Key Takeaways
- Access is limited but crucial: Only 25% of individuals receive the medication they need, highlighting the importance of advocating for comprehensive care.
- Overdose risks drop significantly: Engaging in medication-assisted treatment cuts the risk of fatal overdose by half.
- Retention doubles with medication: MAT keeps 54% of people in treatment at one year, compared to 20-30% in abstinence-only programs.
- Editor’s Pick: The most critical takeaway is that combining medical detox with ongoing pharmacological and behavioral support is the proven path to long-term recovery.
Why These Medication Assisted Treatment Statistics Matter to Your Recovery
Understanding these medication assisted treatment statistics isn’t just about numbers on a page—it’s about recognizing where you stand in the healing process and what support you truly need. Seeing that only a fraction of people receive pharmaceutical intervention for addiction, or that certain barriers keep many from getting help, reveals real obstacles that might be affecting the path ahead.
At Pacific Crest Trail Detox (PCTD) in Milwaukie, Oregon, we provide a warm, home-like environment where you can safely begin your healing journey. We know that medical detox combined with counseling and medication gives you the best foundation for success. These numbers matter because they validate what you might already be experiencing. If you’ve felt like getting the right treatment is harder than it should be, the reality matches that perception. The data confirms that access gaps exist, and understanding them helps navigate around these challenges more effectively.
More importantly, knowing these statistics empowers self-advocacy. Understanding that research-backed treatments like pharmacological therapy paired with behavioral support offer the strongest outcomes means asking better questions and seeking out comprehensive care rather than settling for partial solutions. Every step toward understanding available options brings sustainable healing closer.
These insights also remind you that others face these same challenges. Thousands of people are walking similar paths, encountering similar barriers, and finding ways through. The journey to wellness matters, and having the full picture helps make informed decisions about care.
Your Path Forward Starts with Evidence
Recovery isn’t about guessing what might work—it’s about choosing treatments backed by real science and proven results. As you prepare to take that next step, you deserve care that’s built on evidence, not empty promises. Medical detox combined with pharmacological support and counseling gives you the strongest foundation for lasting change.
These approaches work together to address both the physiological and emotional sides of opioid dependence, helping you move forward safely and with support every step along this journey. Your journey matters, and so does the quality of care you receive. Look for programs that track their outcomes, offer comprehensive services from detox through aftercare, and create a supportive environment where you can heal.
| Treatment Approach | Estimated Success Rate |
|---|---|
| Detox Without Follow-Up Care | 8% |
| Medical Detox + MAT + Comprehensive Aftercare | Significantly Higher |
Remember, detox alone has only an 8% success rate—but combining medical supervision with ongoing therapy and support dramatically improves your chances for long-term wellness. At PCTD, we use advanced tools like ERPHealth software to track your progress and ensure our treatments are working for you.
Data Insight: Personalized Care + MAT + Alumni Services = Sustainable Recovery
You’ve already shown courage by exploring your options. Now it’s time to choose a path that honors your commitment with scientifically-validated care, compassionate support, and proven results. To keep this information handy, you can press Ctrl + D (or Cmd + D on a Mac) to bookmark this page. Your healing starts here.
