Partial Hospitalization (PHP) or Intensive Outpatient (IOP) → Engage in long-term alumni services.
- Top 3 Success Factors: 1) A full continuum of care (increases success from a mere 8% to significantly higher margins), 2) Medication-Assisted Treatment (reduces opioid relapse by up to 50%), and 3) Standardized assessments (boosts program completion by 23%).
- Immediate Next Action: Verify your insurance benefits (excluding OHP) and schedule a standardized clinical assessment to determine the appropriate level of care for your loved one.
Why Comprehensive Care in Drug Rehabilitation Programs Matters More Than Detox Alone
The 8% Reality: Detox Without Follow-Up
Checklist: Are You Falling Into the Detox-Only Trap?
- Has your loved one completed a medical detox but not entered any follow-up care?
- Are you seeing a cycle of relapse after each detox attempt?
- Is there a clear plan for therapy, peer support, or ongoing clinical monitoring?
- Does the program offer a pathway beyond withdrawal management?
If you answered “yes” to the first two questions, it is time to reconsider the approach. As a professional, you understand data, and the data here is stark.

Only 8% of people who go through detox without follow-up treatment achieve sustained recovery—meaning 92% will likely relapse without further support1.
That number can feel staggering, and it is perfectly natural to feel frustrated or even hopeless after repeated setbacks. But every step, even a failed attempt, brings new insight and a chance to build a better plan. Drug rehabilitation programs that stop at detox alone may provide physical stability, but they rarely address the underlying patterns, mental health challenges, or environmental triggers that drive substance use4.
Long-term recovery almost always requires a blend of therapy, support groups, and structured aftercare. If you are supporting an adult child, encouraging post-detox engagement with clinical care is one of the most effective ways to change the outcome. At Pacific Crest Trail Detox (PCTD) in Milwaukie, Oregon, we emphasize that detox is merely the stabilization phase. We provide a warm, home-like residential environment rather than a sterile hospital setting, ensuring your loved one feels safe as they prepare for the real work of recovery.
This approach works best when you view detox as just the first mile of a much longer journey. Up next, we will explore how the continuum of care model creates a real foundation for lasting recovery.
Understanding the Continuum of Care Model
Decision Tool: Mapping the Continuum of Care
- Is your loved one moving directly from detox to ongoing therapy or group support?
- Does the program outline clear steps from medical stabilization through outpatient and aftercare?
- Are regular reassessments and adjustments to the plan part of the process?
If you can check all three, you are likely in a program that values the full continuum of care—a model proven to give people the best chance at lasting change. The continuum of care refers to a coordinated series of treatment levels, beginning with detox and extending through residential, outpatient, and aftercare services.
Each level is designed to meet a person’s changing needs as they progress in recovery. For example, someone might start in a medically supervised detox (typically a 3 to 7-day time investment), transition to partial hospitalization or intensive outpatient therapy (spanning 2 to 6 weeks), and eventually move into ongoing alumni support groups. Consider this method if you want a clear, step-by-step framework that adapts to setbacks or progress, rather than a one-and-done solution.
Programs using this model address not just withdrawal, but also mental health, relapse prevention, and life skills—building a foundation for real stability. Research shows that coordinated care across multiple stages, not just detox, is consistently linked to stronger outcomes and lower relapse rates4. If you are supporting an adult child through these steps, remember that every transition is progress—even when it feels slow.
Medical Supervision and Evidence-Based Treatment
When Medical Detox Becomes Life-Saving
As a professional, you know that assessing risk is the first step in any intervention. When it comes to substance withdrawal, that risk can be fatal.
| Risk Factor / History | Clinical Recommendation |
|---|---|
| Heavy, recent use of alcohol or benzodiazepines | 24/7 Medical Detoxification (High seizure risk) |
| History of severe withdrawal or co-occurring physical conditions | Inpatient Sub-Acute Detox with continuous monitoring |
| Signs of confusion, hallucinations, or unstable vital signs | Immediate emergency medical intervention |
If your loved one falls into any of these categories, medical detox—meaning withdrawal under the care of trained professionals—may be not just safer, but life-saving. Medical detox involves 24/7 supervision, access to emergency care, and evidence-based protocols for managing withdrawal symptoms safely. For substances like alcohol and benzodiazepines, withdrawal can cause seizures or even death if not medically managed, making routine monitoring and intervention absolutely essential4.
This strategy suits families that have watched their loved one experience dangerous withdrawal symptoms or who may be at risk due to other health issues. Facilities with strong medical supervision can intervene early if complications arise, giving you peace of mind during a highly stressful transition. At PCTD, we specialize in these high-risk detox cases, providing compassionate, personalized care with proven results.