References
- Treatment for Opioid Use Disorder: Population Estimates. https://www.cdc.gov/mmwr/volumes/73/wr/mm7325a1.htm
- A Comparison of Medication-Assisted Treatment Options for Opioid Use Disorder. https://pmc.ncbi.nlm.nih.gov/articles/PMC11805484/
- Buprenorphine/Naloxone and Methadone Maintenance Treatment: Outcomes from a Randomized Trial. https://pmc.ncbi.nlm.nih.gov/articles/PMC3711351/
- Retention of Participants in Medication-Assisted Programs in Low- and Middle-Income Countries. https://pmc.ncbi.nlm.nih.gov/articles/PMC5312702/
- Drug Overdose Deaths in the United States, 2023–2024. https://www.cdc.gov/nchs/products/databriefs/db549.htm
- Retention Strategies for Medications for Addiction Treatment. https://www.ncbi.nlm.nih.gov/books/NBK560309/
- Medication-Assisted Treatment for Opioid Use Disorder. https://www.cdc.gov/overdose-resources/files/medication-assisted-treatment-for-opioid-use-disorder.html
- Opioid Use Disorder: Current Trends and Potential Treatments. https://pmc.ncbi.nlm.nih.gov/articles/PMC11254342/
- Economic Benefits of Substance Use Disorder Treatment. https://pmc.ncbi.nlm.nih.gov/articles/PMC10850316/
- Racial and Ethnic Disparities in Medication for Opioid Use Disorder Access, Use, and Treatment Outcomes in Medicare. https://pubmed.ncbi.nlm.nih.gov/38135120/
1. Only 25% Get the Medication They Need
Here’s a reality that might surprise you: even though medications combined with therapy work incredibly well for opioid use disorder, only about 1 in 4 people who need it actually receive it. That’s a massive gap between what’s available and who’s getting help, as highlighted by recent CDC population estimates1.
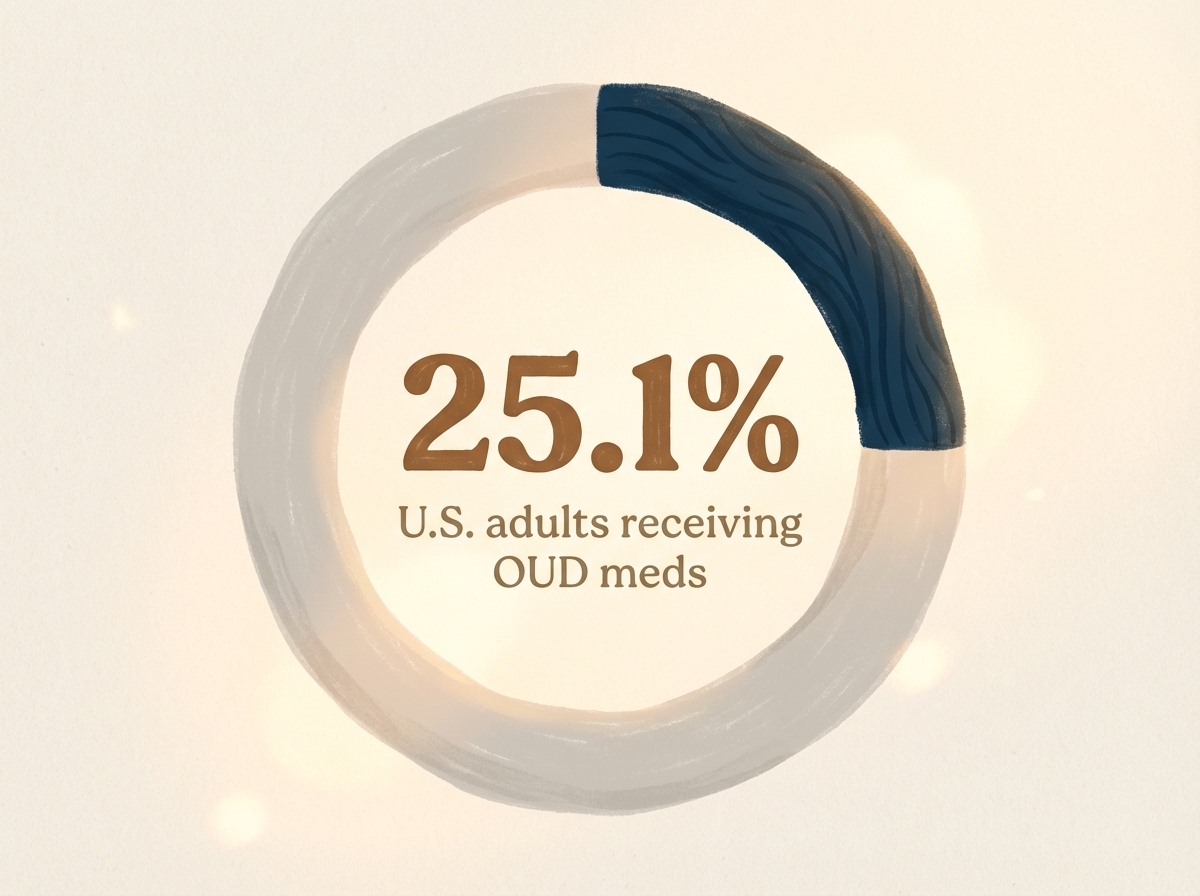
Think about that for a moment. If you’re struggling with opioid use disorder, you’re facing barriers that three-quarters of people in similar situations can’t overcome. These obstacles might include limited provider availability for this type of care, insurance complications, stigma around using medications like methadone or buprenorphine, or simply not knowing where to turn for research-backed treatment.
This treatment gap isn’t just a statistic—it represents real people who continue struggling while effective help exists. Many facilities still don’t offer pharmaceutical interventions alongside therapy, even though research consistently shows it’s one of our most effective approaches for opioid use disorder. Some programs rely solely on talk therapy without the clinical resources that make recovery more achievable.
The good news? You don’t have to be part of that 75% who miss out. Finding a program that combines medications with behavioral therapy means you’re receiving comprehensive care that supports lasting recovery. This integrated approach addresses both the physiological aspects of dependence as well as underlying factors that contribute to substance use.
Understanding this gap matters because it empowers you to advocate for yourself. You deserve comprehensive treatment that includes medical supervision alongside therapeutic interventions. Whether you’re just starting to explore options or you’ve tried other approaches before, knowing that effective treatment exists—and that you can receive it—is your first step toward a different path forward.
2. MAT Cuts Your Overdose Risk in Half
When you’re struggling with opioid dependence, the statistics can feel overwhelming. But here’s some genuinely hopeful news: MAT cuts your risk of fatal overdose by approximately 50%, a fact supported by comparative medication-assisted treatment studies2. That’s not a small improvement—that’s a life-changing difference that could mean everything for you and the people who care about you.
MAT works by combining FDA-approved medications like methadone or buprenorphine with therapy and behavioral interventions. This comprehensive approach addresses both physical dependency and underlying patterns that fuel addiction. The medications stabilize your brain chemistry, reducing cravings and withdrawal symptoms, while therapy helps you build coping skills you need for lasting recovery.
Think about what a 50% reduction in overdose risk really means. It means safer days as you navigate early recovery. It means your body gets clinical support it needs while you work on healing emotionally and mentally. It means you aren’t white-knuckling through every moment, fighting withdrawal alone.
- Stabilized Brain Chemistry: Reduces the intense physical cravings.
- Emotional Healing: Allows you to focus on therapy without the distraction of severe withdrawal.
- Safer Recovery: Drastically lowers the chances of a fatal relapse.
The evidence is clear: MAT isn’t just about managing symptoms—it’s about giving you a real fighting chance at recovery. By combining medical supervision with clinical therapy, you’re addressing addiction from every angle. This is exactly why scientifically-proven programs emphasize this integrated approach, recognizing that recovery happens as your physical needs and emotional healing work together.
You deserve treatment that’s proven to work. Every step you take toward MAT is a step toward safety, stability, and a future where opioid dependence doesn’t control your life anymore.
3. Treatment Retention Averages 54% at One Year
Staying in treatment is one of the biggest challenges you’ll face in recovery, and you’re far from alone in that struggle. Research shows that medication-based approaches keep about 54% of people engaged at the one-year mark, supported by randomized trial outcomes3. That might not sound like a huge number at first, but here’s why it matters: traditional abstinence-only programs see retention rates drop to around 20-30% at one year. MAT literally doubles your chances of sticking with recovery.