Medical detox is often completed within 3–7 days, but the process can be longer for those with complex needs. The time and resources required depend on the substance, history, and individual health risks. While inpatient detox may feel daunting at first, seeing your loved one stabilized—and knowing their immediate safety is protected—counts as a huge win on the path to long-term recovery.
Medication-Assisted Treatment: 50% Relapse Reduction
Medication-Assisted Treatment (MAT) Checklist: Is MAT Right for Your Loved One?

- Has your loved one struggled with opioid or alcohol relapse after traditional treatment?
- Are cravings or withdrawal symptoms making it hard to maintain progress?
- Is there a history of multiple failed attempts at abstinence-only programs?
If you see these patterns, MAT could be a powerful next step. Medication-Assisted Treatment combines FDA-approved medications like buprenorphine, methadone, or naltrexone with counseling and behavioral therapies. MAT addresses both the physical and psychological aspects of addiction, helping to stabilize brain chemistry and reduce cravings.
For opioid addiction in particular, MAT can lower the risk of relapse by 50%—a significant difference when every effort counts7. Opt for this framework when you are supporting an adult who has cycled through detox or therapy without long-term results. It is also a fit for individuals facing intense cravings or withdrawal symptoms that make other approaches feel impossible.
MAT is not a shortcut or a sign of failure—it is an evidence-based path that increases the odds of sustained recovery, especially when paired with ongoing therapy and support groups2. When navigating insurance portals to verify coverage for these services, you might need to press Submit on specific inquiries regarding outpatient pharmacy benefits or use clinical billing codes like H0008 for sub-acute detox and MAT services.
Programs offering MAT often require regular medical supervision, monitoring, and a commitment to therapy. Some programs are outpatient, requiring a few clinic visits per week, while others offer residential support for those with higher needs. Time investment varies: initial stabilization often takes a few days, with ongoing support lasting months to years, depending on individual progress.
Individualized Assessment and Treatment Matching
Why Standardized Assessment Tools Boost Success by 23%
Assessment Checklist: Is Your Loved One Receiving a Standardized Intake?
- Did the program use a structured interview or tool (like the ASAM Criteria) to evaluate medical, psychological, and social needs?
- Were co-occurring mental health issues screened at admission?
- Did you receive a written summary of findings before treatment began?
If all boxes are checked, your loved one is likely benefiting from a best-practice approach—one proven to boost completion rates. Standardized assessment tools are structured questionnaires or protocols used at intake to gather consistent, detailed information about a person’s substance use, health, and environment.
These tools help programs identify the right intensity of care and tailor services to individual needs, rather than relying on guesswork or one-size-fits-all plans. To give you an idea of how clinical teams process this data, consider this simplified logic model:
// Clinical Assessment Logic Example
Assessment_Score = (Medical_Acuity 1.5) + (Psychological_Stability 1.2) + Recovery_Environment_Risk;
if (Assessment_Score > 15) {
Recommend_Level = "Inpatient Medical Detox / PHP";
} else {
Recommend_Level = "Intensive Outpatient (IOP)";
}
Research shows that programs using standardized assessments at intake achieve 23% higher treatment completion rates than those that do not4. This difference matters: completion is a major predictor of sustained recovery. This path makes sense for families who want a more predictable, data-driven pathway that adapts to setbacks and progress, instead of trial and error.
The time investment for a thorough intake can range from 60 to 120 minutes, depending on complexity. Most programs require licensed clinicians to conduct these assessments, ensuring medical and psychological factors are fully considered. Yes, this is a more involved process upfront, but it is worth every minute when the odds of recovery rise.
Addressing Co-Occurring Disorders (70% of Cases)
Integrated Care Checklist: Is Your Loved One’s Program Equipped for Dual Diagnosis?
- Are mental health and substance use disorders treated together, not separately?
- Does the clinical team include both addiction and mental health specialists?
- Are medications for depression, anxiety, or other diagnoses offered as part of the plan?
If you can answer yes to these, your loved one’s care team is likely following best practices for co-occurring disorders. The term “co-occurring disorder” means someone has both a substance use disorder and a mental health condition (such as depression, anxiety, PTSD, or bipolar disorder).
This is more common than many realize—about 70% of people seeking addiction treatment also have a co-occurring mental health issue6. This approach is ideal for families who have noticed mood swings, trauma symptoms, or severe anxiety alongside substance use. Programs that offer integrated treatment—addressing both addiction and mental health together—are proven to outperform those that separate these needs.