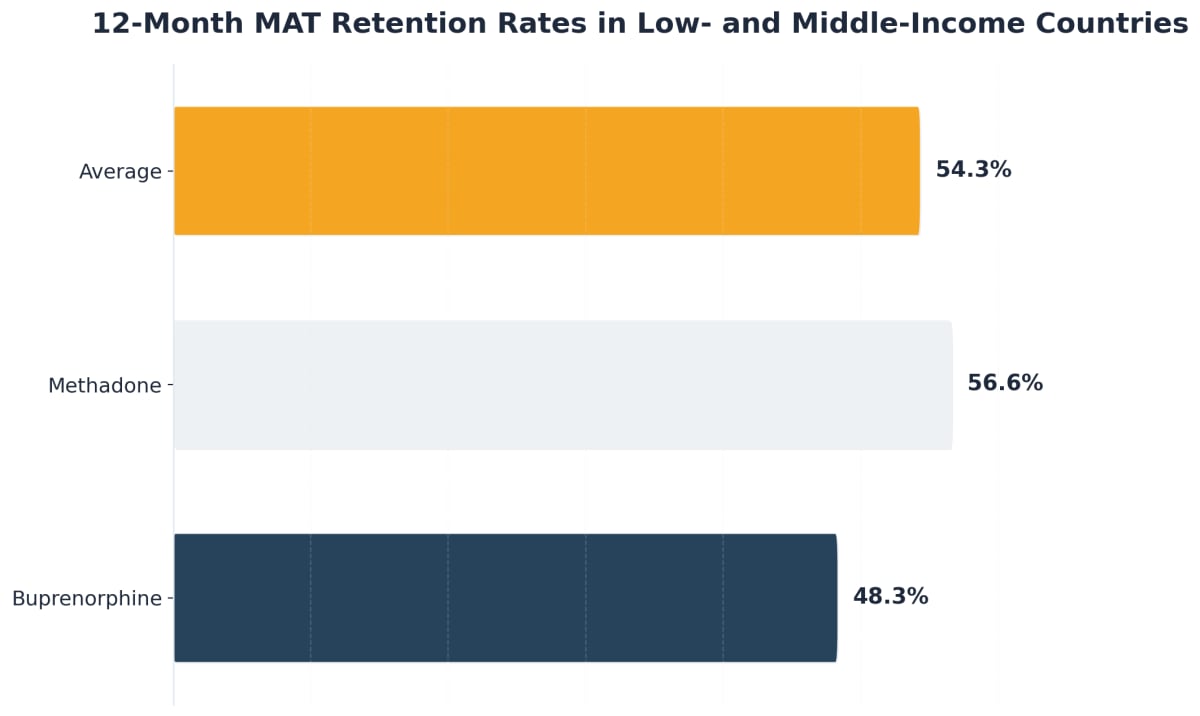
Why does MAT help you stay the course? The medications work with your brain chemistry, not against it. With buprenorphine or methadone, you’re freed from constantly fighting cravings or withdrawal symptoms that make every day feel impossible. You can actually focus on therapy sessions that help you rebuild your life. It’s hard to work on emotional healing when your body is screaming for relief.
Think of it this way: you wouldn’t expect someone with diabetes to manage their condition through willpower alone. MAT gives you clinical support while you develop new coping skills, repair relationships, and figure out what a sober life looks like for you. Combining medication with therapeutic guidance creates a foundation that’s strong enough to support real, lasting change.
Every month you stay in treatment strengthens your path forward. The skills you learn, the support system you build, along with the healing that happens within your brain all compound over time. Yes, nearly half leave treatment before that one-year mark, but you have the power to be in that 54% who stick with it. Pairing clinical intervention with compassionate care plus proven therapeutic approaches gives you the best possible chance at long-term success.
4. Overdose Deaths Dropped 26% in Just One Year
The numbers tell a story of hope that’s hard to ignore. Between 2023 and 2024, overdose deaths across the United States dropped by 26% – the largest single-year decline ever recorded, according to CDC drug overdose data5. That’s not just a statistic; it’s thousands of lives saved, families kept together, and communities beginning to heal. If you’ve been struggling with opioid addiction, this data shows that recovery is possible, and more people are finding their way through than ever before.
This dramatic shift didn’t happen by accident. It’s the result of expanded availability of medications for addiction treatment (MAT), wider distribution of naloxone to reverse overdoses, and increased awareness about treatment options. Combining prescription medications with therapeutic counseling – the foundation of effective MAT programs – gives you the best chance at sustainable recovery. The research is clear: comprehensive care works.
The Role of Naloxone in This Decline
Alongside MAT, the widespread availability of naloxone (Narcan) has been a critical safety net. It rapidly reverses opioid overdoses, giving individuals a second chance to seek comprehensive treatment and begin their recovery journey.
What makes this decline even more meaningful is that it happened across nearly every state and affected multiple substances, including fentanyl-related deaths. You’re part of a larger movement toward recovery, with infrastructure to support you that’s stronger than it’s ever been. Medical detox facilities are now better equipped to handle complex withdrawal safely, while follow-up programs help you maintain progress after those critical first days.
Every step you take toward treatment contributes to this positive trend. Your path forward matters – not just to you and your loved ones, but as part of a nationwide shift proving that addiction can be overcome with proper support, compassion, and scientifically proven care.
5. Racial Disparities Create 3-9% Access Gaps
Reaching medication-based therapies isn’t equal for everyone, and that’s something we need to talk about honestly. Research shows that racial disparities create gaps ranging from 3% to 9%, meaning some communities face significantly harder barriers to getting the help they deserve, as detailed in Medicare access research10. These aren’t just numbers—they represent real people struggling to reach life-saving interventions.
Black and Hispanic individuals are substantially less likely to receive buprenorphine or methadone compared to white individuals, even when they have similar insurance coverage and live in the same areas. Part of this comes down to where treatment centers are located, with fewer facilities operating in predominantly minority neighborhoods. But location is only part of the story.
Cultural barriers, language differences, and past experiences with healthcare systems that didn’t always treat everyone fairly can make it harder to take that first step. When you’ve faced discrimination or felt misunderstood in medical settings before, reaching out for help requires even more courage. And that courage deserves to be met with compassionate, accessible care.
The good news? Awareness is growing, and facilities are working to bridge these gaps. Look for treatment programs that actively welcome diverse communities, offer culturally responsive care, and have staff who understand different backgrounds and experiences. Everyone deserves equal opportunities for scientifically proven interventions that combine clinical care, therapy, and behavioral support—regardless of race, ethnicity, or zip code. The path ahead matters, and finding a place that truly sees you as an individual can make all the difference as you heal.
6. MAT Creates $8,000-$212,000 in Benefits
When weighing whether this pharmacological approach is worth pursuing, understanding the real-world value can make your decision clearer. Research shows that MAT generates substantial economic benefits—between $8,000 and $212,000 per person over time, as shown in economic benefit analyses9. These numbers reflect reduced healthcare costs, fewer emergency room visits, decreased criminal justice involvement, and increased productivity as you rebuild your life in recovery.