At PCTD, we provide specialized programs for specific populations, including LGBTQ+ individuals, veterans, professionals, and those with co-occurring mental health disorders. Programs should provide access to therapy, medication management, and peer support, often requiring a treatment team with cross-specialty training.
Expect a more resource-intensive approach: integrated care often means a longer initial assessment (up to 2 hours), frequent therapy sessions, and medication monitoring, with overall treatment lasting several months. Yes, it is a significant investment of time and trust, but supporting both sides of the struggle gives your loved one a real chance at lasting change6.
Accreditation and Outcomes Tracking in Drug Rehabilitation Programs
You have already learned so much through this journey—you know that finding quality treatment isn’t just about getting through detox, it’s about building a foundation for lasting recovery. The decisions you’re making right now, even when they feel overwhelming, show incredible commitment to your loved one’s future. And you’re asking exactly the right questions about how to recognize programs that deliver real results.
Accreditation from organizations like The Joint Commission or CARF International provides important validation that a facility meets rigorous standards for safety and evidence-based care. You already understand these benchmarks matter—they’re the baseline that ensures medical protocols, staff qualifications, and treatment approaches meet professional standards. But as you know, credentials alone don’t tell the whole story about whether a program truly supports long-term recovery.
What makes the difference is how facilities track and measure their actual outcomes. Quality programs use specialized systems to follow clients through their entire recovery journey, gathering real data about what’s working.
At Pacific Crest Trail Detox, we differentiate ourselves through measured outcomes using ERPHealth software to track statistically-significant treatment results. We don’t just look at completion rates; we look at meaningful progress markers that show whether our approach is truly helping people build sustainable recovery.
This kind of transparency matters because it reflects a commitment to continuous improvement and accountability. Here’s something you’ve likely encountered in your research: detox alone has only an 8% success rate without follow-up care. That sobering statistic reinforces what you already understand—comprehensive treatment that connects medical detox to ongoing support makes all the difference.
Programs offering a true continuum of care, from medically supervised withdrawal management through outpatient services and aftercare, create the pathway your loved one needs. It’s not about a single intervention; it’s about sustained support that adapts as recovery progresses. Consider this route if you want a facility that treats addiction as a chronic condition requiring long-term management rather than an acute issue to be “cured” in a week.
The environment where treatment happens shapes the experience too. A home-like setting rather than a clinical hospital atmosphere can help your loved one feel more comfortable engaging with the difficult work of recovery. When medical expertise combines with genuine compassion and personalized attention—whether that’s specialized programming for veterans, LGBTQ+ individuals, professionals, or those managing co-occurring mental health challenges—treatment becomes more than just medical intervention. It becomes a partnership.
You’re navigating this with wisdom and care, looking beyond surface-level promises to find programs that demonstrate their commitment through measured results and comprehensive support. The facilities that openly share their outcomes data, maintain their accreditations, and continuously refine their approaches based on what actually works—those are the partners who understand that your loved one’s recovery is a journey, not just a destination. Your dedication to finding that level of quality care is already making a difference, even on the hardest days.
Frequently Asked Questions
How do I choose between residential and outpatient programs for my loved one?
Choosing between residential and outpatient drug rehabilitation programs depends on your loved one’s stability, support network, and clinical needs. Residential treatment offers 24/7 structure and is ideal when safety, severe withdrawal, or a history of relapse are concerns. Outpatient programs work well for those with strong family support, reliable housing, and milder symptoms. The National Institute on Drug Abuse notes that program effectiveness is less about setting and more about matching care to individual needs through standardized assessment 2. Consider residential if home triggers or co-occurring disorders create added risks; outpatient suits those needing flexibility to maintain work or family life. Whichever path you choose, ongoing engagement and aftercare remain essential for long-term recovery.
What should I expect to pay for quality addiction treatment, and will insurance cover it?
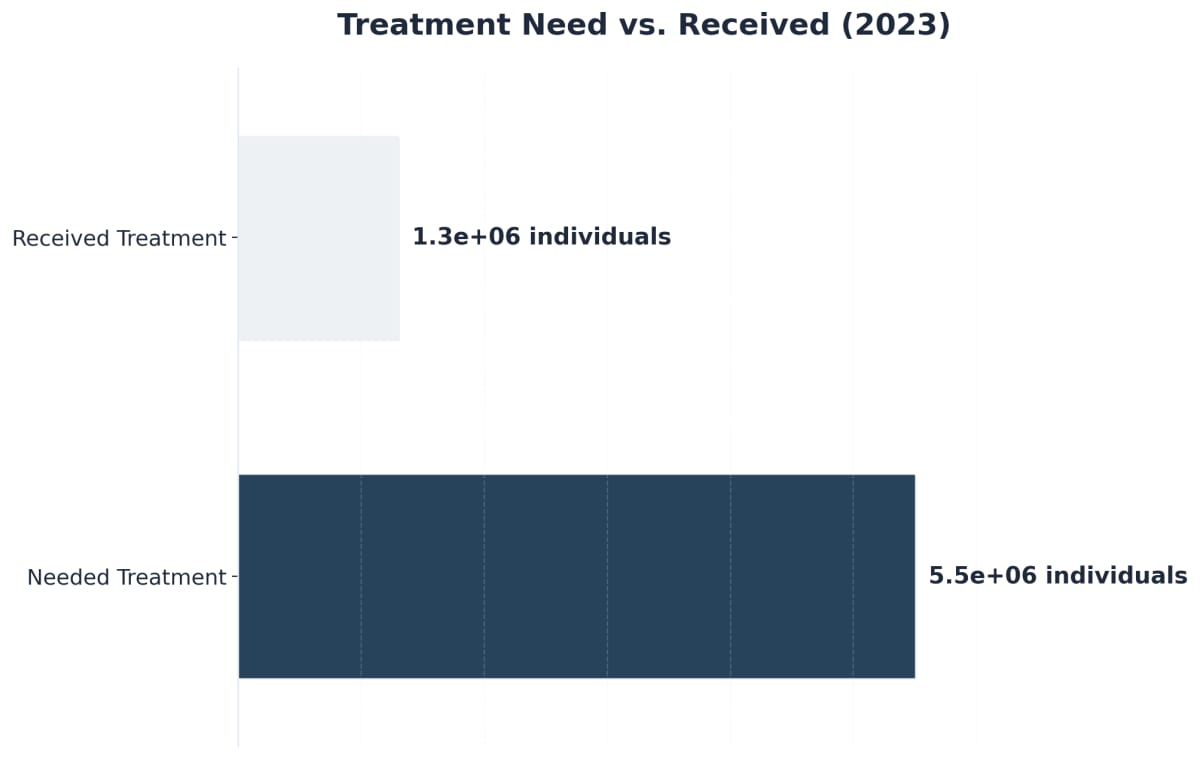
The cost of quality addiction treatment varies widely depending on the level of care, length of stay, and services provided, but many drug rehabilitation programs work with private insurance or Medicaid to offset expenses. Insurance coverage is a key factor—plans often cover medical detox, outpatient, and sometimes residential care, though pre-authorization and network restrictions may apply. Accessing treatment can still be challenging; in 2023, only 1.3 million of the 5.5 million people needing substance use treatment actually received it, with insurance coverage barriers cited as a common obstacle 8. Be sure to verify insurance acceptance, out-of-pocket responsibilities, and any financial assistance options before admission.
How long does the full treatment process typically take from detox through aftercare?
The full process in drug rehabilitation programs usually spans several stages, each with its own timeframe. Medical detoxification can last 3–7 days, depending on substance and health history. Residential or partial hospitalization typically ranges from 2 to 6 weeks. Intensive outpatient or standard outpatient therapy may continue for several months, with aftercare and alumni support extending a year or more. While every case is unique, most families should expect the journey from detox through long-term aftercare to take at least 3–12 months for meaningful progress 4. Remember, steady participation at each step is linked to better outcomes and lasting recovery.
What’s the difference between CARF and Joint Commission accreditation, and does it matter?
CARF (Commission on Accreditation of Rehabilitation Facilities) and The Joint Commission are both respected organizations that accredit drug rehabilitation programs, but their focus differs slightly. CARF emphasizes person-centered care, measurable outcomes, and ongoing quality improvement, while The Joint Commission is known for its rigorous patient safety and clinical standards, including medication management and infection control 39. Both require regular independent surveys and public reporting of results. For families, either accreditation signals a strong commitment to quality, though some programs may choose one based on their clinical strengths or patient population. Accreditation matters—a program with either mark has met national benchmarks for safety and results.
How can I verify a program’s success rates and outcomes data before committing?
To verify a program’s success rates and outcomes data, start by asking for recent statistics on treatment completion, relapse rates, and patient satisfaction—high-quality drug rehabilitation programs should track and openly share this information using validated tools, not just internal surveys. Confirm if outcomes are reported to accrediting bodies like CARF or The Joint Commission, as these organizations require regular, independent data audits for continued accreditation 39. According to the Institute of Medicine, outcome measurement should be a routine component of all addiction treatment programs 4. Don’t hesitate to request specific examples or reports—transparency here signals a program’s commitment to accountability and continuous improvement.