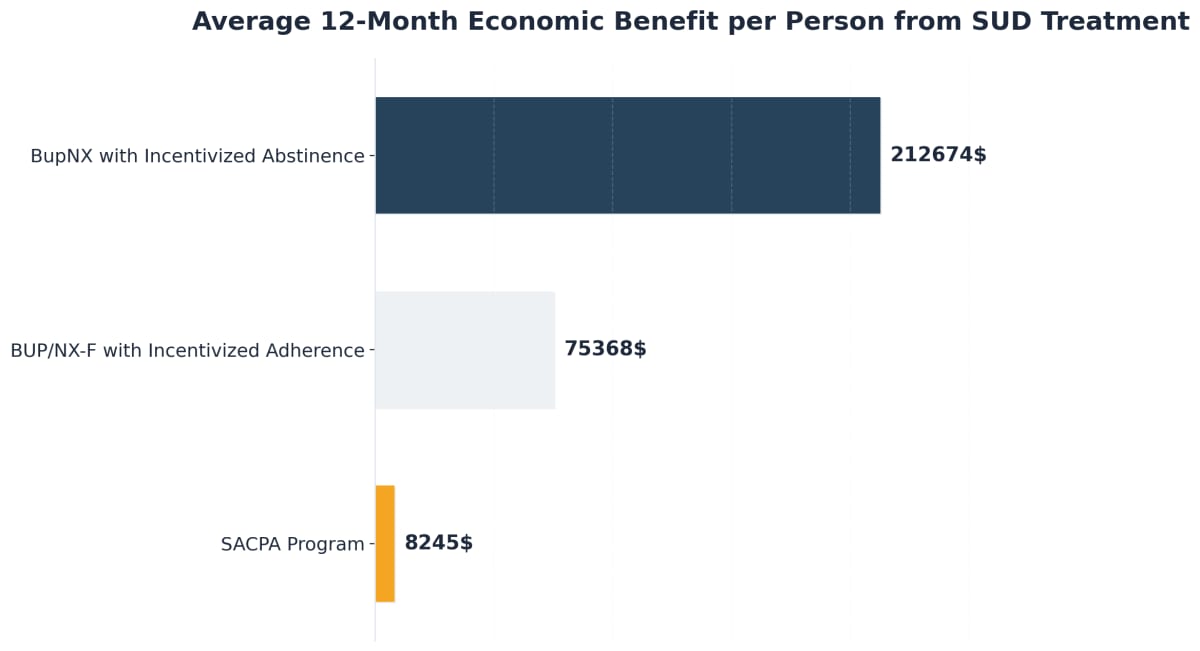
“The financial impact matters because it demonstrates how effective MAT truly is. Combining medications like methadone or buprenorphine with therapeutic support does more than manage withdrawal symptoms—it’s investing in a proven approach.”
Every day you remain in recovery means avoiding expenses that active addiction creates throughout your life and community. These benefits extend beyond dollars and cents. MAT helps you regain stability, reconnect with family, return to work, and rediscover purpose.
Pharmacological interventions address physical aspects of opioid dependence while therapy supports emotional and behavioral changes necessary for lasting recovery. This comprehensive approach is why facilities offering research-supported care emphasize combining medical supervision with clinical therapy—because that combination produces measurably better outcomes.
Yes, starting treatment takes courage, and that’s completely understandable. But knowing that MAT creates real, documented value in people’s lives can provide reassurance as you take this important step. You deserve treatments that work, and strong evidence supports MAT as one of most effective tools available for overcoming opioid dependence.
7. Extended-Release Options Improve Medication Assisted Treatment Statistics
Extended-release formulations of buprenorphine represent a significant advancement in your recovery journey. Unlike daily medications that require remembering doses every single day, extended-release options like Sublocade provide steady medication levels for an entire month with just one injection. This consistency matters because it eliminates daily ups and downs that can trigger cravings and make recovery feel harder than it needs to be.
Research shows that extended-release buprenorphine significantly improves treatment retention rates compared to daily sublingual films or tablets, according to retention strategy reviews6. Without daily dosing concerns, you’re free to focus on therapy components that help build lasting coping skills. You’re addressing physical dependency while simultaneously working on psychological aspects during recovery—and that combination is what creates real, sustainable change.
Monthly injection format also removes some stigma and logistical challenges that come with daily medication. You don’t need to carry medication with you, worry about lost prescriptions, or navigate daily routines that can feel like constant reminders of struggle. Instead, you visit your treatment provider once a month, receive an injection, and continue building the life you deserve.