What questions should I ask during a facility tour to assess quality of care?
When touring a facility, ask about accreditation—are they certified by CARF or The Joint Commission? Inquire how drug rehabilitation programs measure and publish outcomes like completion and relapse rates, and request recent data to see if they use validated tools, as recommended by the Institute of Medicine 4. Explore their process for individualized assessments and treatment planning. Find out if licensed clinicians handle intake and ongoing care, and whether integrated mental health and substance use treatment is available. Finally, observe staff interactions, safety protocols, and the environment—do you sense a supportive, respectful culture? Every thoughtful question brings you closer to the right fit for long-term recovery.
Is telehealth treatment as effective as in-person programs for substance use disorders?
Telehealth treatment can be just as effective as in-person drug rehabilitation programs for many people with substance use disorders, especially when services are structured and evidence-based. Recent updates from national agencies highlight that outcome quality depends more on program design, therapist skill, and ongoing support than on whether care is delivered virtually or face-to-face 24. Telehealth expands access for those in rural areas, with mobility issues, or facing transportation barriers. This solution fits families seeking flexibility or continued care after residential treatment, but it does require reliable internet and private space for sessions. Program completion and satisfaction rates for telehealth are comparable to traditional models when best practices are followed 4.
Your Path Forward: Choosing Evidence-Based Care
You’ve spent this entire article looking at data, outcomes, and what quality care really means—because that’s who you are professionally. But right now, in this moment, you’re also standing at one of the hardest crossroads a parent faces. That dual reality—knowing what evidence-based treatment looks like while feeling the weight of needing it for your own child—that’s an incredibly difficult space to occupy.
We see you there, and we want you to know: the fact that you’re here, researching and learning, already demonstrates the kind of commitment that makes recovery possible. The transition from understanding what works to finding where that care exists doesn’t have to feel overwhelming. Comprehensive treatment isn’t just a concept—it’s a lived experience that unfolds across time.
At Pacific Crest Trail Detox, for example, that journey might begin with medically supervised detox (because as you know, withdrawal from substances like alcohol and benzodiazepines requires careful medical oversight). It then moves through partial hospitalization when someone needs structured support while rebuilding daily routines, continues into intensive outpatient care as independence grows, and extends into alumni services that provide ongoing connection long after formal treatment ends. This continuum isn’t about upselling services—it’s about matching care intensity to where someone actually is in their recovery journey.
What matters most isn’t finding perfection; it’s finding partnership. You need a team that tracks real outcomes because you understand what measurement means. You need transparency about methods because you know the questions to ask. You need people who see your loved one as a whole person—addressing not just the addiction but any co-occurring mental health challenges that fuel it—because you’ve always known recovery isn’t one-dimensional.
This solution fits families who are ready to move beyond the cycle of relapse and invest in a structured, compassionate future. This path forward isn’t easy, but you’re not walking it alone. Your professional knowledge is an asset here, not a burden. Your parental love is a strength, not a weakness. Together, they make you exactly the advocate your loved one needs right now. Trust yourself. Trust the process. And know that choosing evidence-based care isn’t just a clinical decision—it’s an act of hope, grounded in science and delivered with genuine compassion.
References
- SAMHSA National Helpline – Referral and Information Service. https://www.samhsa.gov/find-help/national-helpline
- Principles of Drug Addiction Treatment: A Research-Based Guide. https://www.nida.nih.gov/publications/principles-drug-addiction-treatment-research-based-guide
- CARF International – Accreditation Standards. https://www.carf.org/Provider/
- SAMHSA Treatment Improvement Protocols – Comprehensive Overview. https://www.samhsa.gov/sites/default/files/programs_campaigns/brss_tacs/final-tip-series-narrative_508c.pdf
- American Psychological Association – Treatment Resources. https://www.apa.org/science/about/psa/addiction/treatment
- NAMI – Co-Occurring Mental Health and Substance Use Disorders. https://www.nami.org/Get-Involved/Advocacy/Policy-Priorities/Substance-Use-Disorders-and-Mental-Health
- CDC – Opioid Overdose Prevention. https://www.cdc.gov/drugoverdose/prevention/index.html
- SAMHSA National Survey on Drug Use and Health – Detailed Tables. https://www.samhsa.gov/data/sites/default/files/reports/rpt35325/NSDUHDetailedTabs2023.pdf
- The Joint Commission – Healthcare Accreditation Standards. https://www.jcaho.org/
- American Society of Addiction Medicine – Patient Placement Criteria. https://www.asam.org/public/patient-placement