Extended-release options work particularly well combined with comprehensive support services like individual therapy, group sessions, and aftercare planning. This integrated approach addresses your whole person—not just physical symptoms related to dependency—giving you tools and confidence to move forward with hope and determination.
Frequently Asked Questions
How did we choose which MAT statistics to include in this list?
We focused on medication assisted treatment statistics that show the biggest challenges—and the most meaningful progress—facing people in recovery. Every number was chosen for its real-world impact, like how many actually get access to medication, changes in overdose deaths, and who remains in treatment after a year. These statistics come from large federal studies and peer-reviewed research, so you can trust that they reflect what’s happening on the ground 145. Our goal was to highlight data that matters for your day-to-day work supporting others and advocating for better outcomes.
What should I do if I’m in the 75% who haven’t accessed MAT yet?
If you’re among the 75% who haven’t accessed medication-assisted treatment yet, it’s okay to feel frustrated or overwhelmed—those feelings are valid. Start by reaching out to a trusted healthcare provider or addiction specialist to discuss your options and any barriers you’re facing. Sometimes, stigma or not recognizing the need for help can get in the way, but you’re not alone: nearly 43% of people who could benefit from MAT didn’t even realize they needed treatment 1.
Every step forward counts, even if it’s just gathering information or talking with someone supportive. Ask about telemedicine, insurance coverage, or local programs. Remember, progress is possible and you deserve support.
Why wasn’t data about naltrexone retention rates included in this list?
Great question—data about naltrexone retention rates wasn’t included here because most large studies and reviews show that naltrexone, especially the oral form, has much lower retention compared to methadone or buprenorphine. Extended-release naltrexone can help some people, but real-world studies find higher rates of early dropout and challenges with starting treatment, since you need to be opioid-free for 7–14 days first 62. That means the most reliable medication assisted treatment statistics focus on methadone and buprenorphine, where retention and outcomes are stronger and more consistent.
Can I switch between methadone and buprenorphine if one isn’t working?
Yes, you can switch between methadone and buprenorphine if one isn’t working for you—but it’s a process that should be done with medical supervision and careful planning. Transitioning from methadone to buprenorphine usually requires tapering your methadone dose down to a lower level (often below 30 mg/day) before starting buprenorphine, to avoid withdrawal symptoms. Going from buprenorphine to methadone can be smoother, since methadone can be started at a low dose and increased as needed 2. Everyone’s journey is unique, so don’t be discouraged if you need to adjust your approach. Talk openly with your provider about your symptoms and goals—switching medications is a valid step forward if it helps you stay engaged in treatment and recovery.
How does telemedicine access affect my chances of staying in treatment?
Telemedicine access can make a real difference in your ability to stick with medication-assisted treatment. Recent reviews show that virtual care is just as effective as in-person visits when it comes to keeping people engaged in MAT—and for many, the convenience removes big barriers like transportation and stigma 6. When you can meet with your provider from home, it’s often easier to stay on track, especially during tough stretches or if you have a busy schedule. Medication assisted treatment statistics suggest that when telemedicine is available, retention rates hold steady or even improve, helping more people reach their recovery goals. Remember, choosing flexible care options can be a small win that adds up over time.
What happens to my recovery if I stop MAT after completing treatment?
Stopping medication-assisted treatment (MAT) after completing your program can bring up a mix of relief and worry. The research shows that risk of relapse and overdose goes up after leaving MAT—even if you’ve done well during treatment 8. Your body’s tolerance drops, so if you return to opioid use, the chance of overdose is higher. Many people feel strong cravings or emotional ups and downs in the weeks and months after stopping.
The best outcomes happen when you transition off MAT with medical support and continue counseling, peer groups, or aftercare. Medication assisted treatment statistics remind us: ongoing support matters for long-term success 6. You’re not alone in facing these challenges—every step to protect your progress is worth celebrating.





